This post was written directly by Gangnam New N Dental Clinic and
in strict compliance with Article 56 of the Medical Service Act and the regulations related to medical advertising review.
Through our clinic blog content, we provide medical information
that may be helpful to an unspecified number of patients.
The Cause of Stomatitis: Fatigue and Nutrition
The Unwelcome Guest in Your Mouth Brought on by Imbalance
| Summary |
|---|
| 1. Stomatitis most commonly occurs when physical fatigue accumulates, such as from weakened immunity, vitamin deficiency, and stress. |
| 2. Physical irritation or injury, such as biting the inside of the cheek or getting burned by hot food, can lead to a bacterial infection and cause inflammation. |
| 3. Depending on the symptoms, it is classified into aphthous (ulcerative) and herpetic (vesicular) types, each with different treatments. |
| 4. Getting enough rest and consuming nutrients such as vitamin B12, iron, and folate are essential for prevention and recovery. |
| 5. If symptoms persist for more than two weeks or the pain is severe, it may be a sign of another systemic disease rather than simple stomatitis, so an accurate diagnosis is needed. |

Hello,
This is New N Dental Clinic.
When you are tired or under severe stress, there is an unwelcome guest that always seems to appear.
It is stomatitis, the condition in which white sores appear on the mucous membrane inside the mouth. Why does this condition make even eating a single spoonful of rice painful? Is it simply due to a vitamin deficiency, or is there another reason?
Today, we will take a closer look at the fundamental causes of stomatitis, which can significantly lower your quality of daily life, and how to respond depending on the type.




Previous image
Next image
Key causes that trigger stomatitis

Weakened immunity and excessive fatigue
This is the most typical cause of stomatitis. A wide range of bacteria always live in our mouths, but when the body’s immune system is functioning normally, they do not cause any problems.
However, when immunity weakens due to overwork, staying up all night, or stress, the oral mucosa’s ability to regenerate declines, making it vulnerable to bacterial attack and leading to inflammation.
Nutritional imbalance
When certain nutrients are lacking, the oral mucosa becomes weaker.
-
B vitamins: Stomatitis is more likely to develop, especially when B2, B6, and B12 are deficient.
-
Iron and folate: When nutrients needed for blood production and cell regeneration are insufficient, the mucosa becomes thinner and ulcers are more likely to form.
Oral hygiene and irritating ingredients
Surfactant ingredients in toothpaste can irritate the oral mucosa and cause inflammation, and stomatitis can also develop easily when dry mouth prevents saliva from properly carrying out its antibacterial function.
What kind of inflammation do I have inside my mouth?
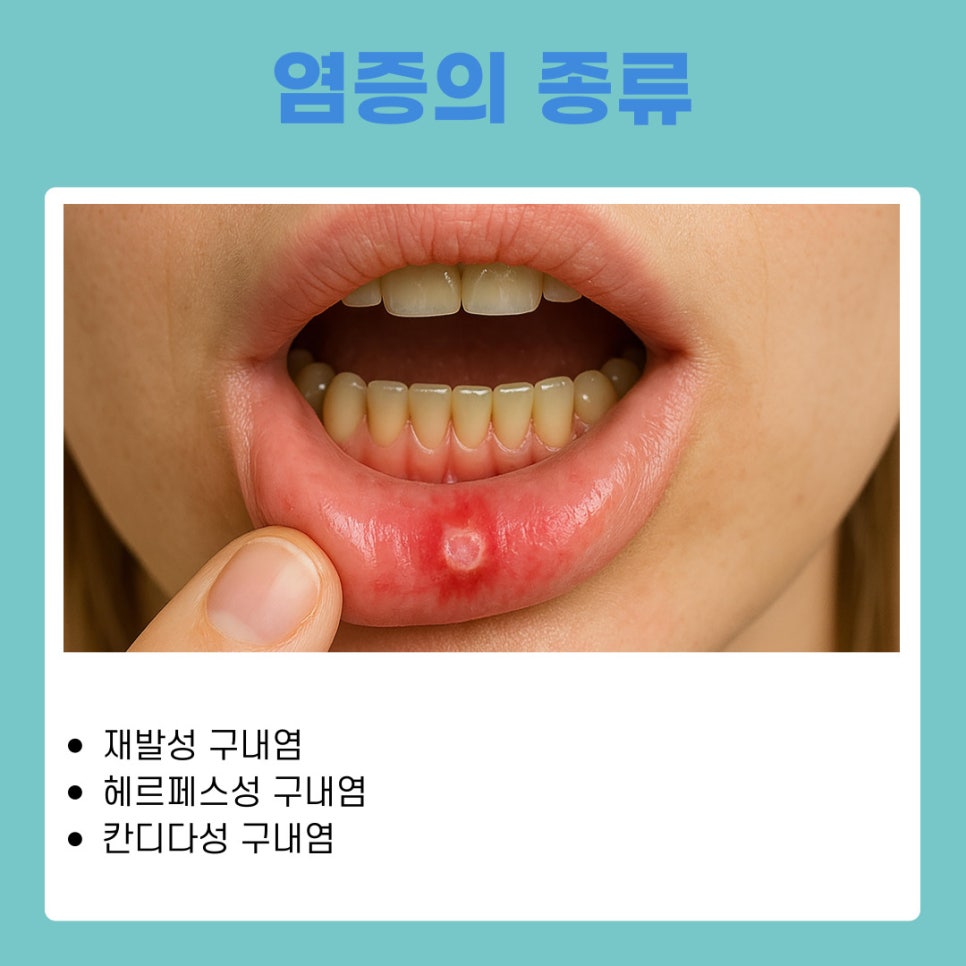
Stomatitis is divided into different types depending on its appearance and cause. Check your own condition.
-
Recurrent stomatitis: The most common form. One or two round, white ulcers appear, and the pain is severe. It is usually caused by weakened immunity.
-
Herpetic: Multiple small blisters appear around the lips or on the roof of the mouth. It is a viral disease and is contagious, so caution is needed.
-
Candidal: It looks like a white membrane has formed inside the mouth, and it is a fungal infection that occurs in elderly or frail people whose immunity has dropped sharply, or in those who have taken antibiotics for a long period of time.
How to help stomatitis heal faster

-
Maintain oral cleanliness: Even if it hurts, brush your teeth thoroughly and use salt water or a low-irritation mouthwash to prevent bacteria from multiplying in the mouth.
-
Medication: When the pain is severe, use a chemical antiseptic, an ointment-type treatment, or a patch-type medicine to relieve pain and protect the affected area.
-
Nutritional supplementation and rest: Get enough sleep and take a multivitamin to improve your body’s recovery capacity.
When you need to visit a dental clinic

In general, stomatitis heals on its own within 1 to 2 weeks. However, you may need medical care if you have any of the following symptoms.
-
If the inflammation lasts for more than 2 weeks or gradually gets larger
-
If you have a fever or severe overall fatigue
-
If stomatitis spreads throughout the mouth, making it impossible to eat
-
If frequent recurrent stomatitis is accompanied by eye pain or inflammation around the genitals

Q. When stomatitis develops, is applying a liquid medicine the best method?
A. Liquid medicine chemically burns the inflamed area to kill bacteria and forms a protective film. It is painful to apply, but it has the advantage of allowing faster recovery.
However, it is not effective for all types of stomatitis. It may be less effective for viral or fungal stomatitis, and if used on a wound that is too large, it can instead damage the surrounding tissue.
If the symptoms are mild or the affected area is wide, it is better to first use an ointment with less irritation, and when rapid pain relief is needed for a localized area, it is advisable to selectively use liquid medicine.









