
When you first decided to have plastic surgery, you probably had a lot of anticipation and excitement.
The wish to see an improved version of yourself in the mirror is completely understandable.
But as time goes by, if you suddenly look in the mirror and think, “Something looks off about my nose,” or “It feels more stuffy and uncomfortable than before,” that may not be just your imagination.
The nose is the center of the face, but it is not simply an organ for looking beautiful; it is also a very important area responsible for breathing.
However, in the past, because the focus was only on aesthetic standards such as a “high and sharp nose” or a “celebrity nose,”
there were not a few cases where surgery was performed by inserting implants that were too large or removing necessary tissue too aggressively.
These surgeries may look fine at first, but they can cause problems over time.
The bridge may look bent or sharply angled, the tip may be lifted too much so the nostrils show, the skin may become thinner and reveal the implant underneath, and in some cases even breathing becomes uncomfortable.

When these functional problems begin in addition to the appearance issues, many people only then start searching for the term “nose reconstruction.”
But “reconstruction” is not simply fixing the nose again.
It is more accurate to see it as a delicate revision surgery that precisely identifies damaged bone or cartilage, thinned skin, and a collapsed structure, then restores both shape and function at the same time.
In this article, I will explain in detail when nose reconstruction is needed and the key points you should check before surgery.
When is nose reconstruction needed?

The situations in which nose reconstruction is needed are more varied than you might think.
That is because the issue often goes beyond simply not liking the shape and is accompanied by structural damage or reduced function.
Typical examples include cases where an implant is visible from a previous surgery, or the tip of the nose has been lifted too much so that the nostrils are overly exposed.
Problems such as a bent nasal bridge or a nose that looks crooked can also become serious reconstruction cases.
In addition, if cartilage has been absorbed over time or tissue has been damaged due to inflammation, nose reconstruction should also be considered.
Also, if breathing has become difficult after surgery, this is not just a cosmetic issue but can be seen as functional damage, so prompt diagnosis is needed.
At moments when it must become a surgery not “to look better” but “to live comfortably,” nose reconstruction should be seriously considered.



Key points you must check before nose reconstruction surgery
- How much damage there is — an accurate diagnosis comes first.
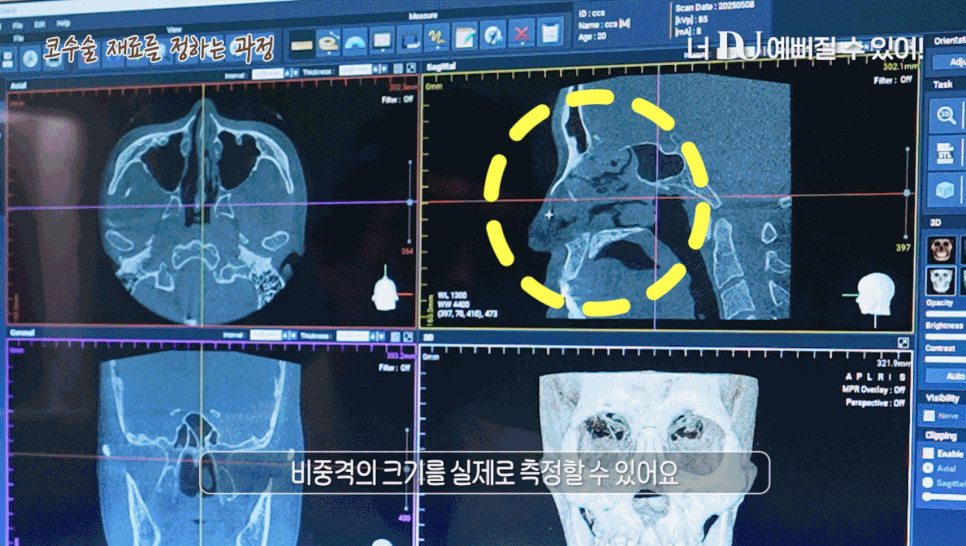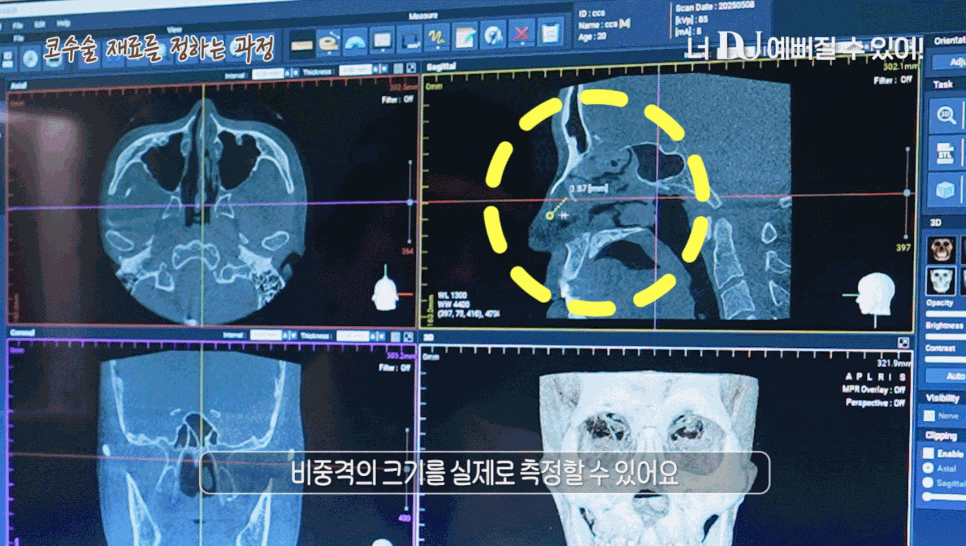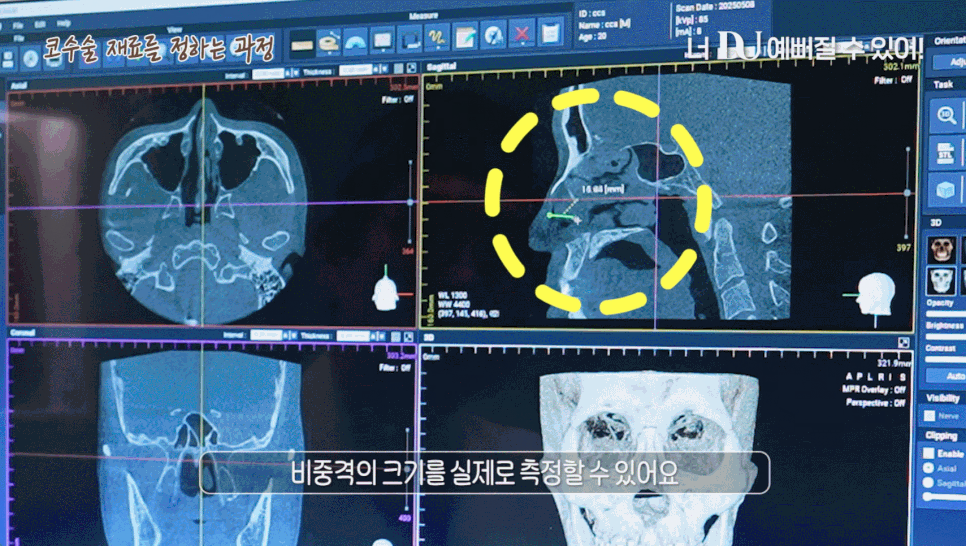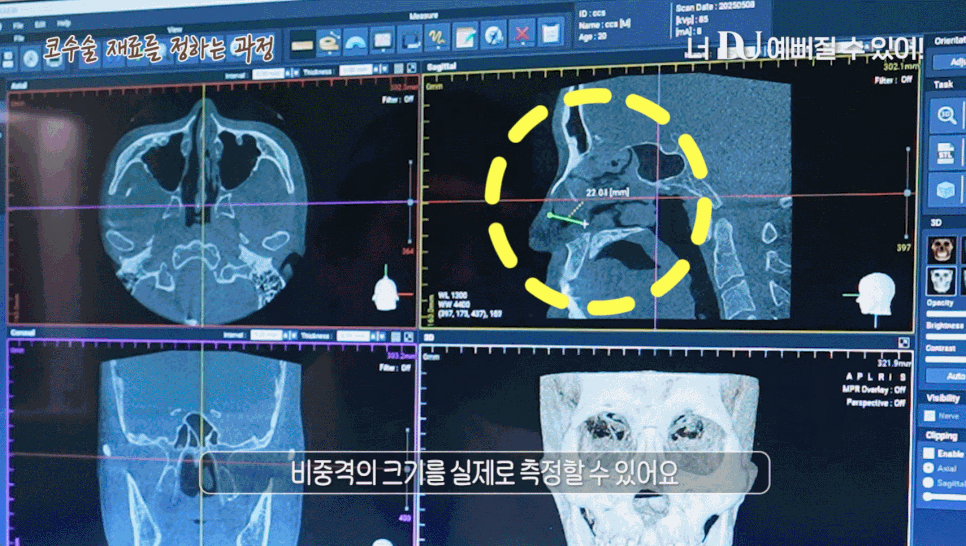
Nose reconstruction surgery does not simply improve appearance; it begins with a precise analysis of the current condition of the nose.
Because the internal structure of the nose is difficult to see from the outside, it is hard to identify the exact problem based only on the feeling that “it seems a little more strange than before.”
At this time, the most useful tool is a 3D CT scan.
It allows the cross-sections to be checked three-dimensionally from multiple angles, making it possible to precisely examine the implant position, cartilage absorption, deformation of the nasal bone, and even deviation of the septum.
Sometimes damage caused by inflammation or changes in skin thickness must also be considered, so diagnosis that looks at the entire structure—not just the surface—is essential.
Because nose reconstruction is a surgery that solves problems of “structure” rather than “appearance,” the depth of diagnosis itself must be different.

- It is not simply a surgery to “put something in again” or “take something out.”
Reconstruction is not a simple revision surgery.
This is because the approach changes completely depending on which tissues were damaged in the previous surgery, what materials were used, and how much adhesion has occurred.
In particular, when the nasal tip has collapsed or the implant has pushed up against the skin and become visible, autologous tissue such as ear cartilage, rib cartilage, or septal cartilage often needs to be grafted to protect the thinned skin and rebuild the structure.
Cartilage is not merely used to fill space; it is like a “design material” that restores a collapsed support structure and stabilizes the shape.
On top of that, the condition of the skin and the flexibility of the nasal mucosa inside the nose also need to be considered, so this is not a surgery that can be solved simply by removing the existing implant and inserting a new material.
To avoid repeating a failed surgery, a far more complex plan and surgical strategy than the first one is needed.

- Previous medical history, surgical history, and whether there was inflammation must also be carefully understood.
One of the biggest reasons nose reconstruction surgery is difficult is that the tissues have already been altered by previous surgery.
If cartilage has been absorbed or the tissue has hardened and adhesions are severe, the risk of bleeding or tissue damage during surgery increases, and the recovery period inevitably becomes longer.
Also, if there was a past infection or a foreign-body reaction caused by an implant, special caution is needed so that the same problem does not recur in the new surgery.
In such cases, a reconstruction strategy centered on treatment and recovery, rather than a simple cosmetic purpose, is needed.
Therefore, nose reconstruction must be decided only after sufficient consultation and examination with medical staff experienced in this field, and it is the first step toward a safe surgery to carefully check the doctor’s experience, surgical cases, and preoperative diagnostic system.

Nose reconstruction may sound like a difficult and frightening topic, but in fact it is about honestly facing your current discomfort and making a second choice for a better you.
When you first had surgery, you were probably driven by a single wish to become prettier, but as time passes, if one day the face in the mirror feels unfamiliar and even breathing becomes uncomfortable, that may be a signal from your body rather than your mind.
Looking better is important, but a face that can breathe comfortably and smile naturally is even more valuable.
Nose reconstruction is not simply a surgery to fix something again; it is closer to a journey of “recovery,” carefully rebuilding a structure that once collapsed.
If you are with medical staff who sincerely listen to your story and carefully examine everything from structure to function, you will likely be able to return to a much healthier and more natural appearance than you have now.
Do not just brush off the discomfort you feel now; please start today by taking the first step toward regaining your “truly you” appearance.
Thank you.













