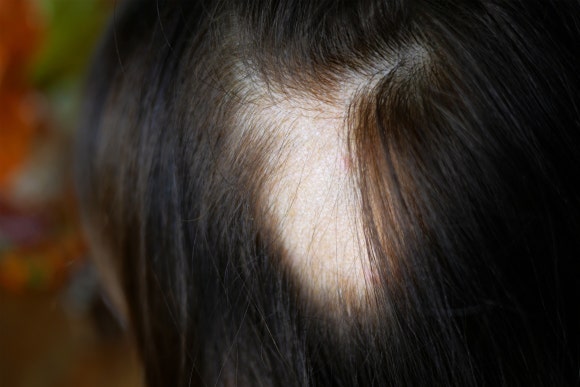
Alopecia areata is often thought of simply as a skin condition that causes hair loss, but in reality, it is closely related to patients’ mental health as well.
In a recent large-scale U.S. cohort study, more than 90,000 patients with alopecia areata were followed for one year, and the incidence of anxiety and depression was clearly identified¹.
In this post, I will explain the study results and their clinical significance in a FAQ format that patients often ask about.
Q1. How often do anxiety and depression occur in patients with alopecia areata?

According to the study, within one year after diagnosis of alopecia areata, the rate of newly developed anxiety was about 3.6%, and depression was 1.6%.
These numbers may look low at first glance, but they are relatively high compared with the general population, and once symptoms begin, they tended to recur more than twice on average¹.
In actual practice, because of the sudden onset and tendency to recur, many patients live in constant tension, worrying that the hair loss will happen again, which can worsen anxiety.
Q2. Why is alopecia areata connected to mental health problems?
The cause can be explained from two major perspectives.
Psychological and social factors
Because the hair loss is visible, patients often avoid being seen and reduce social interactions, which can lead to greater social isolation.
In particular, when the eyebrows or eyelashes are affected, facial expressions change and patients may even feel a loss of identity.
Immunological and neurological factors
Inflammatory cytokines involved in the pathophysiology of alopecia areata (IL-6, TNF-α, IFN-γ) also affect brain neurotransmitter metabolism.
IL-6 strengthens the stress response, and TNF-α interferes with serotonin synthesis, worsening depression².
In other words, it means the skin and the brain are connected within one network.
Q3. Which patients feel a greater psychological burden?
Mental health problems are especially likely to accompany the following cases¹.
- When the eyebrows or eyelashes are also involved
- Patients with frequent recurrences
- Patients with extensive lesions
For these patients, the anxiety caused by the hair loss itself is compounded by reduced self-esteem in daily life and interpersonal problems, increasing the risk.
Q4. Do patients with alopecia areata need a mental health checkup?
It is recommended. At the time of the initial diagnosis, it is helpful to assess anxiety and depression with a simple psychological questionnaire, and then follow up at 3, 6, and 12 months.
Early intervention is especially important for patients with extensive lesions or frequent recurrences.
Not missing small warning signs is the way to protect not only treatment outcomes but also quality of life.
Q5. What treatment approach is effective?
A multidisciplinary approach is the most effective.
- Treatment (medication, injections, etc.)
- Psychological counseling and cognitive behavioral therapy
- Peer support groups (gatherings where people share the same experience)
Using these three approaches together can increase the chances of recovery.
In fact, patients who regain the feeling that they are “not alone” through counseling or group participation often appear much more stable during treatment.
Alopecia areata: why does it also bring mental distress?
Conclusion
Alopecia areata is not just a matter of hair; it is a condition in which the body and mind are connected.
Because anxiety and depression can easily follow, an approach that also looks after the patient’s mental health is needed.
Psychological screening, regular monitoring, and multidisciplinary collaborative treatment can be key strategies for protecting quality of life.
Alopecia areata: why does it also bring mental distress?
Summary table
| Item | Main findings |
|---|
| Number of participants | 91,302 |
| Mean age | 49 years |
| Female proportion | 72.06% |
| Anxiety incidence within 1 year | 3.6% (mean 2.057 episodes) |
| Depression incidence within 1 year | 1.6% (mean 2.136 episodes) |
| Event-free survival rate (anxiety) | 96.38% |
| Event-free survival rate (depression) | 98.13% |
| Risk factors | Eyebrow/eyelash involvement, recurrent/extensive alopecia areata |
| Recommended measures | Initial and regular psychological screening, multidisciplinary treatment, accessibility assessment |
Now it is time for hairhair to grow, this was Kim Jin-oh.
Filsaengsinmo (必生新毛).

Written by: Kim Jin-oh of New Hair Plastic Surgery Clinic (Public Relations Director, Korean Association of Plastic Surgeons / Academic Director, Korean Hair Research Society)
References
Chew, A-L., et al. (2025). Beyond hair loss: Exploring the psychiatric burden of alopecia areata in a large cohort. Journal of the National Medical Association.
[This post is written directly by a board-certified plastic surgeon for informational purposes in accordance with Article 56, Paragraph 1 of the Medical Service Act. Hair transplant surgery and treatment may have side effects, and they should be decided carefully through consultation with a specialist.]


