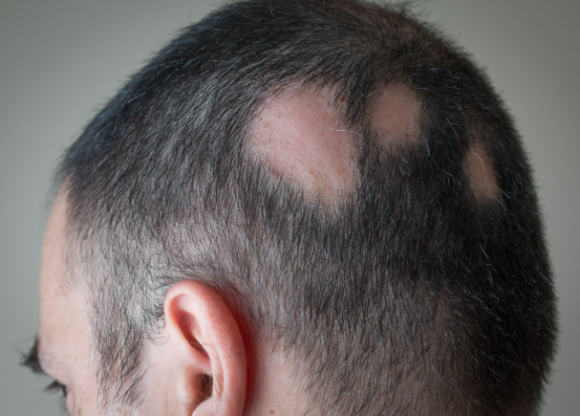
Alopecia areata
Source - Health Joongang
“Maybe it’s because I’ve been under a lot of stress lately.”
This is the phrase that patients with alopecia areata say most often.
Most people who notice a coin-sized patch of hair loss think, “It’ll probably grow back soon,” and move on.
But recent research completely overturns this common belief.
Alopecia areata is not a simple stress-related reaction, but an autoimmune disease caused by immune imbalance, and spontaneous recovery is difficult to expect¹².
In the past, treatment relied on steroid injections or topical medications, but now the field is shifting toward an era of treating the root cause by regulating the immune response itself³.
Based on the latest medical data, we have clearly organized the likelihood of natural recovery in alopecia areata, treatment methods,
and personalized strategies for each patient.
Alopecia areata: Will it get better if you leave it alone?
How likely is natural recovery? Summary
Alopecia areata is a much more complex condition than simply saying, “It happened because of stress.”
According to the latest research, completely recovering without treatment occurs in only 1–3% of cases¹, because the hair follicle is damaged by an autoimmune response².
Recently, approaches that restore immune balance and reduce recurrence through new JAK inhibitor drugs and combination treatment with PRP and PDRN have been drawing attention³⁴⁵.
Q1. Won’t alopecia areata just get better if stress is reduced?
People used to believe that, but recent research shows that the natural recovery rate is less than 10%.
According to a 2025 meta-analysis in Acta Derm Venereol¹, among untreated
patients, complete recovery was 1–3%, and partial recovery was below 8%.
Unlike simple stress-related hair loss, this is an autoimmune disease in which immune cells attack the hair follicle².
Simple rest or improved sleep alone cannot address the underlying cause of the disease.
| Category | Natural recovery rate | Main cause | Need for treatment |
|---|
| Stress-related hair loss | About 80–90% | Temporary stress, fatigue | Can improve with lifestyle changes |
| Alopecia areata | 1–3% complete recovery | Autoattack by immune cells | Treatment required |
Q2. Why does alopecia areata happen?
The cause is immune imbalance.
A normal hair follicle is surrounded by a protective barrier called immune privilege, so it is not attacked by immune cells.
However, when this protective barrier breaks down, T cells recognize the hair follicle as an enemy and trigger an inflammatory response².
When inflammatory signals in the body are repeated at this time, the area of hair loss expands and the risk of recurrence increases. In the end, the key is not “suppressing inflammation,” but restoring immune balance.
Q3. What treatment is most effective these days?

Baricitinib
Source - Drug Information Center
The core of the latest treatment is JAK inhibitors.
These drugs block excessive immune signaling (the JAK-STAT pathway) and suppress the activity of immune cells that attack the hair follicle³.
Starting with baricitinib, which was approved by the U.S. FDA in 2022, new drugs such as ritlecitinib and deuruxolitinib have been developed one after another⁴⁵.
In European studies, about 40% of patients taking baricitinib showed marked recovery within 9 months, and more than half maintained the effect even after stopping treatment⁴.
| Drug name | Main mechanism | Approval year | Clinical result |
|---|
| Baricitinib | JAK1/2 inhibition | 2022 (FDA) | 40% recovery within 9 months⁴ |
| Ritlecitinib | Selective JAK3 inhibition | 2024 (KFDA) | Effective in moderate to severe patients |
| Deuruxolitinib | JAK1/2 inhibition | 2025 clinical completion | Stable hair regrowth |
Q4. Are there treatments that can be combined with medication?
Depending on the patient’s condition, combination treatment for immunity and regeneration can be effective.
-
Local steroid injections: suitable for early-stage or localized lesions
-
Immunotherapy (such as DPCP): used in chronic, recurrent alopecia areata
-
PRP / PDRN injections: relieve inflammation and promote hair follicle regeneration
-
Botulinum toxin: relieves scalp tension and improves blood flow
-
Nutrition and diet therapy: vitamin D, zinc, and iron supplementation, and improved gut health
In a reported case, combining baricitinib and PRP led to visible hair regrowth within 6 months, and even eyebrow recovery by 9 months⁴.
Q5. Are there any side effects or precautions during treatment?
JAK inhibitors are safer than conventional immunosuppressants, but regular blood tests are essential.
Increases in cholesterol and infection risk have been reported, but most cases are mild and have been confirmed to be manageable at less than 5%³.
In the end, the key to treatment success is not “which drug to use,” but “when to start.”
The earlier the intervention, the higher the chance of reversing hair follicle damage.
Alopecia areata: Will it get better if you leave it alone?
How likely is natural recovery? Conclusion
Alopecia areata is not a simple problem that can be solved by “just reducing stress.”
The chance of natural recovery is less than 1 in 10, and only early treatment that restores immune balance is the path to reducing recurrence.
With the development of JAK inhibitors and regenerative treatments, treatment outcomes have improved to the point where complete recovery can now be expected within 9–12 months.
Rather than waiting, starting now—that decision changes the speed of hair recovery.
Now it’s time for hairhair, Kim Jin-oh.
Philsaengsinmo (必生新毛).
Written by: Kim Jin-oh of New Hair Plastic Surgery (Public Relations Director, Korean Association of Plastic Surgeons / Academic Director, Korean Society for Laser, Dermatology and Hair)
References
1.Jastrząb-Miśkiewicz B, Szepietowski JC, Saceda Corrallo D, Krajewski PK. Is spontaneous regrowth in alopecia areata possible: a systematic review and meta-analysis of placebo-controlled studies. Acta Derm Venereol. 2025;105:adv44153.
2.Rudnicka L et al. European expert consensus statement on the systemic treatment of alopecia areata. J Eur Acad Dermatol Venereol. 2024;38:1234–1245.
3.Harries MJ et al. British Association of Dermatologists living guideline for the management of alopecia areata. Br J Dermatol. 2025;192(2):190–214.
4.Youssef Z, Ennaciri M-A, Frikh R, Hjira N. Baricitinib in the management of severe alopecia areata: a report of two cases with sustained clinical response. Cureus. 2025;17(10):e94278.
5.Sánchez K et al. Evaluating current and emergent JAK inhibitors for alopecia areata. Front Immunol. 2025;16:1621492.
[This post is written directly by a board-certified plastic surgeon for informational purposes in accordance with Article 56, Paragraph 1 of the Medical Service Act. Hair loss surgery and treatment may have side effects, and you should make a careful decision after consulting with a specialist.]


