Anyone who is a woman wants to have a beautiful
body shape.
Simply showing
the volume of the breasts
can have a positive effect on the
overall body line and impression.
Interest in breast surgery, which can complete the volume and
line that suit one’s body type, continues to rise.
Although satisfaction after breast augmentation surgery is
generally high, some people undergo
revision surgery because of capsular contracture,
which causes the breasts to become firm.
Today, we will talk about the likelihood of breast capsular contracture and
the factors that should be considered in order to safely undergo
a revision surgery that requires a higher level of technical skill
than the first surgery.
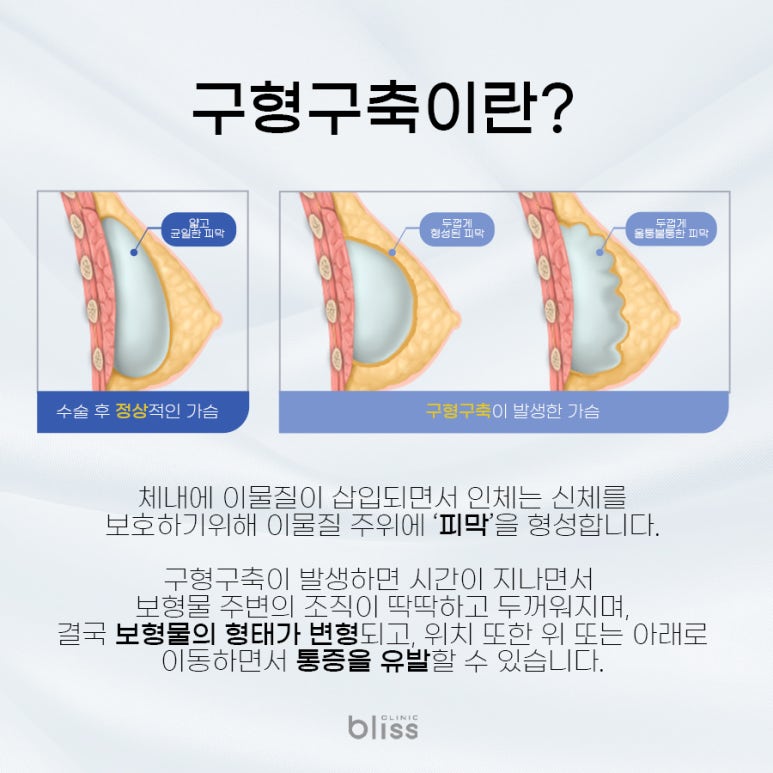
What is breast capsular contracture?
The likelihood of breast capsular contracture occurring
depends on the type of implant, surgical method, and the patient’s individual
condition, but recent studies have reported approximately 4.3% to 14.6%
within 10 years.
When our body reacts to an implant, which is a foreign substance,
a normal defense response occurs in which a capsule forms around it.
However, over time this capsule
gradually contracts and becomes excessively thick,
causing it to harden or the implant to become deformed,
resulting in a distorted shape.
If the breast becomes firm, its shape changes,
and the movement of the implant becomes uncomfortable,
breast capsular contracture may be suspected.

Causes of capsular contracture
The main causes of breast capsular contracture
can include inflammatory reactions in the breast tissue,
blood pooling due to bleeding,
foreign substances entering around the implant,
the type or surface characteristics of the implant, and an individual’s constitution,
all acting together.
First, in the case of an inflammatory reaction in breast tissue,
microorganisms may contaminate the implant surface during surgery,
and as those bacteria repeatedly
stimulate the tissue, a biofilm forms,
causing the capsule to thicken.
Biofilms have the characteristic of not responding well
to antibiotics, so a low-grade infection that is not visible to the eye
can continue for a long period of time.
In particular, skin commensal bacteria such as
Staphylococcus epidermidis are pointed to as major causative organisms.
In addition, if a hematoma forms when blood that occurs during or after surgery pools,
it can become a breeding ground for bacteria,
and if seroma, in which fluid accumulates around the implant,
repeats, it can cause capsular contracture.
Before planning revision surgery for breast capsular contracture,
it is good to check whether the clinic can provide an accurate diagnosis
and establish the proper surgical method so that the same outcome as the previous surgery does not recur,
and whether a systematic aftercare system is in place.
To achieve natural and desired results, it is important to check whether follow-up care
for scar management and infection prevention is well established.
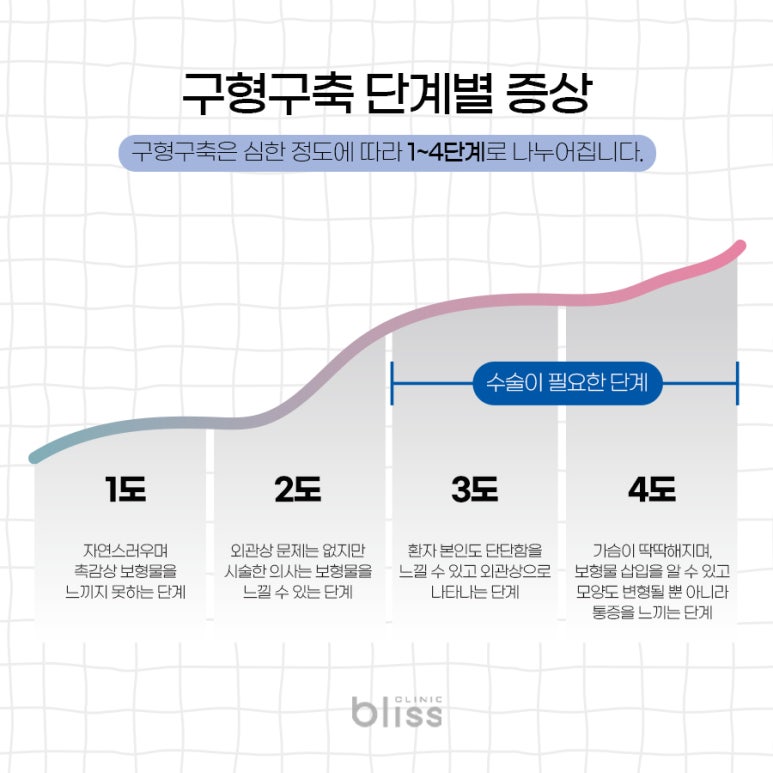
Diagnosis by stage of capsular contracture
Capsular contracture is usually classified into 4 stages (Baker’s classification).
Stage 1: A very mild degree, to the point that no abnormality is felt
Stage 2: No visible problem, but the implant begins to feel slightly firm; usually not noticed by the patient, but detectable by medical staff
Stage 3: Firm enough to be felt by the patient and also visible to others
Stage 4: Very firm with pain, and the change in shape is obvious to anyone
A diagnosis of capsular contracture is mainly made through
palpation, but because assessment may differ by clinic,
an ultrasound examination should be performed to confirm the thickness of the capsule,
the condition of the implant, and whether there is rupture, and then the capsule should be removed together with
the implant, or breast revision surgery should be performed.

The need for revision surgery for capsular contracture
The decision to undergo revision surgery for breast capsular contracture
should be made after considering various factors.
In general, if symptoms of capsular contracture at stage 3 or higher
are suspected, revision surgery is considered.
Problems with the implant itself are also an important
criterion for judgment.
If the implant has ruptured,
has aged due to being old,
or can be felt and shows wrinkling due to rippling,
implant replacement is necessary. In addition, if the external appearance is unsatisfactory,
or if there is noticeable asymmetry in the size and shape of both sides,
revision surgery may be considered.
Because these factors differ from person to person,
it is necessary to make a decision through consultation with a specialist by comprehensively considering the degree of the individual’s symptoms,
aesthetic satisfaction,
and psychological impact.

Why Bliss Clinic is the right choice
Plastic surgery specialist Director Oh Doo-young
provides safe surgery and 1:1 customized design based on
experience gained through countless cases of breast surgery and revision surgery.
From preoperative consultation to aftercare,
we provide personalized medical services that consider each patient’s body type,
skin condition, and desired line through an individual system,
allowing you to achieve satisfying changes.
After surgery, a private single recovery room is provided to reduce the risk of infection
and allow comfortable recovery,
providing fast recovery and stability.