Hello, this is S Leader Dental Hospital, Konkuk Univ. Entrance Dental Clinic, now in its 22nd year since establishment.

When people think of the dentist, many say this:
A dentist is “a place you go when your teeth hurt.”
That is true. Teeth tend to send clear signals when something is wrong. If you feel a throbbing pain while chewing or a sharp sting when drinking cold water, you immediately think, “Oh, something’s going on.”
By contrast, gums are a little different. Even if your gums swell or bleed, it is easy to brush it off as “Did I brush too hard?” And if your breath becomes worse, you may think, “Maybe I’m just not feeling well lately,” and let it pass as part of daily life.
The problem starts here. Gum disease is not a condition that is fine because it causes little pain; it is a condition that is easy to discover late because it causes little pain. So by the time you actually feel pain, the condition below the gums has often already progressed.
Today, at S Leader Dental Hospital, Konkuk Univ. Entrance Dental Clinic, we will explain why gum disease progresses quietly, which signals you should catch early, and how dentists decide whether scaling alone is enough or whether gum treatment is needed—organized so that after reading once, you can get a sense of which situation your own condition may be closer to.
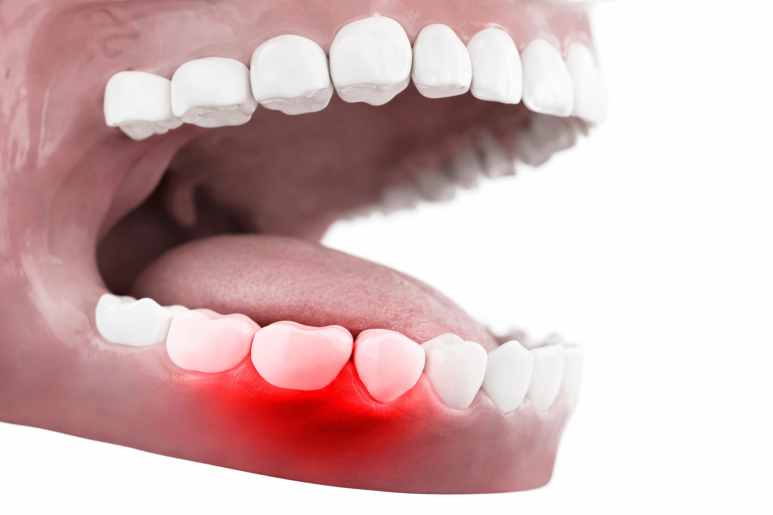
4 reasons gum disease progresses “quietly”
- In the early stage, it is often “surface inflammation,” so the pain is not severe
Gum disease does not start with the bone collapsing from the beginning; in most cases, it starts with inflammation on the surface of the gums. At this stage, there is often no pain, or at most, it may pass as “itchy / uncomfortable / slightly stinging.” More commonly, however, you may notice bleeding when brushing, slight swelling of the gums, or a dull feeling between the teeth.
- The body adapts to discomfort, and people mistake “familiarity” for normal
If the gums bleed a little, anyone will pay attention at first. But if it repeats for weeks or months, people strangely adapt and start thinking, “Is this just how it is?” Bad breath is similar. You get used to it yourself and stop noticing it, and if people around you say nothing, you may not think it is a serious issue.
That is why gum disease is even quieter. It is not because the gums are quiet; it is because we tend to feel and accept the signals as small.
- Unlike teeth, “nerve-like warning” does not always come quickly
When cavities get close to the nerve, pain rises sharply. That makes them easier to recognize. But gum problems send signals in the form of bleeding, swelling, odor, bad-smelling floss, or food getting stuck between teeth rather than nerve pain, so they are easily classified as “bearable discomfort” and delayed. The longer that delay continues, the more likely the environment below the gums is to change.
- By the time it starts to hurt, it may already be deep
When gum disease progresses and begins affecting the jawbone around the gums, the pattern can change. You may also feel a dull ache when chewing, a sense that the tooth feels elevated, looseness, or increased sensitivity as the gums recede. So the important point is this.

A quick look at gum disease stages: gingivitis → periodontitis
It is much easier to understand gum disease if you think of it in two major stages.
If you know these two stages, you can roughly estimate “which side am I closer to?” and “is there a chance it can end with scaling?”
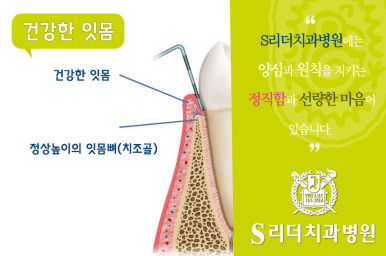
- Gingivitis (inflammation limited to the gums)
This is the stage where the gums swell and bleed. In many cases, this stage does not significantly affect the bone, so the response to care and treatment can be relatively good. In other words, this is the time when “early detection” is most valuable. Gingivitis literally means a problem on the “surface of the gums,” so there are quite a few cases that stabilize with scaling and lifestyle corrections.
- Periodontitis (affecting even the jawbone around the gums)
This is the stage where inflammation has become deeper and begun affecting the area around the jawbone. At this stage, it is often difficult to solve the problem by simply brushing more diligently, and treatment to remove tartar (subgingival calculus) that has accumulated below the gums may be necessary. Many people feel that periodontitis “appeared suddenly,” but in reality, it often develops as gingivitis quietly builds up and crosses over. That is especially true because early pain is minimal.
10 early warning signs of gum disease (if 2–3 apply, check it out)
It is easy to be late if you judge gum disease only by “does it hurt or not.” Instead, check the signals below. If 2–3 or more apply, and especially if they repeat, it is safer to get a checkup.
-
Your gums bleed when you brush
-
Your gums bleed when you floss, or your floss smells bad
-
Your gums often swell or feel itchy
-
Bad breath concerns you more than before
-
Your mouth feels especially sticky and unpleasant in the morning
-
Food starts getting stuck between your teeth more often
-
Your gums feel like they have receded, making your teeth look longer
-
Sensitivity has increased compared to before
-
A certain area feels dull and uncomfortable when chewing
-
A specific gum area swells especially often (a repeated area)
✅ Blood + odor + swelling
If this combination repeats, it is hard to see it as just a temporary condition. Gums often speak this way first instead of through pain.

3 simple checks you can try at home (self-check)
We get asked this a lot: “What should I look at before going to the hospital?” A self-check cannot confirm a diagnosis, but it can help you determine whether the signals you have been ignoring are repeating or not.
- Floss test: “blood” and “odor” are signals from the gums
If your gums bleed often when flossing, or if the floss smells strong, there may be inflammation between the teeth or tartar/plaque that has built up for a long time. Many people brush diligently but still have ongoing gum discomfort, and that is often because the reason is hidden here. The spaces between teeth cannot be fully cleaned by brushing alone.
- Compare photos of the gum line (every 2–4 weeks): “recession” is not something you feel in a day.
If you look in the mirror every day, changes are hard to notice. Photos are different. If you take pictures from the same angle every 2–4 weeks, you may see, “Oh? The line here looks different.” However, photos are affected by lighting and angle, so this is only for reference. Still, it can help visually confirm a feeling that “something seems to keep changing.”
- Record bleeding/swelling: the important thing is repetition, not a single event.
Gums can react differently depending on the day’s condition. So what matters is not “it bled once,” but the pattern repeated over several days to weeks. Keeping a record makes it clearer that “I was just letting this go.”
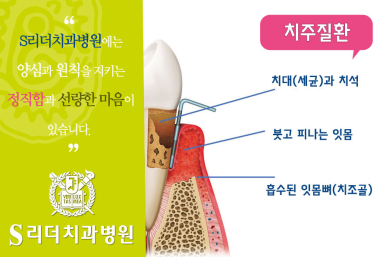
What do dentists check? (examination flow)
When gum disease is suspected, dentists do not simply end with saying, “Your gums look bad.” The important thing is to accurately confirm the current stage, meaning the current location of the condition.
- Check bleeding, swelling, and tartar location: organize the visible signs first
First, the dentist checks where bleeding is happening, whether there is swelling, and where tartar is most concentrated. In particular, tartar below the gums is hard for patients to see themselves. That is also why many people feel that their mouth looks clean on the surface, yet their gums keep feeling uncomfortable.
- Gum pocket depth test: the 기준 for deciding whether scaling alone may be enough
There is normally a very shallow gap between the gums and the teeth. But if inflammation becomes deeper, that gap can become like a “pocket,” which is called a pocket. As the pocket deepens, the environment below the gums becomes more favorable for bacteria, and tartar can settle and accumulate there more easily. That is why the pocket test helps determine whether simple scaling is likely enough or whether treatment below the gums is needed.
- X-rays if necessary: bone condition cannot be judged by appearance alone
The visible appearance of the gums and the condition of the bone do not always match. Sometimes there are bone changes even when the gums are not significantly swollen, and other times the gums are red and swollen on the surface but the bone changes are not severe. So if needed, X-rays are used to check the condition of the jawbone around the gums. In the end, the treatment plan is determined by checking both what can be seen and what cannot be seen.

How is treatment carried out? (step-by-step flow)
Gum disease treatment is often carried out not as “one treatment and done,” but by organizing the condition step by step and re-evaluating it according to the situation.
Step 1: Scaling / controlling inflammation
This is the basic step of removing tartar and reducing inflammation. Many people think, “If I just get scaling, that’s the end,” but this step is literally the “basic cleanup.” In many cases, people improve at this stage, but if bleeding or swelling keeps recurring even after this step, the next stage may be necessary.
Step 2: Removing tartar below the gums (if needed)
If tartar has gone deep below the gums, treatment may be needed to clean below the gums as well. Depending on the condition, this process may be carried out by dividing the treatment by area rather than doing everything at once. People often ask, “Why do I need to come multiple times?”—the reason is that the area below the gums is sensitive, and forcing everything in one session can increase discomfort, so a stepwise approach is sometimes used.
Step 3: Re-evaluation (checking whether there has been improvement)
After treatment, the gums are checked to see how stable they have become. At this stage, the decision is made about whether to continue treatment or move on to maintenance care. This re-evaluation is important because, in gum treatment, how the gums respond to healing is more important than the fact that treatment was done once.
Step 4: Maintenance care
Gum disease is less like something that is completely finished after one treatment and more like a condition that stays stable when a proper management routine is established. Regular checkups, scaling intervals, and interdental care routines are key. In the end, gums respond much better to “a little bit consistently” than to “one big treatment once.”
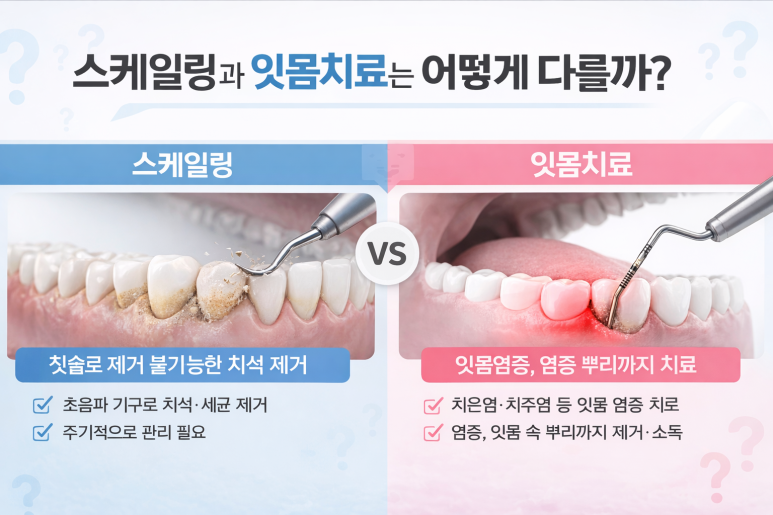
How are scaling and gum treatment different?
“I got scaling, so why am I still bleeding?”
“What is the difference between scaling and gum treatment?”
These are very common questions. Simply put:
Scaling: basic treatment that mainly cleans the tooth surface and the gum line
Gum treatment (periodontal treatment): needed when tartar/inflammation below the gums must be managed more deeply
So if bleeding and swelling continue even after scaling, rather than blaming yourself for “not brushing well enough,” it may be more accurate to check the condition below the gums once. It may not be a matter of effort, but rather a condition where the area that needs care has changed.
In the end, gum disease is often less a condition that suddenly becomes a big problem and more a condition that quietly accumulates and increases daily discomfort. That is why catching it while it is quiet is the most efficient approach.

Prevention: 6 habits that keep gum disease from progressing “quietly”
The most important thing for protecting your gums is not an expensive toothpaste or a costly, special product.
In the end, what matters is a lifestyle habit you can keep consistently.
So today, let’s focus only on routines that are practical and realistic without feeling burdensome.
- Floss or use interdental brushes once a day
Doing it once at night is more important than doing it perfectly every time. The starting point of gum disease is often the spaces between the teeth.
- Brush the gum line gently
Brushing too hard can irritate the gums. The key is gentle, thorough, and accurate. In particular, it is important to lightly brush along the gum line.
- Manage dry mouth and smoking
When the mouth is dry, bacteria can multiply more easily, and smoking can affect gum recovery. Even small adjustments to these habits can make a difference in gum condition.
- Set regular scaling/checkup intervals
For people who form tartar easily, shorter intervals can be helpful. In many cases, regular management is more comfortable than getting a large amount of treatment all at once.
- Check habits of grinding or clenching
Clenching your teeth tightly can place stress on the gums and teeth. In particular, for people under a lot of stress, consciously relaxing the jaw can help.
- Do not ignore the “blood/odor” signals
Gums often speak through blood and odor instead of pain. Not ignoring those signals is ultimately the biggest prevention.

The signals your gums send,
this is how S Leader Dental Hospital,
Konkuk Univ. Entrance Dental Clinic,
checks them.
The reason gum disease progresses quietly is not because the gums are fine, but because we tend to use pain as the only 기준, while gums often speak first through signals such as bleeding, swelling, and odor. So for gum disease, the most important thing is not “it’s okay because it doesn’t hurt,” but rather reading the signals and managing them before the pain starts.
If some of today’s checklist items keep repeating, simply checking your condition once before it develops into a major treatment can already make a difference.
At S Leader Dental Hospital, Konkuk Univ. Entrance Dental Clinic, when patients visit because their gums bleed or because bad breath is concerning, we do not simply recommend scaling alone. Instead, we check gum bleeding, tartar location, and the condition below the gums together so that we can realistically guide them toward the care and treatment needed at the current stage. Gum disease progresses quietly, but if caught early, it can become much more manageable. Rather than putting up with discomfort for too long, we recommend checking your gum condition accurately through an examination.





Konkuk Univ. Entrance Dental Clinic :: S Leader Dental Hospital















