When going about everyday life as usual,
hardly anyone seriously thinks about how much
hair they are losing or bothers to count it.
Human hair generally sheds about 50 to 100
strands a day through natural activities and
habits. However, if the amount exceeds this
and hair is falling out excessively, or if the
hair itself has become weaker and thinner
than before, it may be possible to suspect
a typical condition has developed.
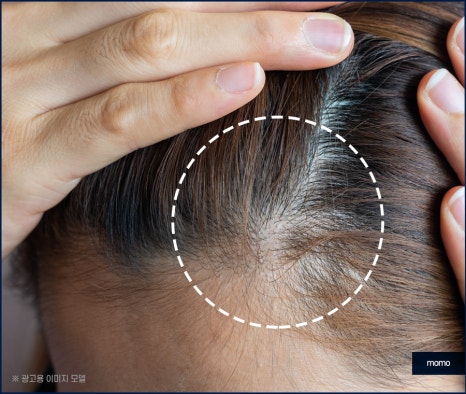
There are many reasons why these symptoms
appear. Representative causes include genetic
factors that can be passed on to you if a
family member or relative has a condition
that causes hair loss, an overly dry air
environment that leads to excessive scaling
on the scalp, or increased sebum secretion
due to low humidity. In addition, hormonal
changes, large and small amounts of stress
from various environments such as school and
work, and the negative effects of an irregular
lifestyle and Westernized eating habits that
are often overlooked because of a busy daily
routine can worsen the condition of the scalp
and hair, and may cause a large amount of
hair to fall out.
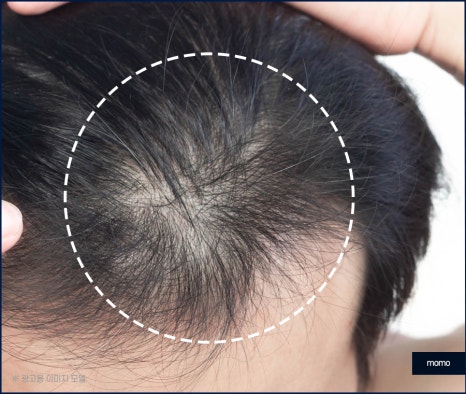
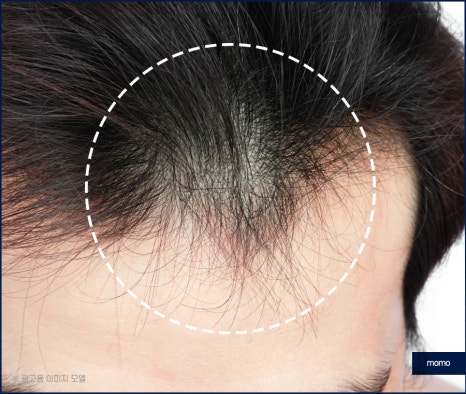
This condition can also appear in many
forms, such as male pattern and female pattern
hair loss. Today, we will take time to look
at frontal hair loss among them. First, there
is a way to self-check for a hair-loss
condition, so I would like to share that
first. Using your thumb and index finger,
gently pull the hair on the front, back, and
sides of your head. If three or more hairs
come out, it can be judged that the symptoms
are likely already progressing. Also, if the
amount of hair falling out on your pillow or
around you after sleeping, or when brushing
and shampooing, has noticeably increased
compared with before, or if your scalp
frequently itches and dandruff has increased,
or if you often undergo hair procedures such
as perms and dyeing, you should be even more
careful not to overlook this condition.
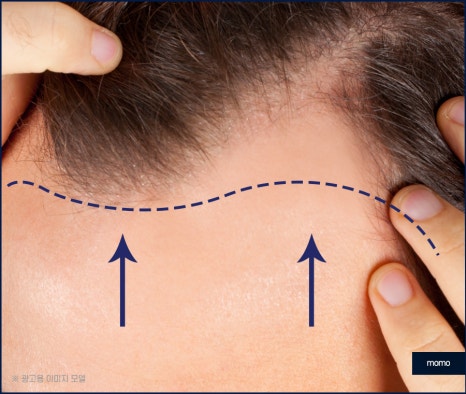
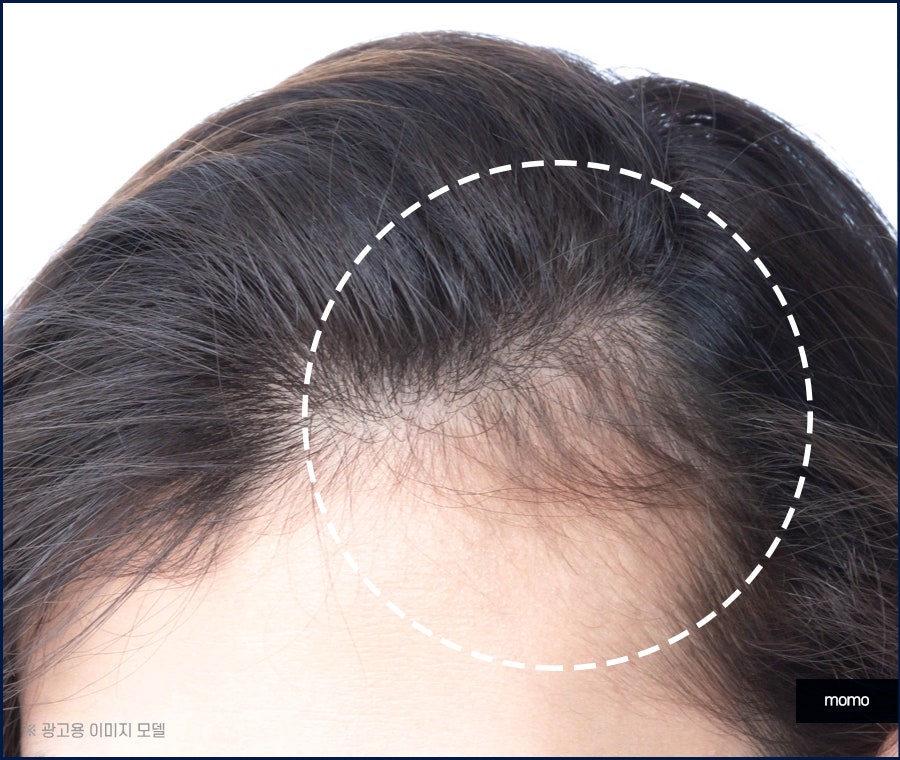
So, what does frontal hair loss mean?
It refers to a condition in which the hairline
in the forehead area and the sides gradually
recedes backward, forming a scar-like lesion
in a band shape. This is called frontal hair
loss. It is known to occur mainly in post-
menopausal women between about 55 and 70 years
old.
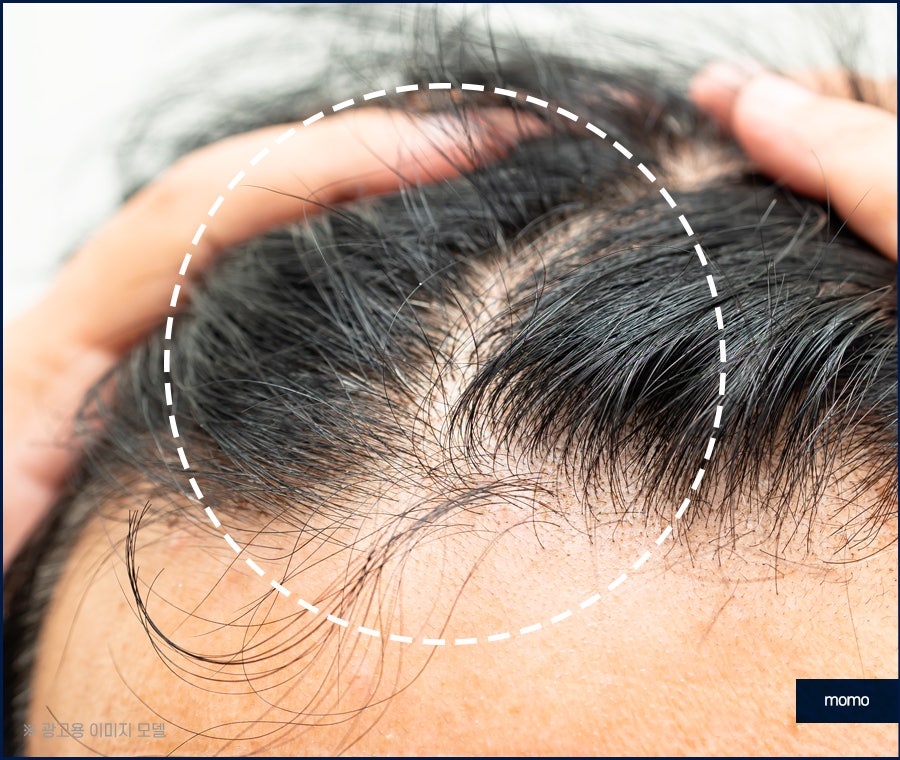
In the area where symptoms begin to appear,
typical signs of cicatricial alopecia, in
which the follicles close, are visible. In
addition, hyperkeratinization and redness
appear around the follicles, indicating that
frontal hair loss is currently active and
progressing. This type of hairline recession
occurs slowly and gradually, and if it is not
actively addressed early, it is known to
recede by an average of about 1.05 cm each
year.
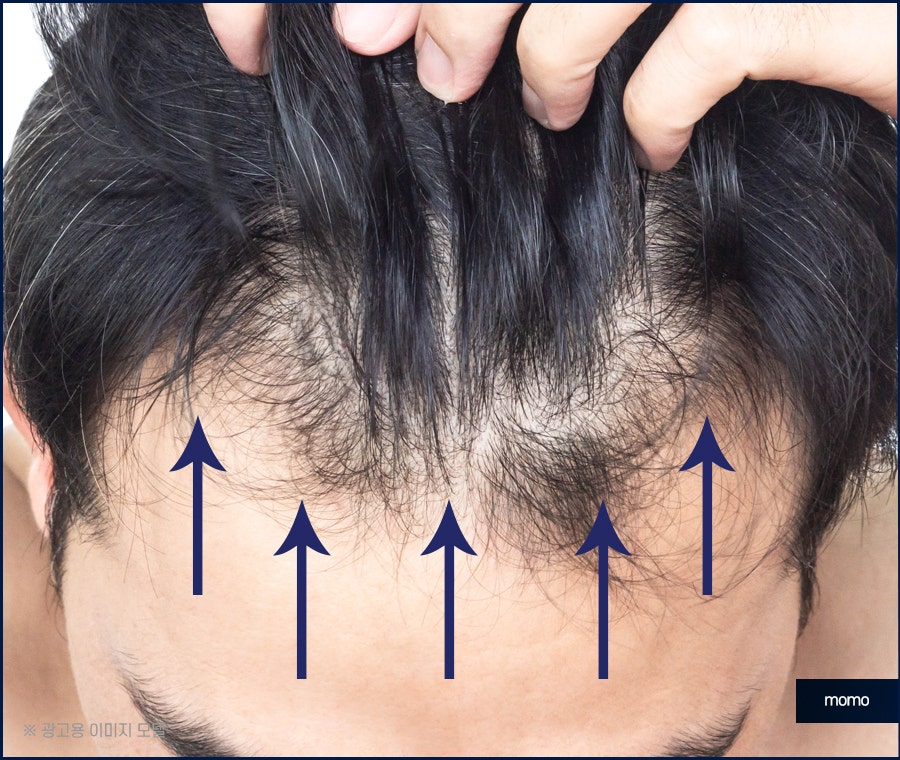
Another way to diagnose this condition based
on clinical features is the previously
mentioned recession and unclear shape of the
hairline, along with a paler skin tone than
normal skin, loss of eyebrows and fine hair,
or veins in the affected area that are visible
enough to stand out. If only one or a few
hairs remain on the existing border line, or
if papules appear and small black or brown
spots are visible on the face, it would be
wise to recognize that the condition has
occurred.
There are several hypotheses about the causes
of frontal hair loss, although they are not
completely certain. Among them, one of the
main factors said to be more commonly found
than in cases without it is a family history
carrying the influence of a specific gene.
Also, since it tends to occur more often in
women after menopause, estrogen is especially
related to the hair cycle, promoting the
transition to the catagen and telogen phases.
It is said that a deficiency in this hormone,
or pregnancy, childbirth, breastfeeding, and
hormone therapy, may increase the risk of the
condition.

In addition, considering that such cases have
recently occurred worldwide, environmental
factors should by no means be overlooked.
These include excessive dieting, sunscreen,
dyes, shampoo, and smoking. In particular,
with sunscreen, if it accidentally enters the
hair follicle, it can disrupt the immune
response and trigger autoimmunity, so caution
is needed. If frontal hair loss appears to me,
it can only become a source of deep concern
and worry.
If you notice signs such as hair losing its
strength, becoming thinner, or falling out,
rather than making crude attempts with various
unverified methods, it is most important to
visit a relevant clinic, carefully consult
about your current symptoms, condition, and
type, and proceed with appropriate testing.
Also, the measures for addressing frontal hair
loss can include efforts to improve it with
steroid-related solutions or methods such as
5-alpha reductase inhibitors if the symptoms
are relatively early. After these symptoms
stabilize, a direction toward hair transplant
can also be pursued to expect a natural and
full hairstyle.

However, because the long-term graft survival
rate that can be maintained may also decline
when the condition is recurring or still
progressing, it would be advisable to pursue
such solutions after confirming that the
symptoms have clearly stopped.