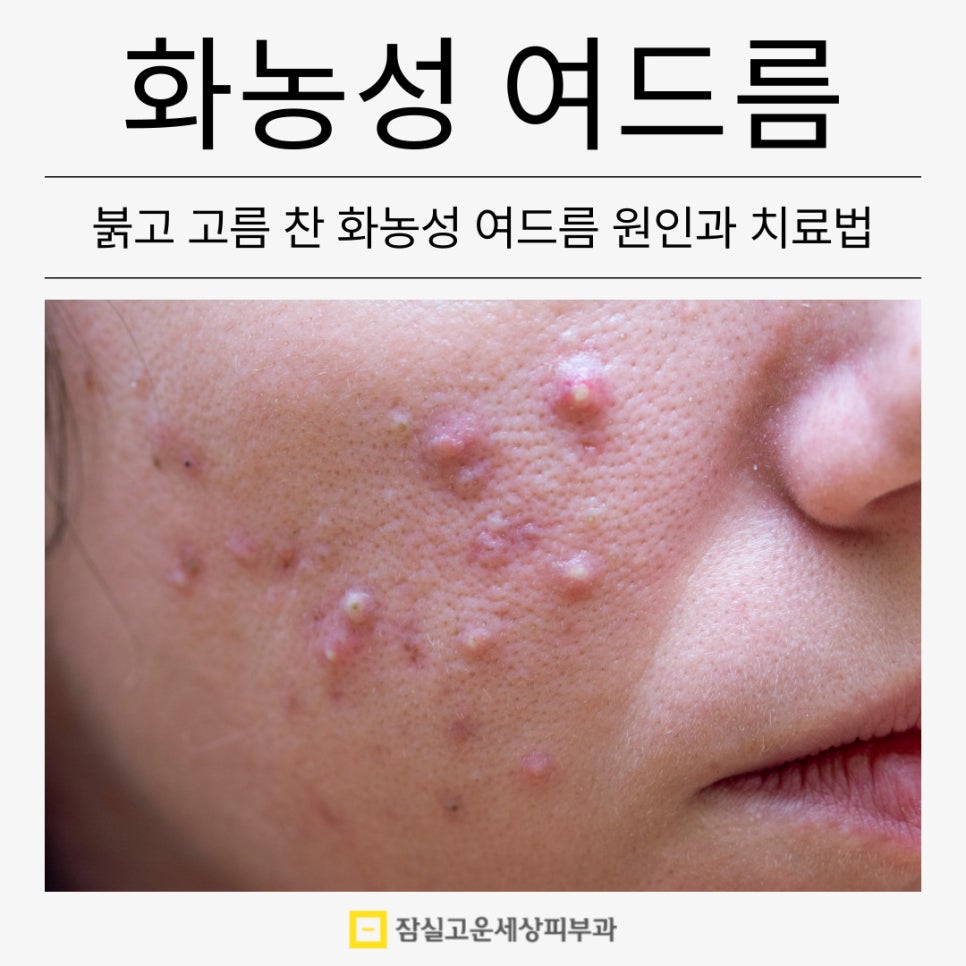
Red, pus-filled pustular acne
From the causes to treatment!
Hello, this is Jamsil Gounsesang Dermatology.
A hard lump suddenly appears on the skin. After a few days,
pus builds up inside, and it becomes red and swollen, causing
pain and discomfort so severe that even touching it with your
hand is difficult.
You may let it pass, thinking one or two times is fine, but when
it keeps recurring, it appears again in the same area, and even
after it calms down, pigment may remain or the skin may sink
in, leading to scars. In many of these cases, it is “pustular acne.”
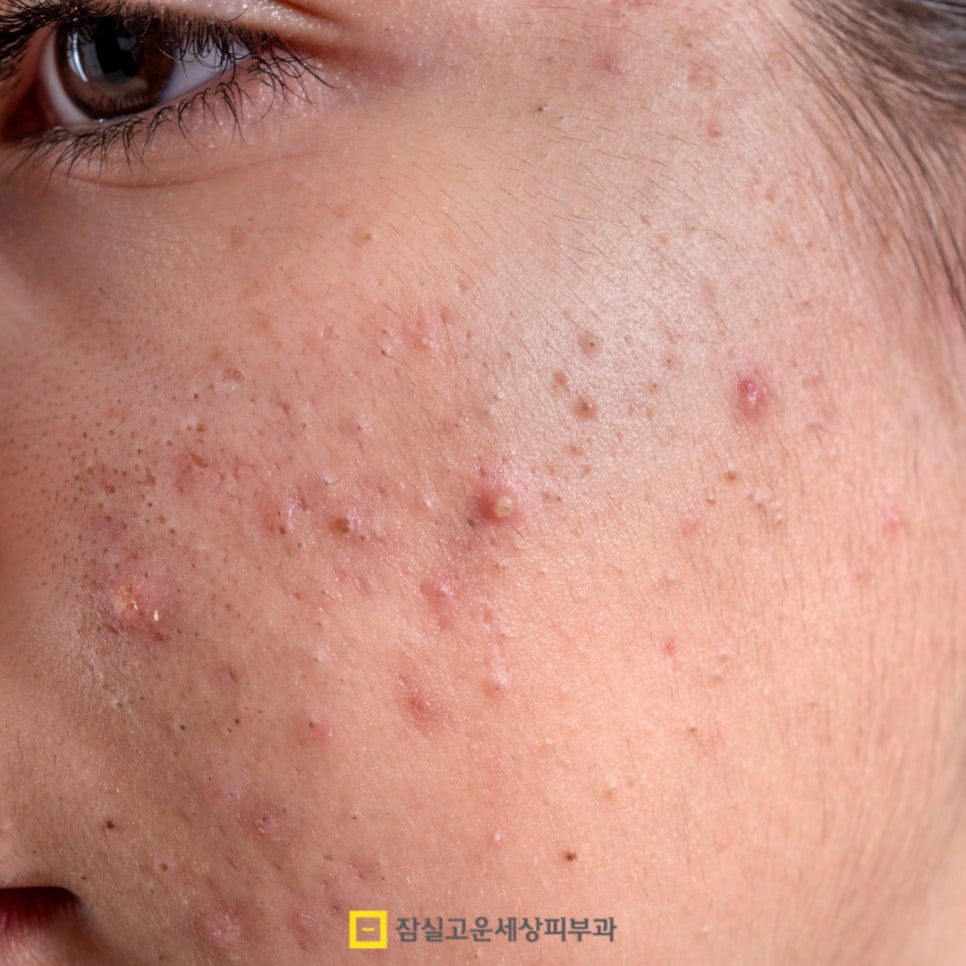
Pustular acne is not simply severe acne; it is a state in which
a strong inflammatory response and infection have already
occurred within the skin. Because the follicle and dermal tissue
are being damaged in a deeper area than the pus visible on the
surface, it cannot be resolved with topical treatments alone, and
if left untreated, it can lead to scarring, recurrence, and
post-inflammatory hyperpigmentation.
That is why it is most important to accurately diagnose pustular
acne early and receive appropriate treatment.
- Why does it occur?
- Main causes of pustular acne
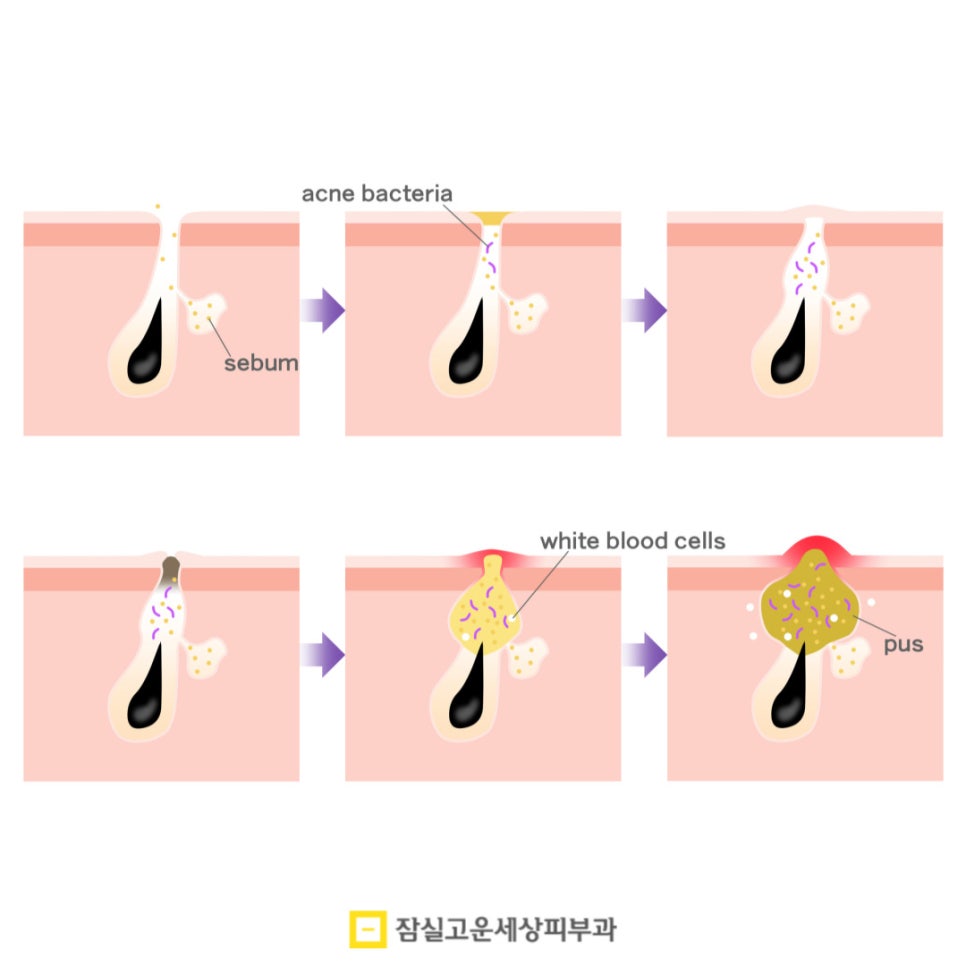
Pustular acne occurs when four conditions act at the same time:
excessive sebaceous gland activity, clogged pores, bacterial
infection, and an inflammatory response. First, as the sebaceous
glands become highly active and sebum is excessively secreted
onto the skin surface, this sebum mixes with dead skin cells
inside the pores and blocks the pathway for sebum drainage,
forming the “comedone,” the starting point of acne. Then the
acne bacteria inside the pore multiply by feeding on the sebum,
and as the immune response tries to eliminate them, inflammation
occurs. At this point, the tissue around the pore is damaged, and
white blood cells gather at the inflamed area, creating pus.
That is pustular acne.

This process is not limited to a skin problem alone, but is also
strongly influenced by hormonal changes and lifestyle habits.
In particular, during the late teens to early twenties, sebum
production increases sharply due to an increase in male hormones
(androgens). In women, symptoms may worsen around the menstrual
cycle or in connection with conditions such as polycystic ovary
syndrome.
If irregular sleep, a high-fat and high-sugar diet, smoking,
stress, and skin irritation (such as excessive cleansing or
cosmetic ingredients) are added on top of that, pustular acne can
fall into a vicious cycle of recurring outbreaks.
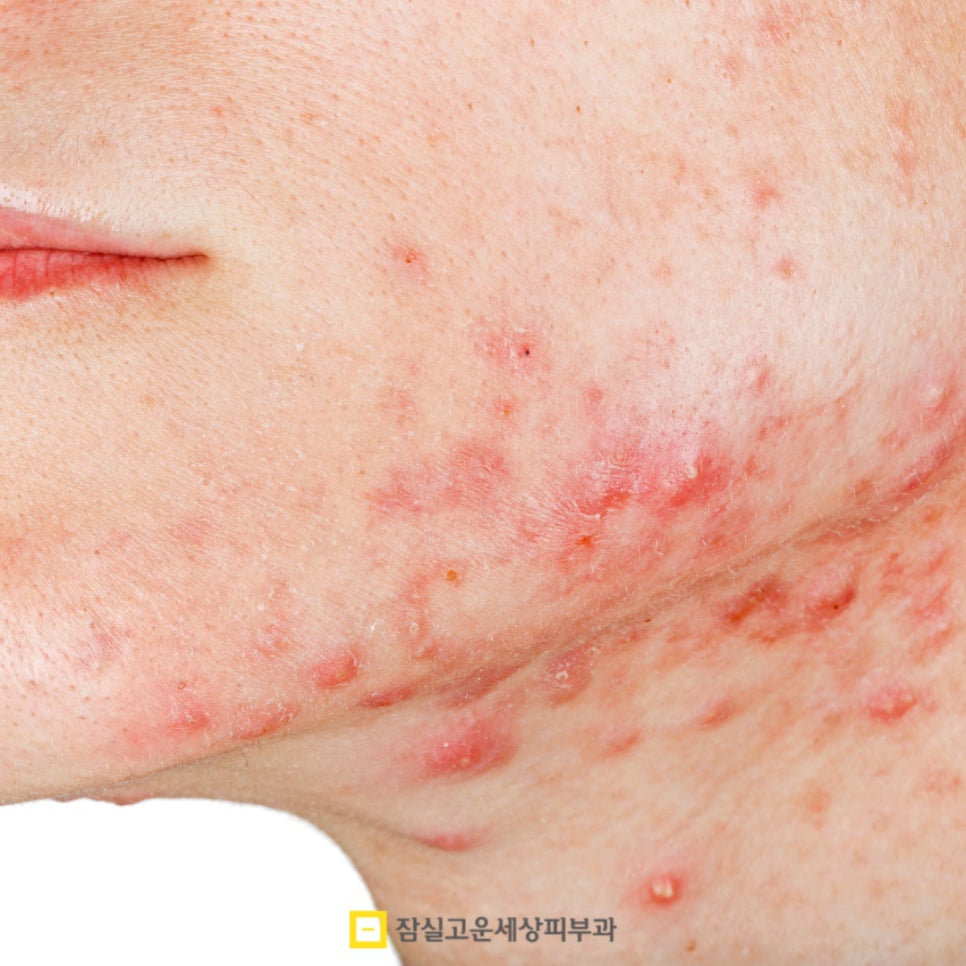
- How does it appear?
- Characteristic symptoms of pustular acne
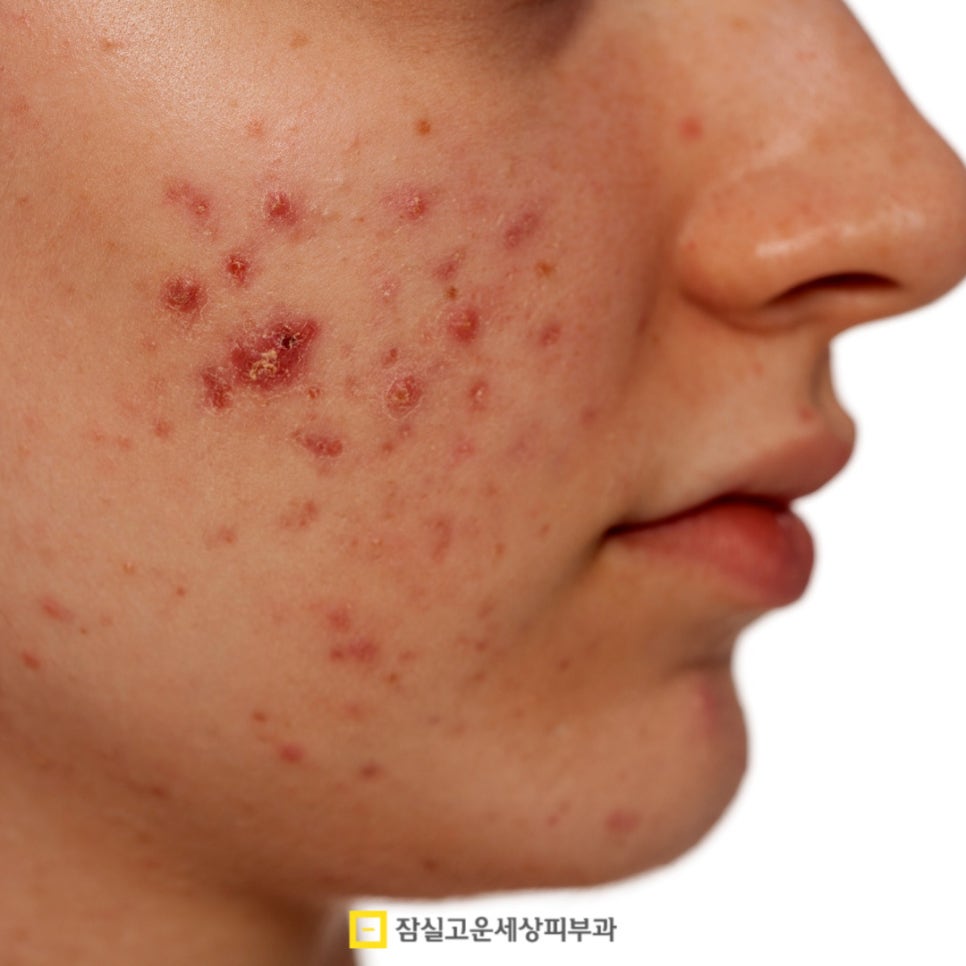
Pustular acne appears superficially as a red, raised inflammatory
nodule. In the beginning, it starts as a small, painful lump deep
in the skin, but it gradually grows larger and fills with pus,
with a white or yellow center beginning to protrude.
When touched from the outside, it feels warm, there is deep pain
when pressed, and the skin may become firmly swollen.
In particular, pustular acne often develops in areas with active
sebum secretion such as the chin, cheekbones, temples, and
around the neck, and it is sometimes distributed symmetrically.
Multiple lesions may appear at once, or it may recur in the same
spot after it has subsided. The important thing is that at this
stage, the skin tissue has already been partially destroyed, and
because the inflammation has invaded the dermis, irritation can
lead not only to hyperpigmentation but also to depressed scars.
How is it treated?
- Step-by-step treatment for pustular acne
The treatment approach for pustular acne differs depending on
whether it is mild, moderate, or severe.
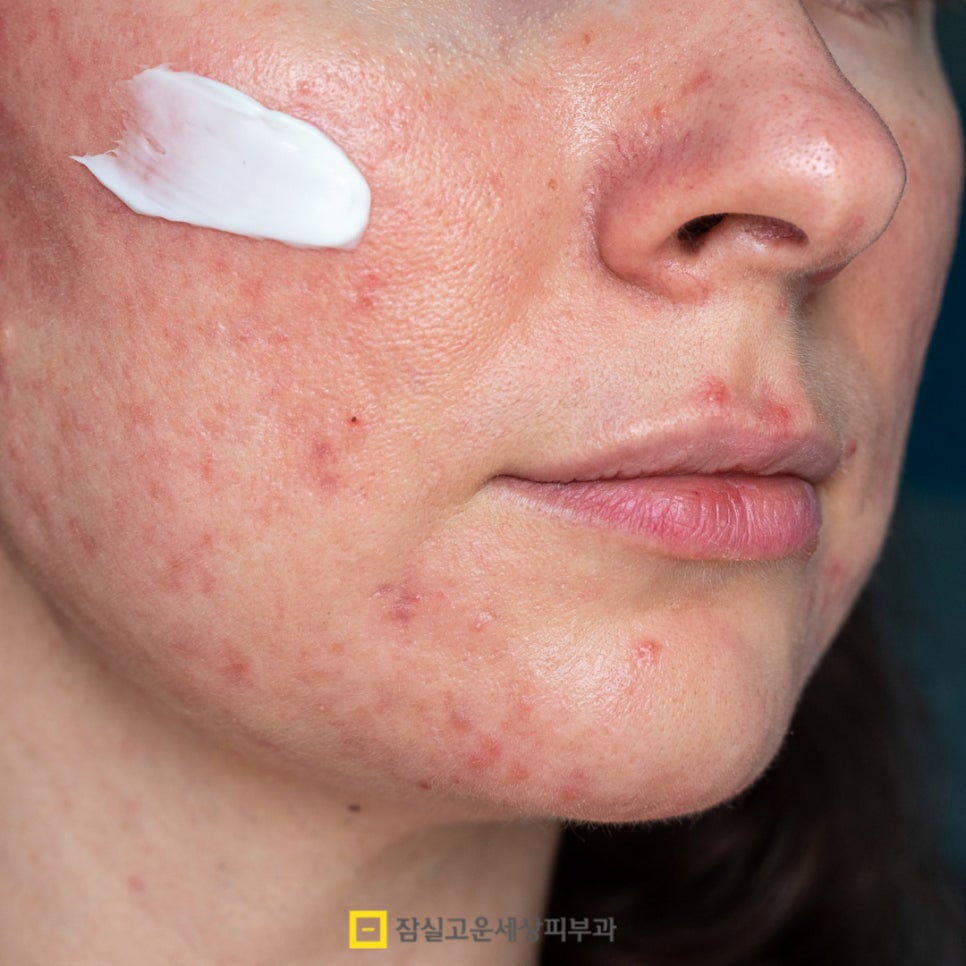
In mild cases, topical anti-inflammatory agents are used first,
and external treatments that suppress the growth of acne bacteria
and calm inflammation inside the pores are the basis of care.
These may include antibiotic ingredients, retinoids, and benzoyl
peroxide, and using a cleanser or improving lifestyle habits in
parallel can also help with prevention.
For moderate to severe pustular acne, simple topical medication
has limited effectiveness, so hospital treatment is necessary.
At this stage, an incision and drainage procedure to release the
pus is performed first, and afterward, an antibiotic ointment is
applied to the infected area. If inflammation is severe, a very
small amount of steroid is injected into the inflammatory lesion
through an intralesional injection. This injection is effective in
quickly calming inflammation and reducing the risk of scarring.
If pustular acne recurs chronically or the affected area is wide,
oral medication that systemically suppresses sebum production may
be considered. This method directly controls the sebaceous glands
to suppress acne formation itself, and is especially used when
pustular acne has recurred continuously for more than 6 months or
has not responded to previous treatment. However, because of liver
function concerns and, in women, issues related to contraception,
expert diagnosis and regular consultation are absolutely necessary.
In addition, depending on the case, acne treatment peels, radio
frequency, laser, and other energy-based devices may be used in
combination to regulate sebaceous gland activity or reduce
post-inflammatory hyperpigmentation.
However, all treatments should be customized by comprehensively
considering the skin condition, depth of inflammation, and history
of recurrence. Above all, early intervention before the
inflammation progresses is the key to avoiding scars.
Pustular acne cannot be resolved simply by removing the visible
pus.
Because the inflammation has spread into the dermis, the skin
structure itself is damaged, and as a result, marks and scars are
easily left behind. In particular, if you squeeze acne with your
hands or try to treat it yourself, the inflammation can spread to
surrounding areas, and recovery will inevitably be slower.
The key to treatment is quick intervention and step-by-step
response. From the moment inflammation begins, the reaction inside
the skin must be accurately assessed, and when necessary, the
spread of inflammation should be blocked through procedures such
as drainage, antibiotics, and injection treatment.
For recurring pustular acne, lifestyle management should be
combined with sebum-control treatment, and if pigmentation or
scars remain afterward, treatment should continue with a focus on
regeneration.
Acne is common, but pustular acne is different. Do not dismiss it
as a simple skin problem. To reduce invisible damage and recover
without regret, the moment inflammation appears on the skin is the
most important time. What you do now will determine the skin you
have in the future.
Directions to Jamsil Gounsesang Dermatology
Jamsil Gounsesang Dermatology Treatment Guide
Jamsil Gounsesang Dermatology Homepage
This article is provided by Jamsil Gounsesang Dermatology for the purpose of providing medical information in accordance with Article 56, Paragraph 1 of the Medical Service Act. As all procedures/surgeries carry the risk of side effects such as bleeding, infection, and nerve damage, please proceed carefully after充分 consultation with medical staff.








