Atopic Dermatitis
Complete Guide!
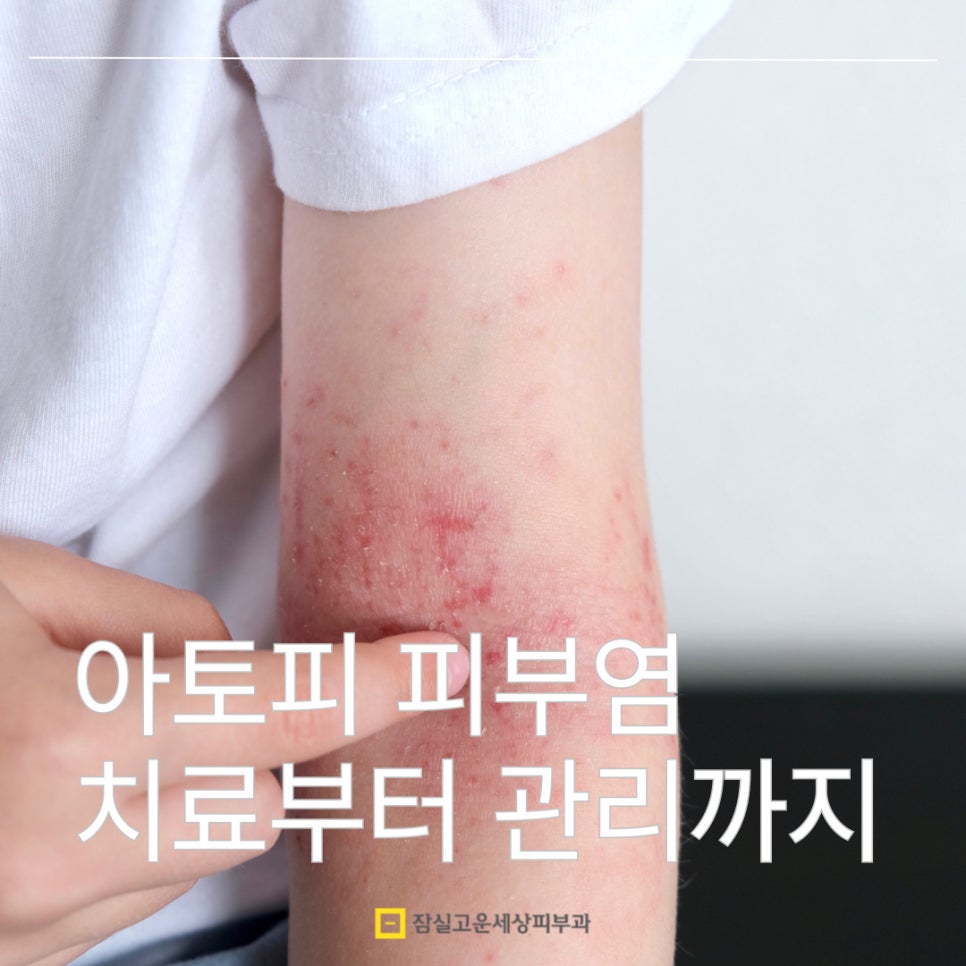
Hello! This is Jamsil Gounsesang Dermatology:-)
You've probably heard many people around you say things like, "It’s been like this since I was little," "They say it’s genetic, so there’s nothing I can do," and "It doesn’t get better even if I watch what I eat."
Atopic dermatitis is not simply a matter of itching on the skin. When you look at children who scratch all night and lose sleep, adults who cannot concentrate at work, and in severe cases people who avoid going out in front of others and end up experiencing depression and social isolation, you can see how much this condition lowers quality of life.
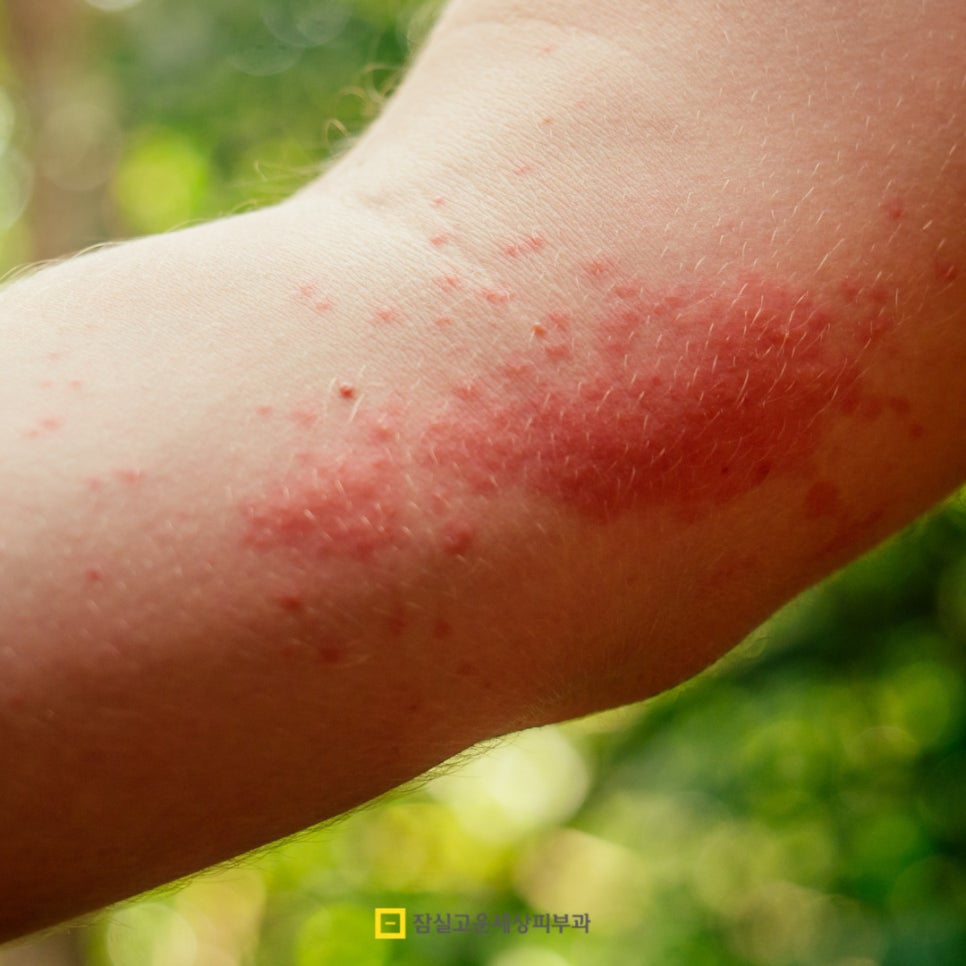
However, atopic dermatitis is not a disease that can be dismissed as merely an "inborn constitution." If you understand the cause accurately, treat it systematically, and manage it in daily life, it is a condition that can be made much less painful.
Today, we will take a closer look at the causes and treatment of atopic dermatitis, as well as management methods that can be practiced in everyday life.
- The
Fundamental Causes and Mechanism of Atopic Dermatitis
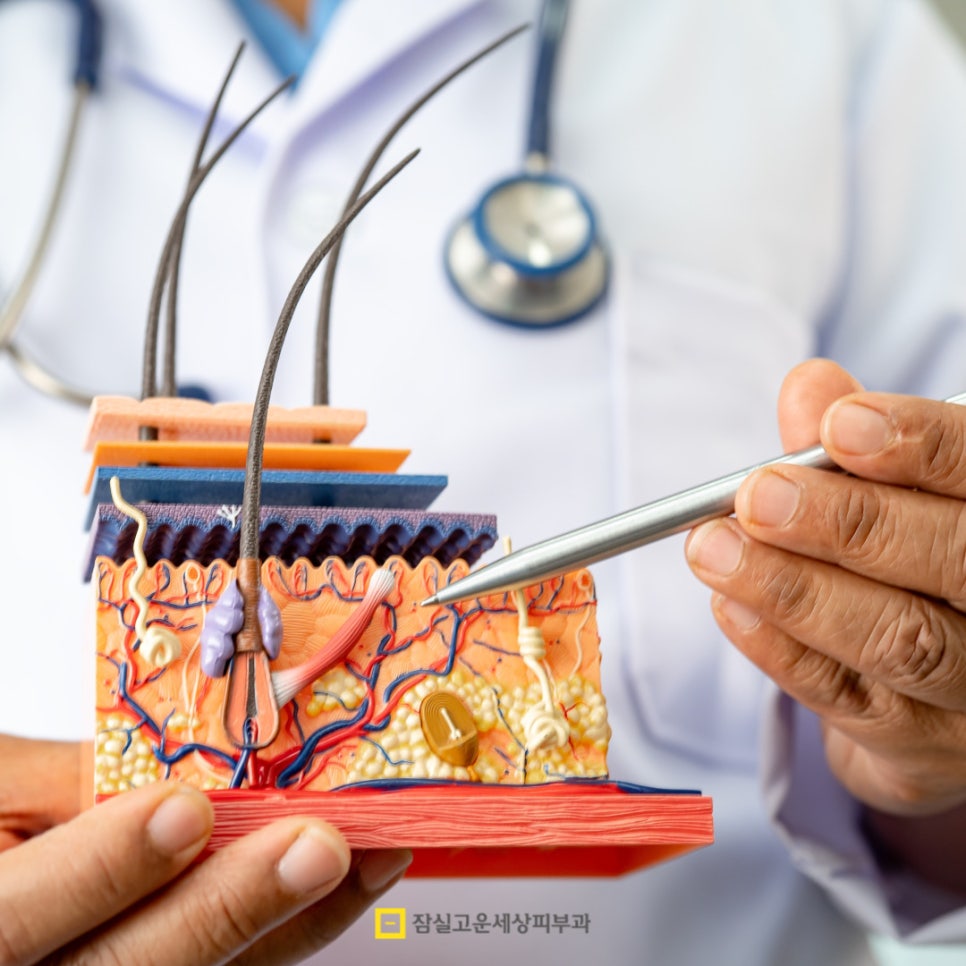
The most fundamental cause of atopic dermatitis is an abnormality in skin barrier function.
Normal skin has keratinocytes tightly connected like stacked bricks, with lipid components such as ceramides filling the spaces between them to protect the body from external irritation. But in the skin of atopic dermatitis patients, this barrier is weakened, so moisture escapes easily and, on the other hand, external allergens or irritants can penetrate more easily.

When various substances such as dust mites, animal dander, pollen, detergents, sweat, and fragrance penetrate through this weakened skin barrier, the body's immune system recognizes them as external invaders and triggers an excessive response. This is the key mechanism that causes the inflammation and itching of atopic dermatitis. It is similar to how wind and dust keep entering a house whose door does not close properly, making the house messy.

In particular, many atopic dermatitis patients have insufficient production of a protein called filaggrin in the skin.
This protein plays an important role in skin moisture retention and barrier formation. When filaggrin is lacking, the skin becomes dry and more sensitive to external stimuli, which creates a vicious cycle that further worsens atopic dermatitis symptoms.
- The Interaction of Genetic and Environmental Factors
Genetic factors also play an important role in the development of atopic dermatitis. If there is a history of allergic diseases such as atopic dermatitis, allergic rhinitis, or asthma in the family, there is a high possibility of having a genetic predisposition known as the so-called "atopic march." If one parent has atopic dermatitis, the likelihood of it occurring in a child is about 30-40%, and if both parents have atopic dermatitis, it rises to about 60-70%.
However, having a genetic predisposition does not necessarily mean atopic dermatitis will occur. According to recent studies, environmental factors interact with genetic predisposition to determine the onset of atopic dermatitis. Fine dust, air pollution, sudden temperature changes, excessive stress, and a Westernized diet are major environmental factors that can trigger or worsen atopic dermatitis.

In particular, the modern-day "hygiene hypothesis" is also drawing attention. It is the theory that children who grow up in overly clean environments may actually be more vulnerable to allergic diseases. The idea is that appropriate exposure to bacteria during childhood helps the immune system develop in a balanced way.
But this does not mean hygiene can be neglected; a balanced approach is needed.
- Systematic Treatment Methods and Step-by-Step Approach
The most important principles in treating atopic dermatitis are "restoring the damaged skin barrier" and "safely controlling the inflammatory response." Treatment should be approached step by step depending on the severity of symptoms and the patient's condition.
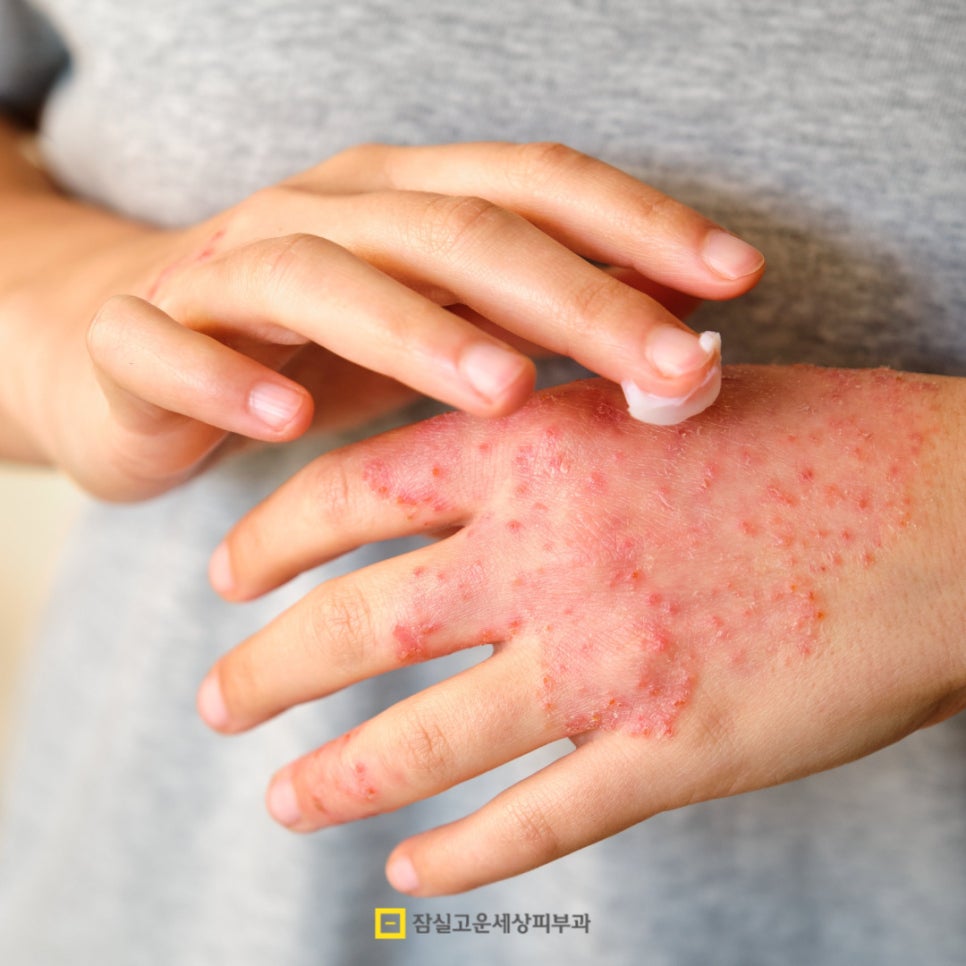
Stage 1 treatment is centered on topical steroid ointments. Many people have vague fears about steroid ointments, but if used with the proper strength and in the correct way, they are very safe and effective. Mild-strength steroids are used on sensitive areas such as the face and neck, while relatively stronger steroids are used on thicker areas of the trunk or limbs. The important thing is to gradually reduce the frequency of use as the inflammation subsides.
Topical calcineurin inhibitors such as tacrolimus (Protopic) or pimecrolimus (Elidel) are excellent alternatives to steroids. They are especially useful on areas where steroid side effects are a concern, such as the face, neck, armpits, and groin, or when long-term maintenance treatment is needed. There may be a slight stinging or burning sensation at first, but for most people this disappears after a few days of use.
Stage 2 treatment can include phototherapy. Ultraviolet B (UVB) phototherapy is effective in regulating the immune system and reducing inflammation. If treatment is received 2-3 times a week, for a total of about 20-30 sessions, significant improvement can be expected. However, the downside is that the treatment period is long and requires frequent hospital visits.
Stage 3 treatment involves the use of systemic immunosuppressants or biologics. Systemic immunosuppressants such as cyclosporine, methotrexate, and azathioprine are effective for patients with severe atopic dermatitis, but regular blood tests and monitoring for side effects are necessary. Recently, a biologic called Dupixent has been introduced, offering new hope to patients with severe atopic dermatitis who do not respond to existing treatments.
- Managing Atopic Dermatitis in Daily Life
4-1. Proper Moisturizing
Moisturizing is the foundation of atopic dermatitis treatment. Moisturizer should be applied 2-3 times a day, especially within 3 minutes after showering. Lotions have a light texture and are suitable for larger areas, creams provide excellent moisturizing power, and oils offer the strongest moisturizing effect. Choose products with minimal fragrance, preservatives, and alcohol, and products containing moisturizing ingredients such as ceramides, hyaluronic acid, and glycerin are good.

4-2. Improving the Living Environment
Dust mites are the most common allergen. Keep bedroom humidity below 50%, use dust mite-proof covers on mattresses and pillows, and wash blankets and pillows in hot water at 60°C or higher at least once a week. It is better to use hard floors rather than carpets and blinds rather than thick curtains. Keep indoor temperature at 20-22°C and humidity at 40-60%, and replace air purifier filters regularly.
4-3. Proper Bathing Methods
When bathing, keep the water lukewarm (37-39°C) and make sure bath time does not exceed 10-15 minutes. Use mildly acidic products with a pH of 5.5 and avoid washcloths or rough sponges. After bathing, apply moisturizer generously within 3 minutes.
4-4. Clothing Selection and Laundry
Choose soft clothing made of 100% cotton and avoid wool or synthetic fibers. Be sure to wash new clothes once before wearing them, and choose loose-fitting clothes rather than tight ones to minimize friction on the skin. Use fragrance-free, fluorescent-free, low-irritation detergent, avoid fabric softener, and rinse thoroughly after washing so that no detergent residue remains.
4-5. Stress Management and Sleep
Stress increases cortisol secretion and worsens atopic dermatitis. Manage stress through regular exercise, meditation, yoga, and similar activities, but shower immediately after exercise to remove sweat. Lack of sleep weakens the immune system, so it is important to get enough sleep and maintain a comfortable bedroom environment.
4-6. Dietary Management
The relationship between atopic dermatitis and food varies from person to person. Eggs, milk, nuts, shellfish, and wheat flour are common allergenic foods, but indiscriminate dietary restrictions can lead to nutritional imbalance. Consult a specialist and confirm with allergy testing.
Fish rich in omega-3 fatty acids, vegetables and fruits with many antioxidants, and yogurt containing probiotics can help reduce inflammation.

Atopic dermatitis is a chronic condition in which genetic factors and environmental irritants act together.
However, it is necessary to move away from the idea that it is a burden you must carry for life and instead recognize it as a condition that can be sufficiently controlled through systematic management and treatment.
The most important thing is to combine appropriate medication treatment that restores the skin barrier and controls inflammation with moisturizing, environmental improvements, stress management, and proper lifestyle habits.
In particular, finding the "treatment and management method that suits you" and consistently practicing it is the most important thing.
Atopic dermatitis is not a condition that can be completely cured overnight, but through proper understanding and systematic management, it can be controlled to a level that does not interfere with daily life.
Above all, not giving up and establishing and following a long-term management plan with a specialist is the path to living healthily alongside atopic dermatitis. Do not become discouraged because of atopic dermatitis; we hope you can regain a healthy and happy daily life through active treatment and management.
Thank you!
[ Directions to Jamsil Gounsesang Dermatology ]
[ Jamsil Gounsesang Dermatology Clinic Information ]
[ Jamsil Gounsesang Dermatology Website ]
This article is provided by Jamsil Gounsesang Dermatology for the provision of medical information in accordance with Article 56, Paragraph 1 of the Medical Advertising Act. All procedures/surgeries carry the risk of side effects such as bleeding, infection, and nerve damage, so please proceed carefully after sufficient consultation with the medical staff.










