
When I first lost one molar, I never imagined the empty space would stay on my mind for so long. At first, I thought I could just chew on the other side, and I kept brushing off the discomfort as something minor, believing I would get used to it over time.
But after that molar was lost, my eating habits changed faster than I expected. Before long, I developed the habit of chewing on only one side without thinking, and there were many days when my jaw felt strangely fatigued. Even eating meals no longer felt like the carefree, thoughtless moment it used to be.
Still, I kept putting off treatment, thinking there was no way to get the missing tooth back anyway. But recently, when another molar also ended up needing extraction, the problem I had been avoiding all this time came rushing into reality at once, and I felt weighed down.
Having one molar missing and having several teeth missing were clearly different. There were more moments when I had to calculate which direction to chew, and I could no longer enjoy the foods I liked as freely as before. The emptiness in my mouth began to feel like more than a simple inconvenience, as if it were unsettling my whole daily life.
So I finally decided it was really time to stop delaying and began seriously looking into implants. I wanted to fill the missing space again and regain a daily life where I could chew properly, and even if it was late, I no longer wanted to leave my teeth unattended from this point on.
But during the consultation, I was told that it was not a situation where an implant could be done right away; a bone graft would be needed first. At that moment, I stopped again at the threshold of treatment because the process felt longer and heavier than I had expected.
Even the word implant already carried the tension of something like surgery, and hearing that I would also need a bone graft made my mind even more complicated.
In this way, many people come to learn about bone grafting only after looking into implants. Since an implant needs to be firmly anchored in the jawbone to last a long time, if a tooth has been missing for an extended period or if inflammation and periodontal disease were severe, the bone height and thickness may become insufficient, making immediate placement difficult.
The treatment discussed in such cases is a bone graft implant. It is more accurate to understand it as a process of rebuilding the foundation so that the implant can withstand force without loosening. In particular, the upper molar area is more likely than other areas to have bone deficiency, because over time the maxillary sinus, an empty space above, tends to descend while the height of the jawbone decreases, which can make the surgical plan more delicate.
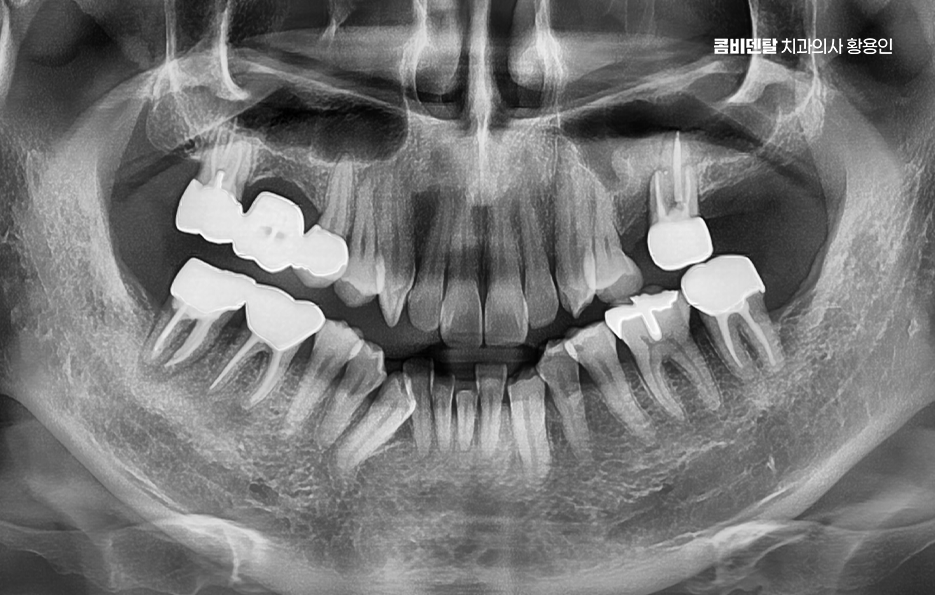
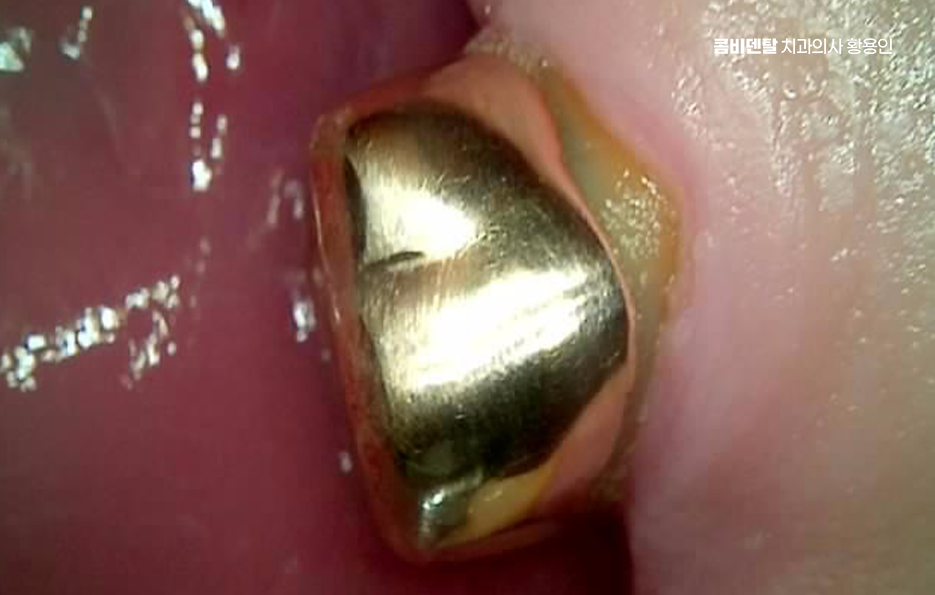
A representative case where sinus lift surgery is needed is also when an implant must be placed in an upper molar site and the bone height is not sufficient. In such cases, the space is lifted and the bone is reinforced because placing the implant as-is is likely to result in inadequate fixation.
This situation is more likely to arise the longer it has been since the tooth was extracted. Bone that no longer receives stimulation after a tooth is lost is gradually resorbed, and in the upper jaw, the maxillary sinus space can expand as well, causing the conditions for implant placement to deteriorate more quickly than expected.
Bone graft implants are also often needed when teeth are lost due to periodontal disease. Gum inflammation may not only have weakened the tooth but also dissolved the surrounding bone, so the foundation must be rebuilt before the implant can be placed. Teeth that were difficult to extract or had significant inflammation around the root also tend to leave bone defects. In such cases, even if the gums appear to have healed on the outside, the internal structure may have collapsed, making stable placement difficult without additional reinforcement.
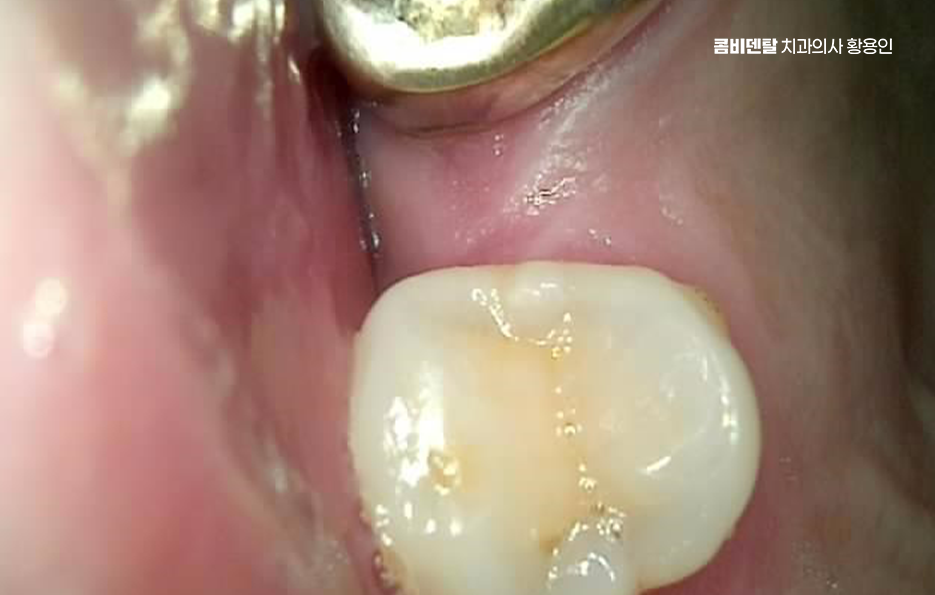
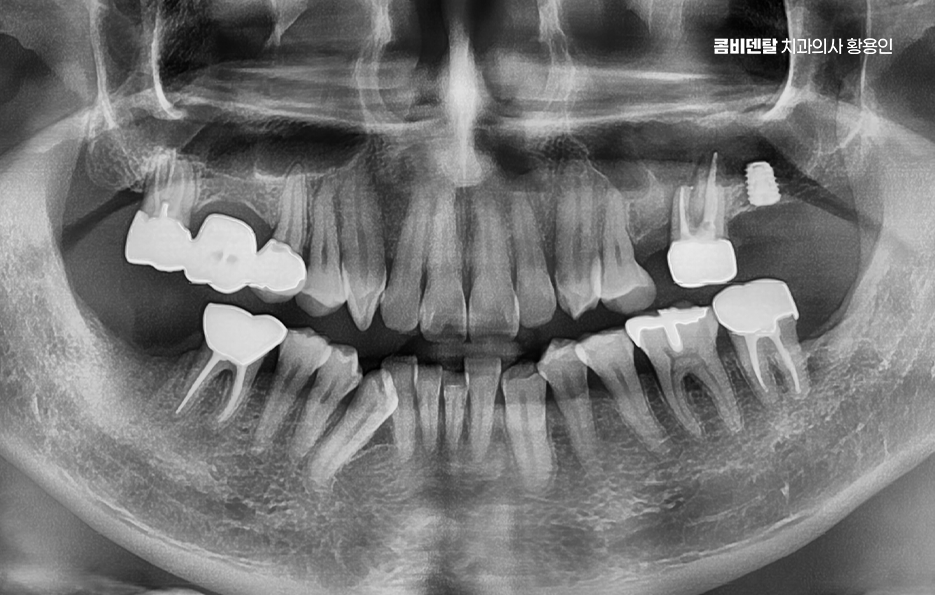
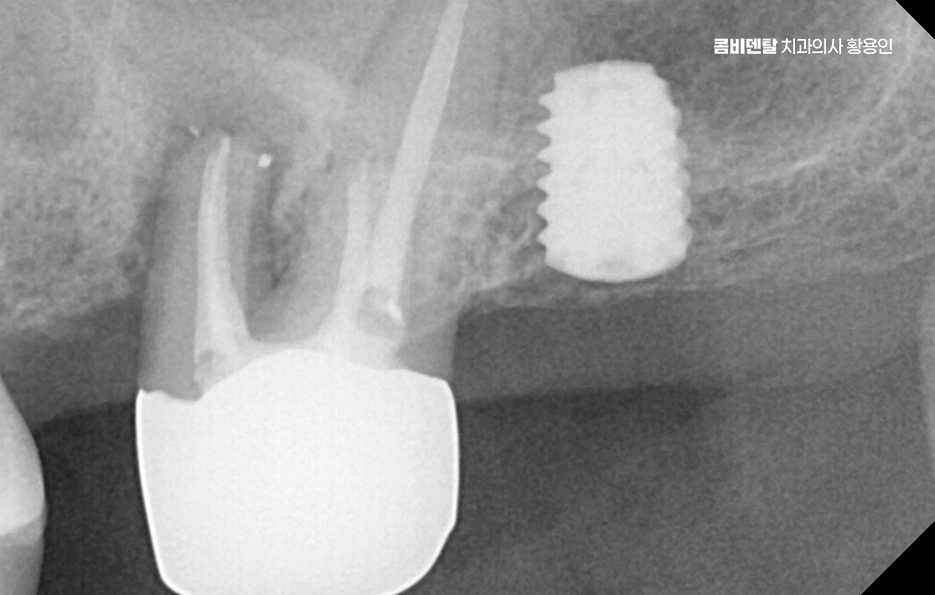
Bone graft implants are not performed in the same way for everyone. If the amount lacking is not large, the bone may be reinforced at the same time as implant placement. If the defect is substantial, the bone graft may be done first, followed by a period of healing before placement. Sinus lift surgery also has more than one approach: if only a little bone is missing, a relatively simple method may be possible, but if the deficiency in height is significant, a lateral approach may be needed to lift the sinus membrane and place bone graft material.
That naturally leads to the question of how long a bone graft implant can be expected to last. There is no single definitive answer, but in the end, the lifespan of a bone graft implant is influenced more by post-placement care and the stability of the surrounding tissues than by the surgical difficulty itself.
It is true that there are more things to be careful about than with an implant placed in a site where the bone is excellent from the beginning. However, it cannot be said that a bone graft or sinus lift procedure necessarily shortens the lifespan of a bone graft implant, and if the treatment plan and aftercare are well matched, there are plenty of cases that remain in good condition for a long time.
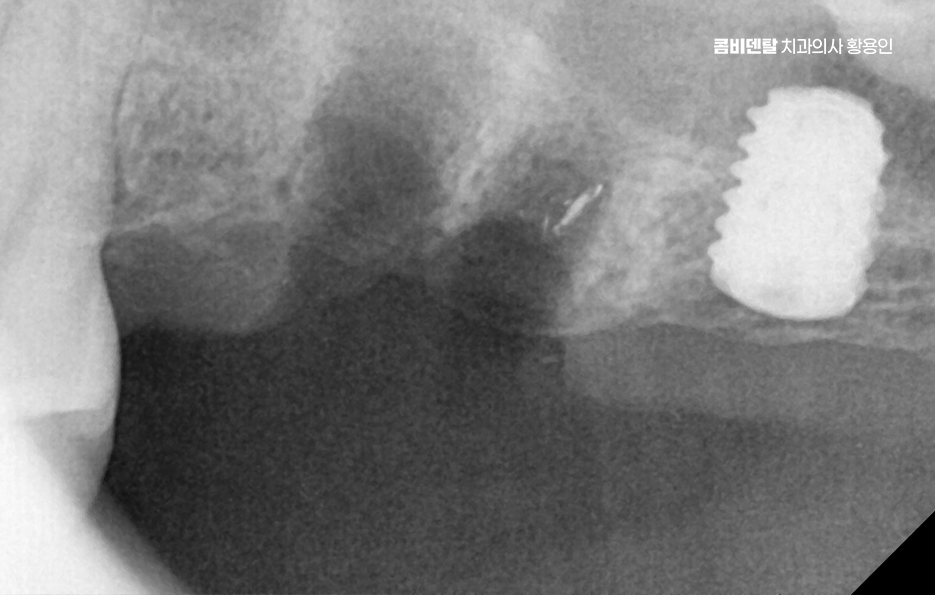
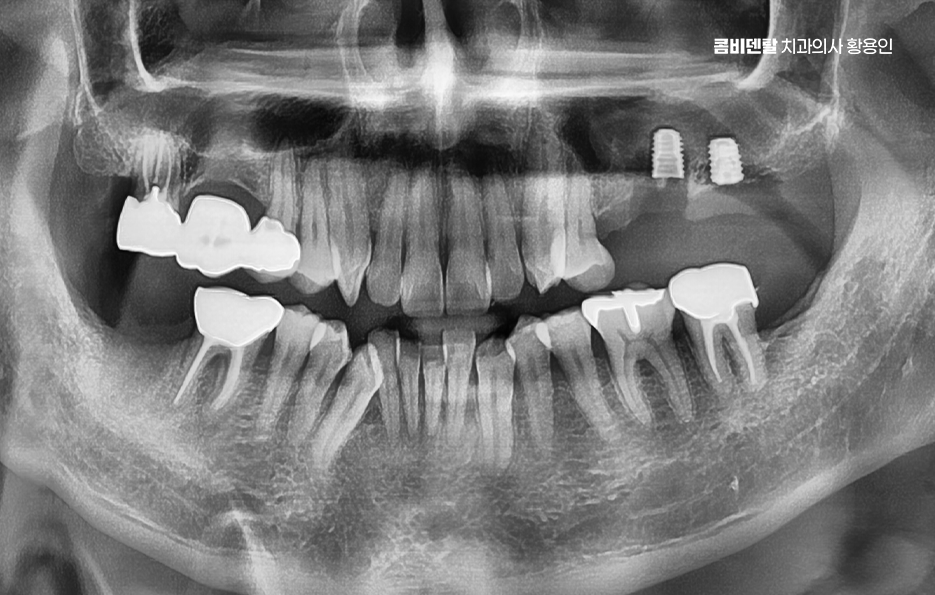
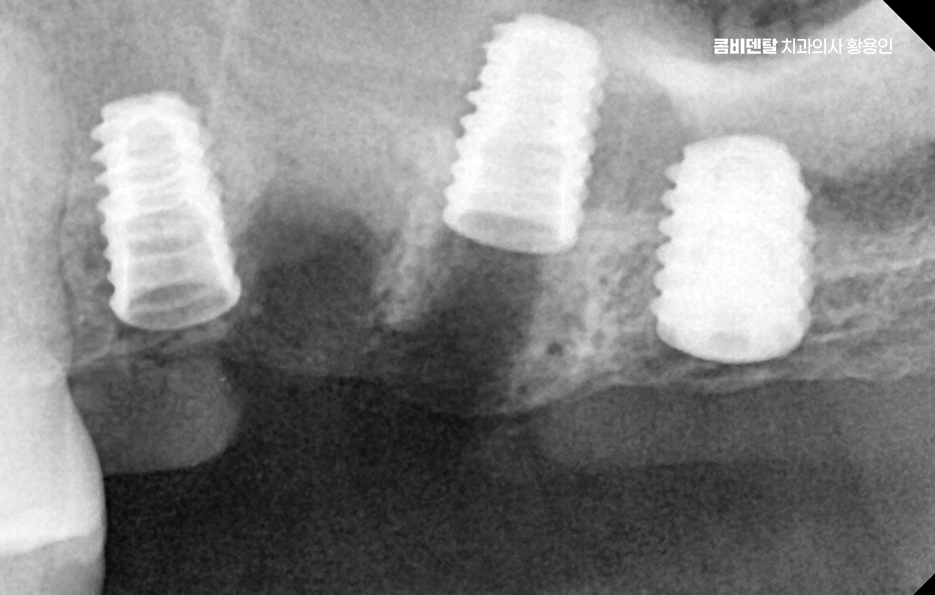
What matters even more is how well the grafted bone settles and whether the gum tissue around the implant remains healthy. Long-term stability can depend more on whether the area is maintained so that force is distributed evenly without inflammation after surgery, rather than on the immediate post-operative period.
A common cause of reduced bone graft implant lifespan is peri-implantitis. Regardless of whether a bone graft was performed, if bacteria accumulate at the gum margin and inflammation keeps recurring, the bone and support structure that were so carefully built up can weaken again. Smoking is also a major variable. Cigarettes reduce blood flow to the gums and worsen the healing environment, making them unfavorable for early recovery and also making inflammation easier to develop later during the maintenance phase. For that reason, smoking can be considered one of the main lifestyle factors that undermine the lifespan and long-term stability of bone graft implants.
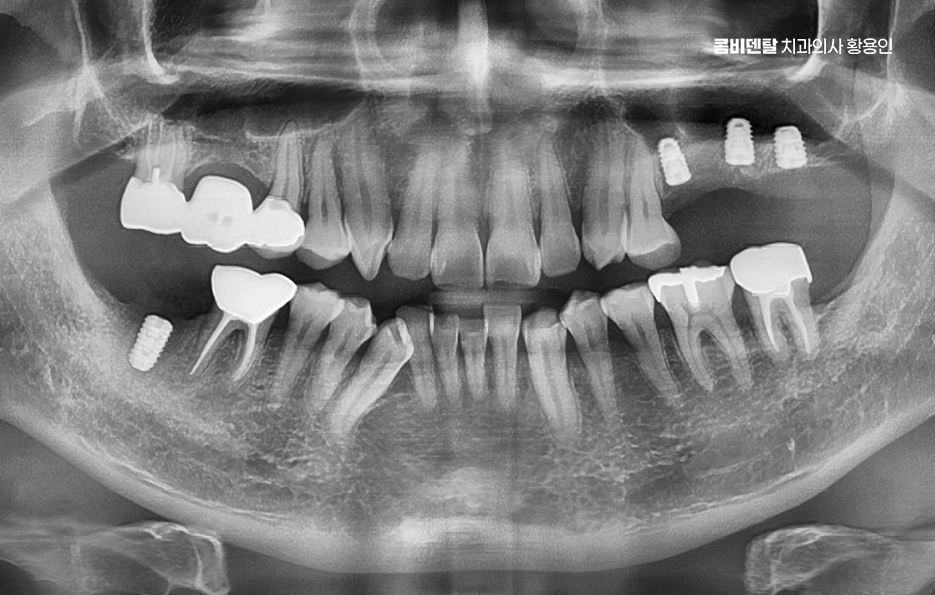
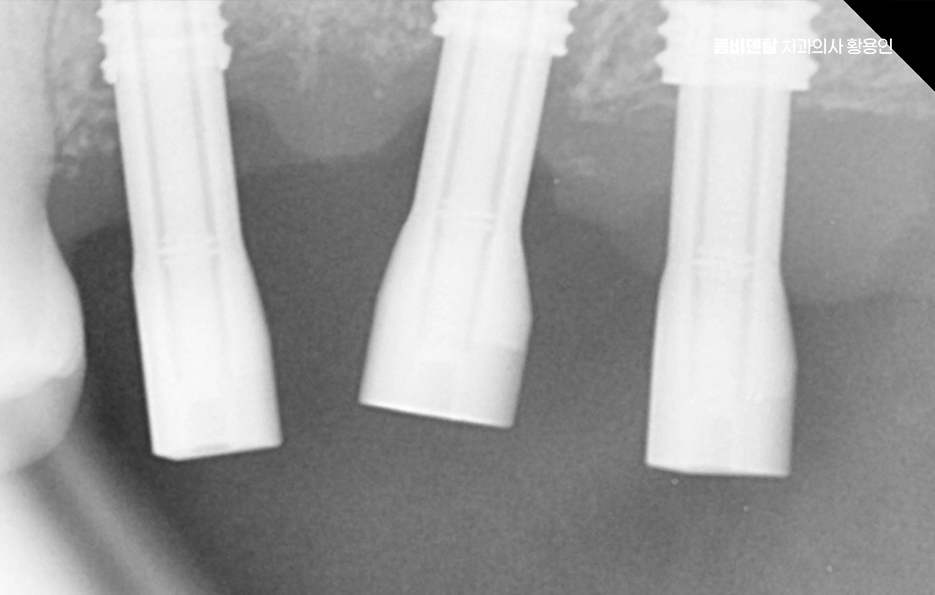
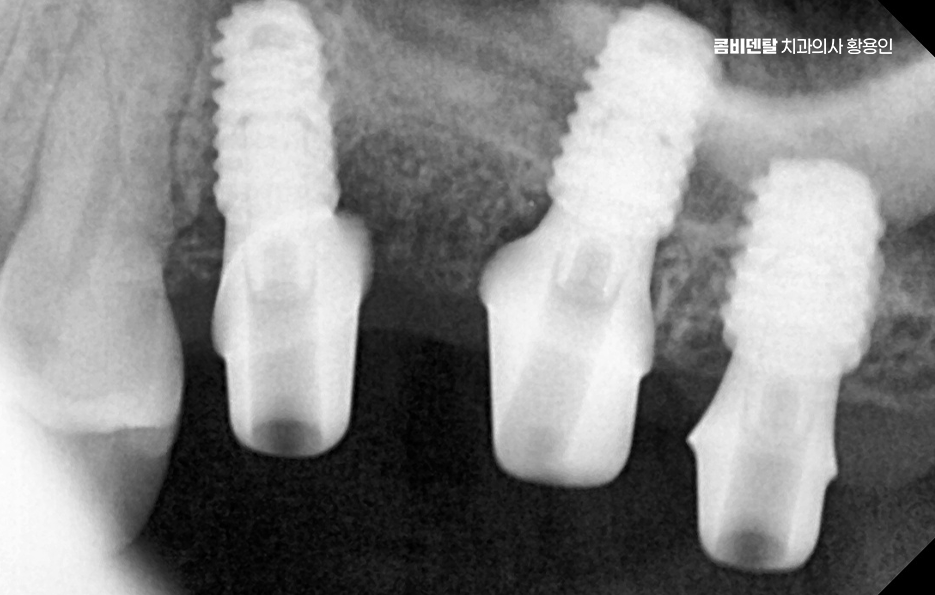
The important point in maintaining the lifespan of a bone graft implant is not some special secret, but not overlooking the basics. Rather than stopping at brushing alone, you should carefully clean the border around the implant using interdental brushes or dental floss so that food debris and plaque do not remain for long. Regular checkups are also very important. Even if a bone graft implant looks fine on the outside, the condition of the gums and bone inside must be monitored consistently, so not postponing checkups even when there is no pain can make a big difference in preserving its lifespan.
In conclusion, a bone graft implant can be seen as a preparation process that first creates the conditions for an implant to be used for a long time. Its expected lifespan is also determined by the current condition of the jawbone, gum health, and lifestyle management. I hope you understand the structure and principles of implants well and approach treatment with a long-term perspective.





 Previous image
Next image
Previous image
Next image





 Previous image
Next image
Previous image
Next image





 Previous image
Next image
Previous image
Next image





 Previous image
Next image
Previous image
Next image

















 Previous image
Next image
Previous image
Next image




 Previous image
Next image
Previous image
Next image




 Previous image
Next image
Previous image
Next image




 Previous image
Next image
Previous image
Next image