Hello, this is Dr. Jo Hyun-woo of 입체성형외과.
I mentioned reconstruction after contour surgery before,
and today I’d like to explain in more detail what materials are actually used in reconstruction surgery.
Problems that can occur after facial contour surgery, such as hollowing caused by excessive bone removal, asymmetry, or nonunion, are addressed using various materials and techniques to help restore functionally and aesthetically satisfying results.
In particular, recent advances in 3D printing technology have made a major contribution to the field of facial contour reconstruction and have opened a new era of personalized reconstruction.
Reconstruction Using Autologous Tissue
The most ideal reconstruction material is still the patient’s own tissue.
Autologous tissue has the advantages of no rejection reaction, strong resistance to infection, and a high engraftment rate due to good blood supply.
I briefly explained fat grafting surgery for recovering overcorrection.
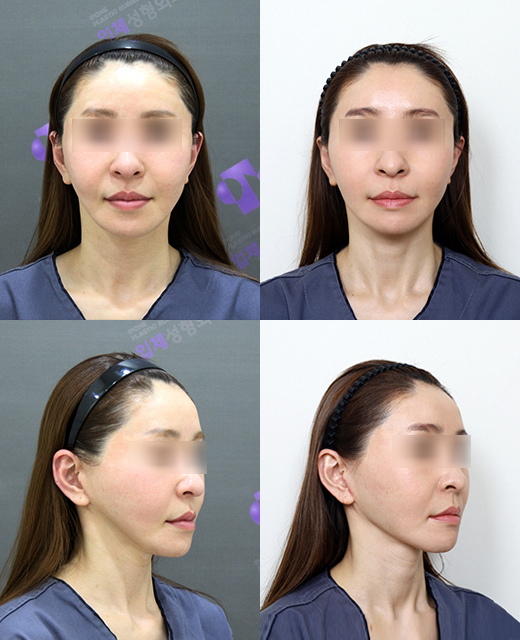
A patient who underwent fat grafting to the square jaw area to improve hollowing caused by excessive square jaw reduction surgery
Autologous fat grafting is mainly used to correct minor depressions or irregular contours.
It involves refining autologous fat harvested from areas such as the abdomen or thighs and grafting it to the needed area.
It is relatively simple and recovery is quick, but the engraftment rate of the grafted fat can vary from person to person, and some of it may be absorbed.
Second, there is autologous bone grafting.
When the defect is large or strong structural support is needed, the patient’s own bone is harvested and grafted.
It is usually taken from the ribs or pelvic bone, and once it engrafts after transplantation, it fuses with the surrounding bone, offering the possibility of long-lasting effects.
However, scars may remain at the donor site, and there is also a possibility of resorption or shape changes.
Third is autologous cartilage grafting.
It is mainly used for nose reconstruction or subtle contour correction, using cartilage harvested from the ear or nasal septum.
It is effective for creating soft shapes or adding subtle volume.
Reconstruction Using Artificial Implants
Recently, when autologous tissue alone makes it difficult to secure sufficient volume, or when harvesting autologous tissue is difficult due to the patient’s condition, artificial implants can be used.
In recent years, materials with excellent biocompatibility and the ability to be manufactured in various shapes have been developed and used.
- Methyl methacrylate (PMMA): Also called bone cement, it can be mixed directly during surgery and shaped into the desired form.
It provides firm and solid support and has the advantage of being relatively inexpensive.
However, it may generate heat during the reaction, and it has the disadvantage of being difficult to remove later.
At present, this product is not being imported into Korea, so it does not seem to be used much.
- High-density polyethylene (Medpor): It has a porous structure, allowing surrounding tissue to grow into it and adhere, which increases stability.
It can be processed into various shapes and is clearly visible on X-rays, making postoperative confirmation easier. However, it may be vulnerable to infection and difficult to remove.
In the past, Medpor was widely used, but with the arrival of 3D printers, it seems to have gradually become a less commonly used material.
- Silicone: A material that has long been widely used in various plastic surgeries.
It is soft and easy to process, making it easy to create the desired shape, and it has the advantage of being relatively easy to remove.
However, a capsule may form, it is vulnerable to external impact, and there is also a possibility of shifting or deforming.
This is the material I currently use mainly for correction surgery for sunken eyes.
Creating implants with 3D printers to compensate for these drawbacks has made surgery remarkably simpler.
- Titanium: It has excellent biocompatibility and high strength, so it is mainly used in plate or screw form and serves as an auxiliary material for fixing fracture sites or for bone grafting.
It is stable and harmless to the human body, but it is difficult to directly provide the volume needed for reconstruction.
It also has the drawback of appearing like a cyborg on X-ray images, so in my case, I do not use it as a reconstruction material.
- PCL (Polycaprolactone): PCL is a biodegradable polymer that is gradually broken down and absorbed in the human body.
It is soft and flexible, making it easy to process into various shapes, and it is a material with strong potential for use in personalized implant fabrication, especially when combined with 3D printing technology.
PCL may induce a process over time in which it is replaced by autologous tissue, allowing for more natural reconstruction results.
It also has excellent biocompatibility, and compared with other polyesters, it produces fewer acidic byproducts during degradation, which can help reduce inflammatory reactions.
PCL can be used alone to help maintain volume, and it can also be used as a bone formation-inducing membrane.
However, PCL alone may lack the ability to directly induce bone formation, so it is often mixed with bone formation-promoting substances such as beta-TCP (β-TCP) or bioactive glass.
It takes a long time to fully absorb, and shape changes or possible inflammatory reactions during the absorption process must also be considered.
The New Era of Personalized Reconstruction with 3D Printing Technology
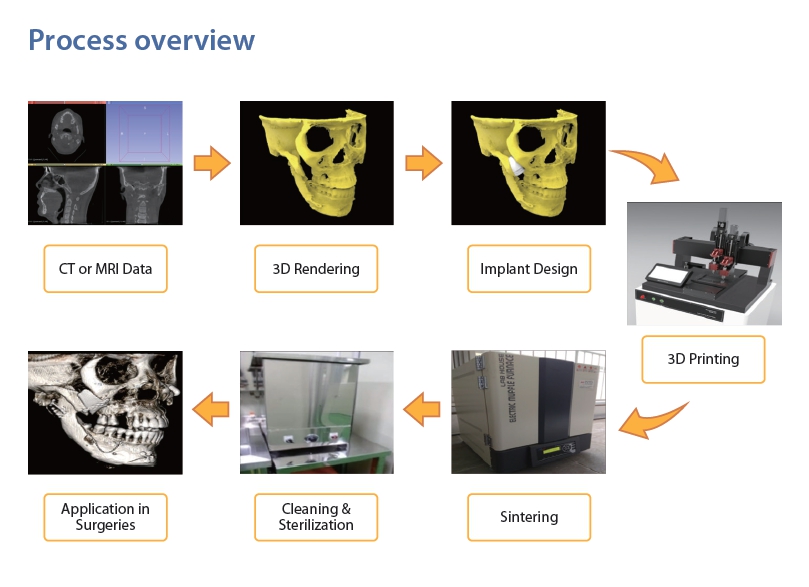
The most notable technology in the field of facial contour reconstruction recently is 3D printing.
Based on the patient’s CT data, 3D printing technology accurately reproduces three-dimensional models of bone or soft tissue and is used to create personalized implants and guides that are precisely tailored to each individual.
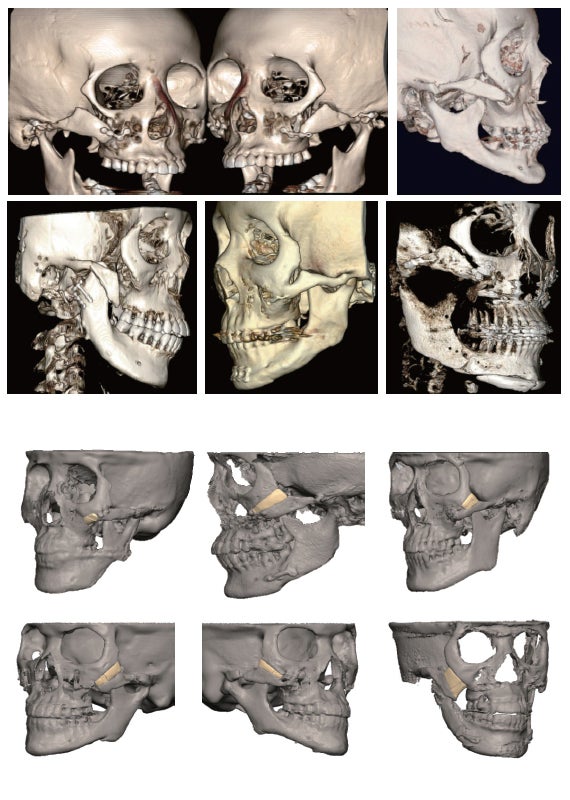
- Accurate diagnosis and surgical planning
By converting the patient’s CT data into a 3D model, it is possible to accurately understand the anatomical structure and extent of the defect in the surgical area.
Through this, virtual surgical simulation can be performed before surgery to find the optimal reconstruction method and minimize errors that may occur during surgery.
According to a study published in the 2020 Journal of Craniofacial Surgery, surgical planning using 3D printed models was shown to help shorten surgery time and improve surgical accuracy compared with traditional methods.
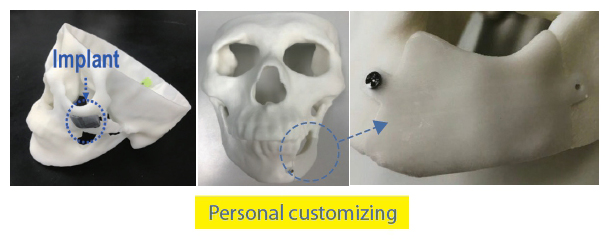
- Custom implant fabrication
In the past, ready-made implants had to be trimmed to fit the patient or combined from multiple pieces, but with 3D printing technology, custom implants that perfectly match the shape and size of the patient’s defect can be created. Implants are mainly made by 3D printing materials such as titanium, PEEK (Polyetheretherketone), and PMMA.
PEEK has excellent biocompatibility, strength similar to bone, and radiolucency, which means there are fewer restrictions on postoperative CT or MRI scans.
PCL is gaining attention as a 3D-printable biomaterial, and thanks to its biodegradability, active research is being conducted on natural reconstruction through autologous tissue induction. PCL has a low melting point (55–60°C), making it suitable for 3D printing, and its excellent flexibility and tensile strength make it appropriate for scaffold fabrication for craniofacial bone reconstruction.
Bioactive glass ceramic (BGS-7) is composed of minerals such as calcium, silicon, sodium, and phosphate ions that naturally exist in the human body, and it bonds with living tissue. It is a non-toxic and proven safe material, and according to research results, BGS-7 induced successful osteogenic differentiation of human mesenchymal stem cells (hMSCs).
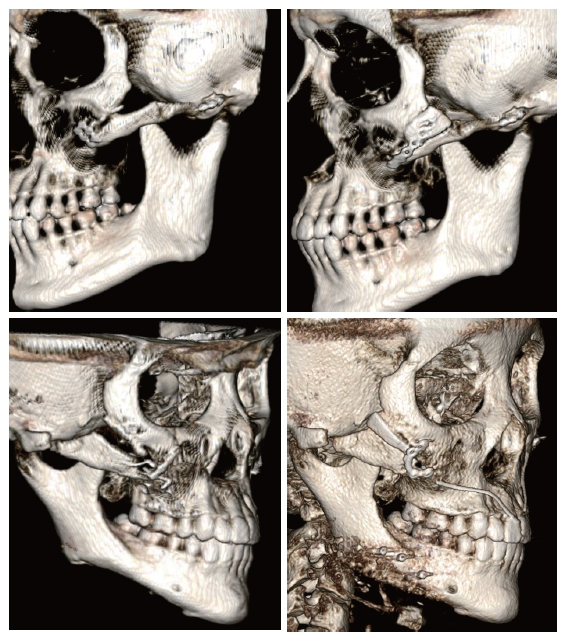
- Surgical guides and jigs
3D printing technology is used not only to make implants, but also to create surgical guides or jigs that guide the exact osteotomy line or implant placement position during surgery.
Using these guides allows consistent and accurate results even in complex reconstruction surgeries, regardless of the surgeon’s level of experience.
Of course, 3D printing technology is not a magic key that solves everything.
There are still limitations, such as high production costs, the need for skilled medical staff, and the need for additional research on the long-term biocompatibility and stability of some materials.
In addition, it has limitations in soft tissue reconstruction, so it is often used in combination with other reconstruction methods such as autologous tissue grafting.
However, 3D printing technology continues to advance, and research on creating artificial tissues and organs using cells or biomaterials through bioprinting is also actively underway. In the future, there may come a time when custom bone or cartilage tissue is created and transplanted using a patient’s own stem cells through 3D printing.
No matter which material or method is used for reconstruction surgery, the most important thing is to accurately understand the patient’s individual condition and needs and provide the best solution accordingly.
Facial contour reconstruction is an important surgery that restores not only aesthetic aspects but also functional aspects such as chewing and speech, as well as psychological stability.
Based on the latest technology and a variety of materials, our clinic will continue to research and strive to contribute to improving our patients’ quality of life.
Thank you.




