A clear, smooth complexion
is an important factor
that shapes one’s appearance.
However, as we age
or are exposed to external irritation,
various pigmentation conditions
can appear on the skin.
One of the most representative of these is melasma.
Melasma is found more often in women,
and it is characterized by
brown or grayish-brown pigmentation
appearing symmetrically on the face.
Beyond being a simple cosmetic concern,
it can lead to reduced confidence and mental stress,
so many people continue to look for ways to manage it.
Melasma is not just a blemish on the skin surface,
but a pigment disorder caused by a combination
of factors such as excessive activation of melanocytes,
skin barrier damage, and hormonal changes.
Therefore, proper understanding and personalized care
are more important than anything else.

What Is Melasma?
Medically, melasma is a pigmentary disorder
in which melanin pigment is overproduced
and deposited on the skin surface.
It usually appears symmetrically on the forehead, cheeks,
cheekbones, around the nose, and around the mouth,
and is seen as brown or grayish-brown patches
with relatively unclear borders.
Melasma can be broadly divided into two types.
Epidermal melasma: This occurs when melanin is deposited mainly in the epidermis,
and the brown color appears relatively distinct.
Dermal melasma: This occurs when melanin is deposited
in the dermis as well,
appearing bluish or light brown
and is more difficult to treat.
In particular, once melasma develops,
it is difficult for it to disappear completely on its own,
so consistent and systematic management is essential.
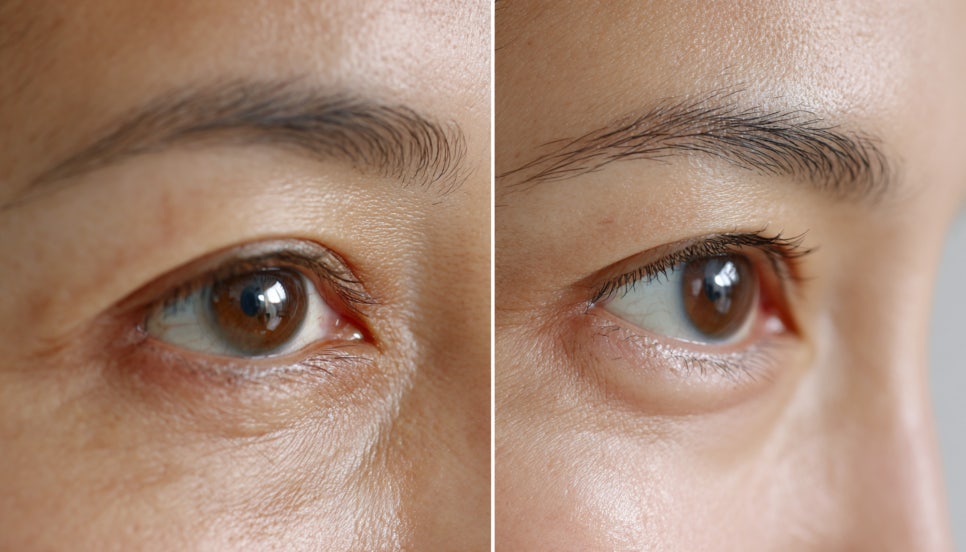
Why Melasma Develops
The causes of melasma are not simple.
Several factors below work together.
UV exposure
Ultraviolet rays (UVA, UVB) are the biggest factor
because they stimulate melanocytes and worsen pigmentation.
If sunscreen is not used
or if you spend a lot of time outdoors,
melasma can develop more easily,
and existing melasma can become darker.
Hormonal changes
In women, melasma can develop or worsen
in relation to hormonal changes such as pregnancy, childbirth,
use of birth control pills, and menopause.
In particular, an imbalance of estrogen and progesterone
is known to stimulate melanocytes.
Genetic factors
If someone in your family has melasma,
the risk of developing it is higher.
Skin type and melanin responsiveness
may also be influenced by genetics.
External irritation and lifestyle habits
Repeated heat, friction, and inflammation on the skin
can worsen melasma.
In addition, lack of sleep, stress, smoking,
and an unbalanced diet can also interfere with melanin metabolism
and cause pigmentation.
Ultimately, melasma can be said to be the result
of a combination of environmental factors
and internal hormonal and genetic characteristics,
rather than a single cause.

How to Manage Melasma
For melasma, the term “management” is more appropriate than “treatment.”
Because it is difficult to completely remove melasma
in a short period once it appears,
the key is to reduce pigmentation over the long term
and prevent new melasma from developing.
Thorough sun protection
Use of topical treatments
Dermatology procedures
Improving lifestyle habits
The Importance of Long-Term Management
Melasma is not simply a skin blemish,
but a pigment disorder that appears
as internal skin conditions and external irritation
accumulate over a long period of time.
Therefore, it is difficult to completely solve
it with short-term procedures or cosmetics alone.
However, if sun protection, lifestyle improvements,
and professional treatment are combined,
melasma can be lightened and new cases can be prevented.
Above all, consistency is important.
Since melasma appears gradually,
management should also be approached
from a long-term perspective.
Through an accurate diagnosis and personalized treatment,
you can restore the skin’s natural health
and a brighter tone,
and this can ultimately lead to regained confidence.