“Doctor, I tend to get canker sores pretty often...
Could it have something to do with my gums not being in good shape?”
Hello, I’m Kim Tae-hyung, the chief doctor at Blanche Dental Clinic.
When I’m doing scaling or treating cavities, people sometimes ask questions like this offhand.
They don’t come to the dental clinic specifically because of canker sores,
but while sitting in the chair with their mouths open, they suddenly remember it and cautiously ask, “Can you check this at a dental clinic too?”
If you search online, there are so many methods—salt water, ointments, patches, vitamins...
Yet some people recover quickly with the exact same approach, while others don’t heal for weeks or get better only to have it come back again.
Just reading online reviews often makes it even more confusing about what you should actually do.
As a dentist, I’ll say this plainly: for people who keep getting canker sores, the problem is usually that they’ve identified the wrong “cause” before even thinking about the “fastest way to heal.” Today, I’ll start with the cause and then organize practical ways to deal with it depending on the situation.

Why do canker sores happen?

Most people think it’s “because the immune system is weak.” That’s not wrong, but that’s not all there is to it.
When I examine the mouths of patients who say their canker sores keep coming back, surprisingly, the problem is often the oral environment itself. For example, an old restoration edge may keep scraping the mucosa, a malocclusion may cause them to habitually bite the inside of the cheek, or tartar may accumulate around the gums and keep the area in a state of chronic inflammation.
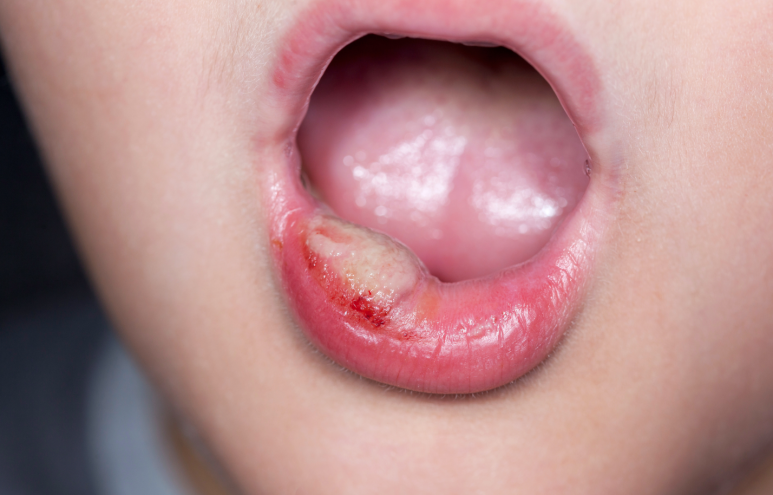
The main causes of canker sores can be summarized like this.
First, physical irritation.
Orthodontic appliances, dentures, sharp edges on old crowns, or habits like repeatedly biting the inside of the cheek can injure the mucosa and cause ulcers in those spots.
Second, oral hygiene issues.
When there is a lot of tartar and bacteria, even a small wound can easily develop into an ulcer.
There are quite a few people who haven’t had scaling for more than a year and have unusually frequent canker sores.
Third, overall physical condition.
Lack of sleep, stress, nutritional deficiencies such as vitamin B12 or iron deficiency, and hormonal changes can all reduce the mucosa’s ability to recover.
Tongue canker sores and gum canker sores — the cause differs by location
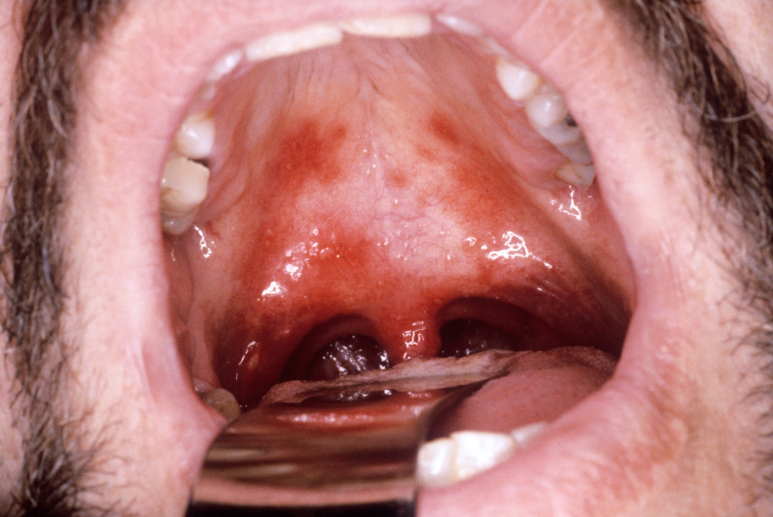
When I look at the mouths of people who say, “I keep getting them on the side of my tongue,” I often find that the inner surface of the lower molars has worn down sharply and is continuously irritating the tongue. They usually have no idea.
For people who keep getting them on the gums, there is a high chance that tartar buildup or a problem with how a restoration fits is hiding underneath.
Simply applying ointment won’t solve the cause, which is why it keeps recurring in the same place.
During consultations, when I ask, “Do you chew mostly on one side?” a lot of people say, “Hmm... I never really paid attention, but now that you mention it, I think I may only chew on the right side.” This kind of one-sided chewing habit also repeatedly puts stress on one area of the mucosa.
How to heal canker sores fast depends on the situation
Not all canker sores are the same.
Because the way to handle them changes completely depending on the condition, it’s best to first check which situation applies to you.
| Category | Common aphthous canker sores | Canker sores that require a dental visit |
|---|
| Size | Small ulcers under 1 cm | 1 cm or larger, or multiple at once |
| Duration | Heals naturally within 7–14 days | Does not heal for more than 2 weeks |
| Frequency | Occasional, once or twice | Repeats 2–3 times or more per month |
| Location | Different place each time | Keeps recurring in the same place |
| Response | Ointment, patches, salt-water gargling | Oral exam needed to identify the cause |
If you fall into the left column, over-the-counter ointments or patches are usually enough to manage it.
When the pain is severe, applying a thin layer of a steroid ointment (such as Oramedy) over the ulcer can help, and patch-type products reduce irritation during meals.
The concentration matters for salt-water gargling. About half a teaspoon of salt in 200 ml of lukewarm water is enough.
If it’s too concentrated, it can irritate the mucosa and actually make things worse.

The problem is when you fall into the right column. In that case, no matter how much ointment you apply, it won’t help.
If it keeps recurring in the same spot, that means there is a source of physical irritation there, and an ulcer that doesn’t heal for more than two weeks may not be a simple canker sore.
Mucosal diseases, autoimmune diseases, and, in rare cases, early oral cancer lesions can also start out looking similar to canker sores.
For recurring canker sores, you ultimately need to look at the oral environment
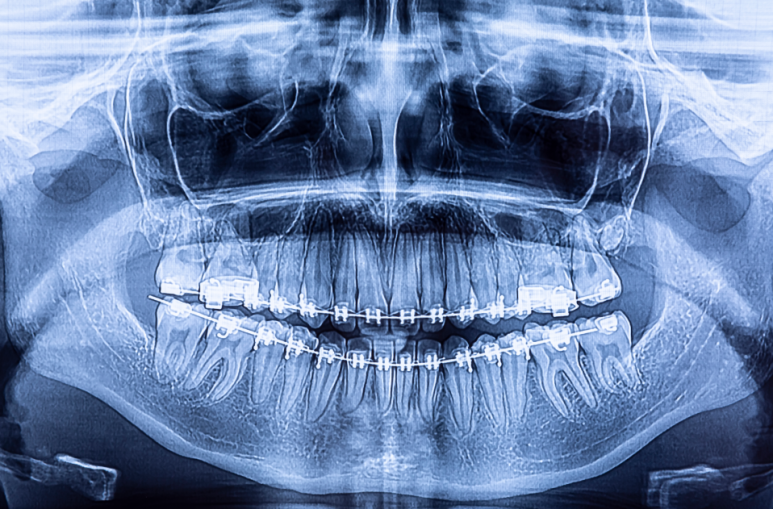
In fact, with just one X-ray and one oral examination, you can immediately check whether the cause of recurring canker sores is inside the mouth or not.
Before brushing it off as “maybe my immune system is weak,” checking the oral environment itself may be a much faster solution.
The fit of restorations or crowns is also often the cause of mucosal irritation.
If, while reading this, you’d like to know more about crown treatment, please refer to the post below as well.
What first seemed like a canker sore that would be solved with just one ointment is, in many cases, actually a problem that started from the edge of an old restoration or a piece of tartar. If you’re only piling up ointment costs, now may be the time to take a closer look at the cause.
Where that cause is in your mouth is something that can only be identified by looking directly.
If you’re coming in for scaling, just mention it to me and I’ll check it with you. You don’t need to make a separate appointment.
If you have any questions, feel free to ask in the comments or by phone.
This was Blanche Dental Clinic in Gangnam. Thank you.









