“Doctor, do wisdom teeth really have to be removed?
I heard there are people who don’t have them removed...”
I’m Kim Tae-hyung, the chief director of Blanche Dental Clinic.
When a wisdom tooth is found on an X-ray while visiting for cavity treatment or scaling,
nine out of ten patients ask this almost immediately. That’s because the pain associated with wisdom teeth is naturally very frightening.
It is true that some wisdom teeth do not need to be removed.
I also do not want to remove teeth that do not need to be extracted. However, the situation changes if the tooth is impacted.
And depending on what kind of “impaction” it is, the decision between extraction and observation changes completely.
To be honest as a dentist,
making this judgment properly is not possible with only the standard X-ray taken for cavity treatment.
Today, I’ll organize the criteria exactly as I explain them in the treatment room.

Impacted wisdom teeth: why are they a problem if they don’t hurt?
An impacted wisdom tooth refers to a wisdom tooth that is completely buried in the jawbone or has only partially emerged and has not properly come in. It either lacks space or has come in at the wrong angle and stopped halfway.
The problem is that you can’t see this condition.
On the surface, everything may seem fine, but inside the bone it may be pushing against the molar next to it, or food may be getting trapped in the gap between the wisdom tooth and the gum, allowing cavities to slowly progress. By the time symptoms appear, it is not uncommon for the adjacent molar to already be damaged.
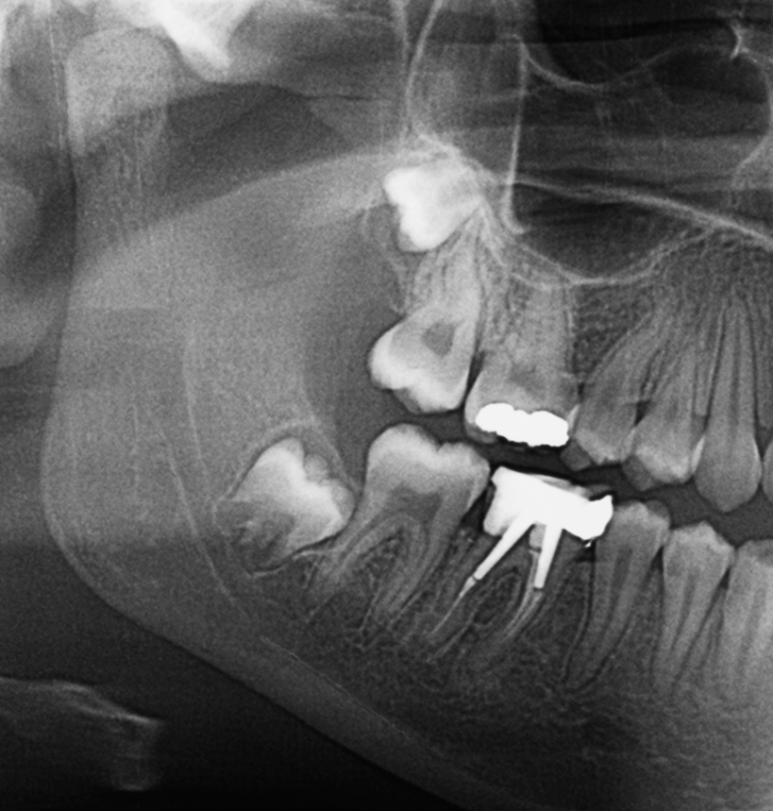
When I look at an X-ray in the clinic, there are cases where I ask, “It doesn’t hurt right now, does it?”
The patient says yes, but in the image you can see the wisdom tooth digging into the root area of the adjacent molar.
And one more thing: as we get older, the bone becomes harder, which increases the difficulty of extraction and the recovery period.
For an impacted wisdom tooth with problems, removing it now is less painful and less complicated than removing it later.
Cases where it should be removed vs. cases that can be monitored
Not all impacted wisdom teeth need to be removed. I also judge, case by case, whether to extract or monitor them.
| Category | Cases where removal is needed | Cases that can be monitored |
|---|
| Wisdom tooth angle | Lying sideways and pushing the molar in front | Standing upright or at a harmless angle |
| Gum condition | Partially covered, creating a pathway for food and bacteria | Completely covered with no surrounding inflammation |
| Effect on adjacent molar | Damage such as cavities or root resorption is progressing | No effect on nearby teeth |
| History of inflammation | Repeated gum swelling and pain | No history of inflammation |
| Cyst findings | A cyst around the wisdom tooth is identified | No cyst findings |
The key is not “Does it hurt right now?” but “Is the structure likely to cause problems later?”
If the angle is wrong and it is pushing on the adjacent tooth, or if only half the gum covers it and it has become a pathway for bacteria to come and go, then extraction is appropriate even if there are no symptoms.

On the other hand, if it is completely buried in the bone and not affecting anything around it, there is no reason to go through bone removal just to take it out.
Removing a wisdom tooth that does not need to be removed, or leaving one that does need to be removed, are both problems.
Why a standard X-ray is not enough
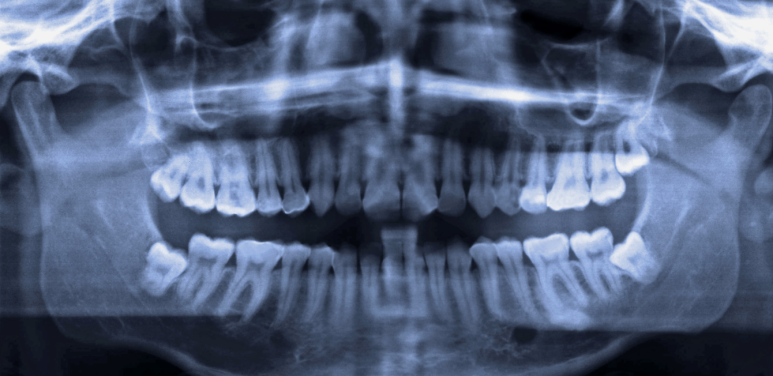
Even on the panoramic X-ray commonly taken during cavity treatment, you can see that an impacted wisdom tooth is present. You can also get a rough idea of its angle and position. So, to a certain extent, you can judge that “the wisdom tooth is lying down, so it should be removed.”
However, that is not enough when deciding accurately whether to remove it, and even less enough when planning a safe extraction.
A panoramic image is a 2D photo, so it is difficult to precisely identify the exact depth inside the bone, the 3D shape of the roots,
and most importantly, the distance to the inferior alveolar nerve.
The inferior alveolar nerve is a thick nerve that runs through the lower jawbone, and in many cases it passes right beneath the roots of an impacted wisdom tooth.
If this nerve is damaged, numbness or altered sensation may occur in the lower lip or jaw, and in rare cases recovery can take a long time.
With 3D CT, the distance between the wisdom tooth and the nerve can be seen in 0.1 mm increments. You can also check at once how many roots there are, the direction in which they are curved, and whether there is a cyst.
This information is necessary to say accurately, “This one needs to be removed” or “This one does not need to be removed right now.” To avoid removing a wisdom tooth that does not need to come out, precise diagnosis comes first.
Even if you were told on a panoramic X-ray that it should be removed, there are cases where 3D CT shows it can be monitored.
Why surgery is different for fully impacted wisdom teeth

A fully impacted wisdom tooth is completely buried in the jawbone and has not emerged at all.
In this case, the difficulty of extraction increases significantly.
The gum often has to be incised, some of the bone covering the wisdom tooth has to be removed, and then the tooth must be divided and taken out in pieces. The scale of the procedure is completely different from a routine extraction.
That is why some local dental clinics say, “Please go to a university hospital,” but even if it is not a university hospital, the procedure can be carried out without issue if the clinic has experience with impacted wisdom tooth extractions and makes a surgical plan based on 3D CT.
If the extraction is performed under sedation, the patient does not retain the fear or memory of pain during the procedure,
so for those who have been postponing treatment because they are afraid of extraction, sedation extraction may be worth considering.
How much pain and swelling occurs after extraction?

The biggest reason people delay impacted wisdom tooth extraction is worry about pain and swelling.
To be honest, saying there will be no swelling and no pain would be a lie. However, the degree varies greatly depending on the extent of the impaction and the scope of the surgery.
If it is a partially impacted tooth, it is not much different from a routine extraction, and daily life is usually possible after 2 to 3 days.
In cases where the tooth is fully impacted and bone removal is involved, swelling may last for about 3 to 5 days, and the pain is usually manageable with the prescribed painkillers.
Many people also worry about food getting stuck in the empty space after extraction, but do not poke at it with a toothpick.
A light rinse is enough to remove it, and it will resolve naturally over time.
If you would like to know more about the recovery process after wisdom tooth extraction, please refer to this post as well.
→ 「How long do pain and swelling last after wisdom tooth extraction? Blanche tells you」
An impacted wisdom tooth is not fine just because it doesn’t hurt, and it is not the case that every impacted tooth must be removed.
However, that decision can only be made accurately after a precise 3D CT evaluation.
This has been Banpo Blanche Dental Clinic. Thank you.
✅ Recommended reading









