Many people think plastic surgery is a department that only handles cosmetic care,
but in fact, plastic surgery specialists across the country
experience and treat a wide range of wounds during their residency training.
Because of the nature of plastic surgery in university hospitals,
a lot of facial trauma and wounds in areas with tissue defects are seen,
In addition, from extravasation caused by IV lines coming out in patients hospitalized in other departments,
to pressure sores in patients with limited mobility,
to wounds in diabetic patients with reduced blood flow…
When you go around general wards and intensive care units
and disinfect (dress) the wounds of all kinds of consultation patients,
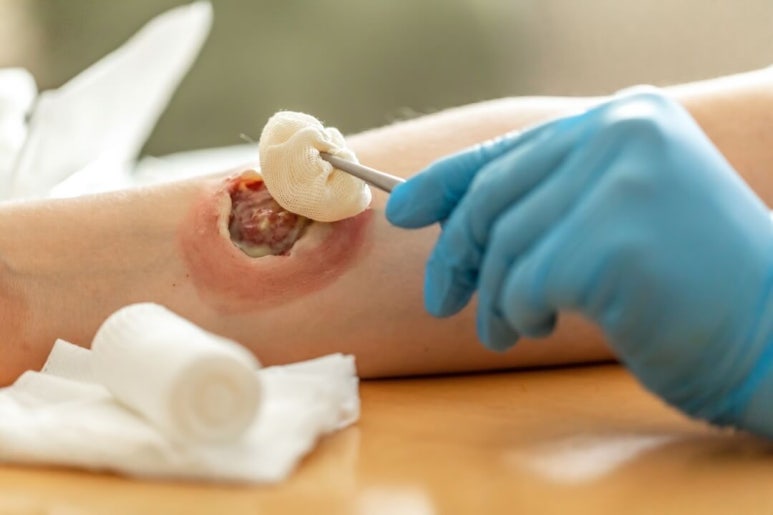
Image of visiting the ward for dressing changes
Unlike the proud image of a plastic surgeon that is consumed in media or public perception,
it feels rewarding to be like a wound cleaner
who goes around the whole hospital.
Blood splattered on the gown is a badge of honor, haha.

As a plastic surgery specialist
and as a wound expert with extensive experience in treating various wounds,
today I would like to introduce not a specific plastic surgery topic,
but rather
how to properly use dressing materials
for wounds.
How to choose dressing materials
- General overview of wound dressing: classification of dressing materials
a) Dry vs. moist dressings
Until the mid-1900s, there was not much difference in wound care,
but after a 1948 academic report showed that a moist environment is more favorable for wound healing,
the evolution of dressing materials began.
Just as a sauna has dry and wet options,
dressing methods are also
divided into dry dressings
and moist dressings.
I will explain this in more detail in the specific sections below.
b) Occlusive vs. open vs. secondary dressings
i) Occlusive dressing
This means covering the entire wound.
From gauze or Band-Aid-type adhesive bandages
to pharmacy-available Duoderm Spot Patch, Mepiform Band, Madeca Band, and more...

Occlusive dressing materials
Most of the dressing materials we commonly see
are occlusive dressings.
Their main purpose is to protect the wound from external physical irritation,
and to maintain an appropriate level of moisture in the wound
to create the best environment for healing.
ii) Open dressing
This means leaving the wound open
without applying a bandage or adhesive strip.
After double-eyelid surgery, applying only an ointment to the upper eyelid area
and leaving it open without attaching any adhesive bandage
is an example of open dressing.
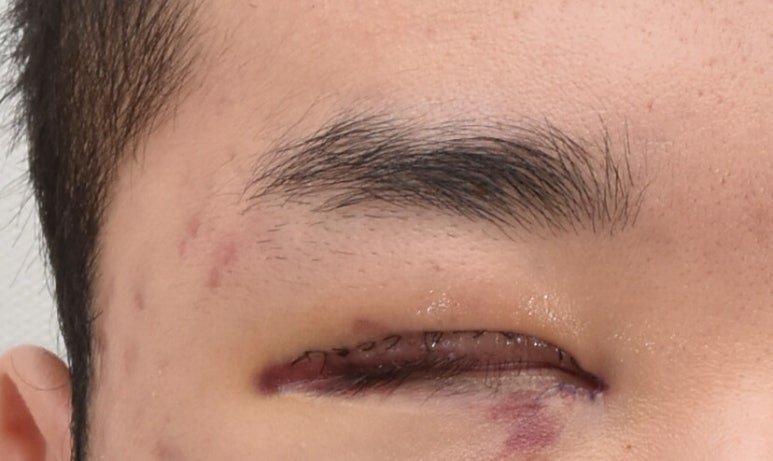
Open dressing on day 3 after incisional double-eyelid surgery
If you attach Mepiform to the double-eyelid area,
it would be very uncomfortable because it would make opening your eyes difficult.
iii) Secondary dressing
This refers to attaching tape to secure the dressing material.
Materials that have their own adhesive strength, like Duoderm, do not need a secondary dressing,
but gauze or how to use Mepiform must be secured with tape like the ones below.
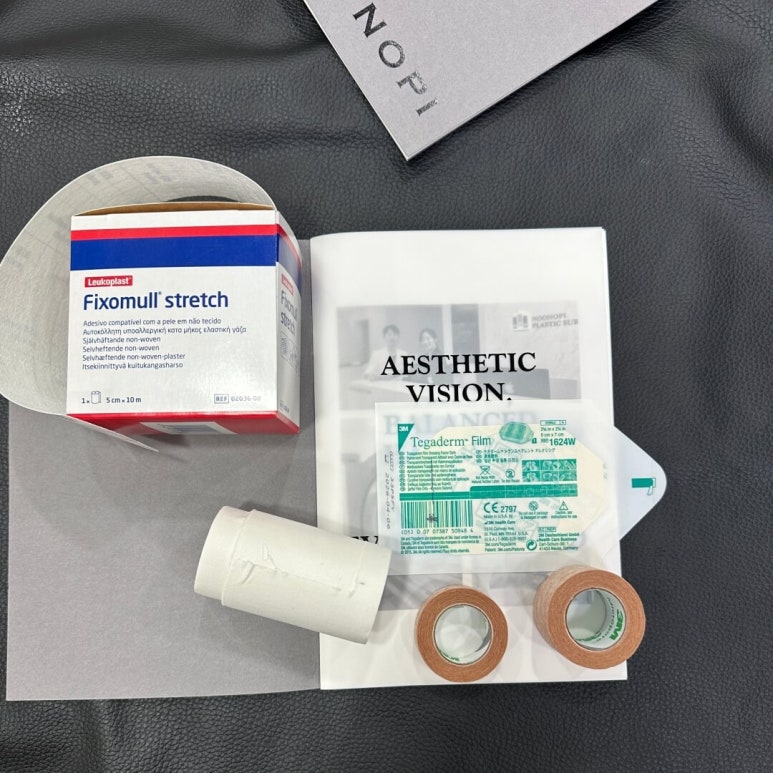
Fixation tapes used for secondary dressings
Wrapping a bandage to secure a dressing material or a splint
also counts as a secondary dressing.
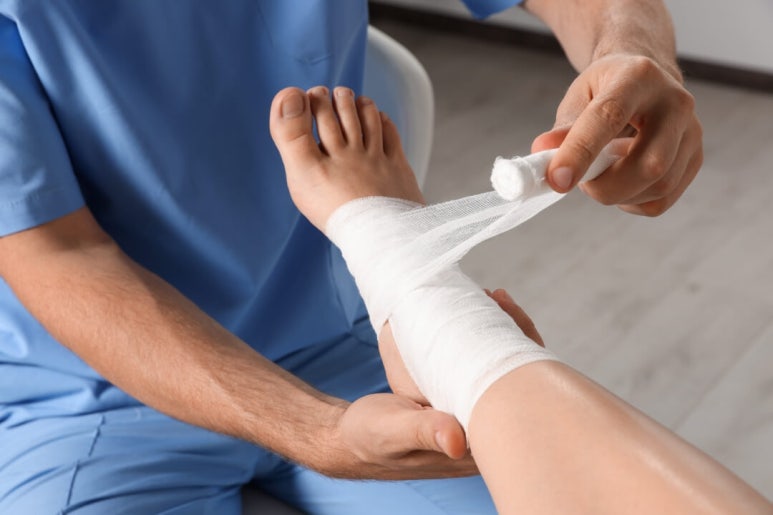
Bandage fixation also counts as secondary dressing
- Detailed wound dressing: how to use dressing materials
a) Moisture is important for wound care!
According to the 2004 issue of the International Wound Journal,
the T.I.M.E. concept for wound bed preparation used in chronic wounds was introduced.
The acronym T.I.M.E. stands for
T (tissue)
I (infection)
M (moisture)
E (edge)
which means...
Among these, what matters when dressing wounds yourself at home
is moisture.
As mentioned earlier, dressing methods are divided into dry dressings and moist dressings,
and the dressing material changes accordingly...
The choice of material
determines the wound’s moisture level,
so using the right material is very important!
b) Dry dressing: e.g., gauze
If a wound is too moist, the surrounding tissue becomes macerated.
In such cases, if you apply a dressing that makes the wound moist, like Mepiform,
the wound edges may become macerated.
Therefore, you need to use a material that absorbs the exudate (wound fluid)
so that the wound does not become macerated....
● Wounds with a fair amount of exudate
● Situations where a moist environment would slow healing
In these situations, dry dressing should be used,
and the most representative cost-effective dry dressing material
is gauze.

The representative dry dressing material: gauze dressing
If you went through plastic surgery residency,
you will have heard of wet-to-dry dressing at least once...
You place wet gauze on the wound, and once the moisture evaporates over time,
when you replace the gauze,
it has the effect of peeling off scabs (unnecessary necrotic tissue)
around the wound, almost as if performing debridement,
so it is sometimes used in university hospital plastic surgery departments.
However, perhaps because the companies that make dressing materials
would not make much profit selling gauze alone,
or perhaps because they sponsored professors’ paper writing, it is hard to know,
but the wet-to-dry dressing method
is now treated somewhat as an old-fashioned approach,
which is the current trend (link).
c) Moist dressing: e.g., Mepiform, Duoderm exudate
As mentioned briefly above,
wounds heal more efficiently in an appropriately moist environment
than in a dry one.
The reason is that the exudate contains
various macrophages and proteolytic enzymes, which work better
when proper moisture is maintained
than in a dry environment.
In other words, moist dressing means
blocking moisture evaporation.
Moist dressings are also divided into several types.
i) Film type

Tegaderm
It is made of a thin acrylic or polyurethane film,
and while gases can pass through, liquids and microorganisms cannot.
Because it is transparent, a wound can be assessed without removing the dressing,
which is an advantage, and in university hospitals it is more commonly used
for secondary dressings or for securing IV lines.
Unlike Duoderm or Mepiform,
it is rarely used as a stand-alone dressing material,
so it is hard to find in pharmacies.
Because it does not allow moisture to pass through,
in eye-level plastic surgery clinics,
it is used more often as waterproof tape for customers.
.
ii) Foam
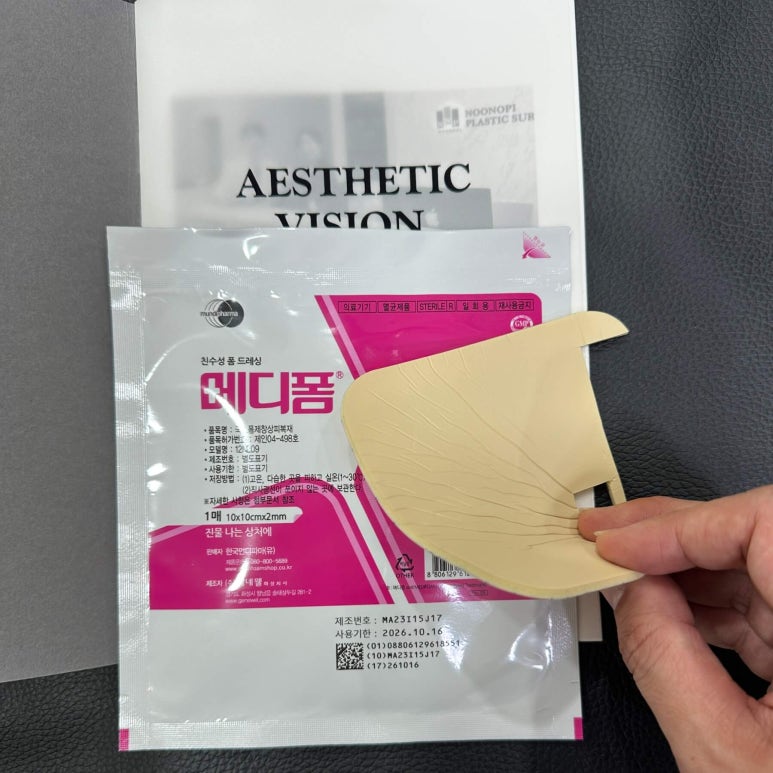
Mepiform, a representative foam dressing
Foam dressing materials represented by Mepiform
are also commonly called moist bandages...
Made of urethane, they have a soft, cushion-like feel,
and among dressing materials that are easy to get at pharmacies,
they are among the best in terms of absorbing exudate.
Therefore,
● wounds with a lot of exudate
● wounds that need moisture retention
● when granulation tissue needs to fill in
● when you are not sure what material to use for wound care
Using Mepiform
will at least not fail.
The downside is that it has no self-adhesive power,
so it must be secured with tape (that is, a secondary dressing is needed)...
For households that cannot easily stock a wide variety of dressing supplies,
having to do a secondary dressing is somewhat inconvenient.
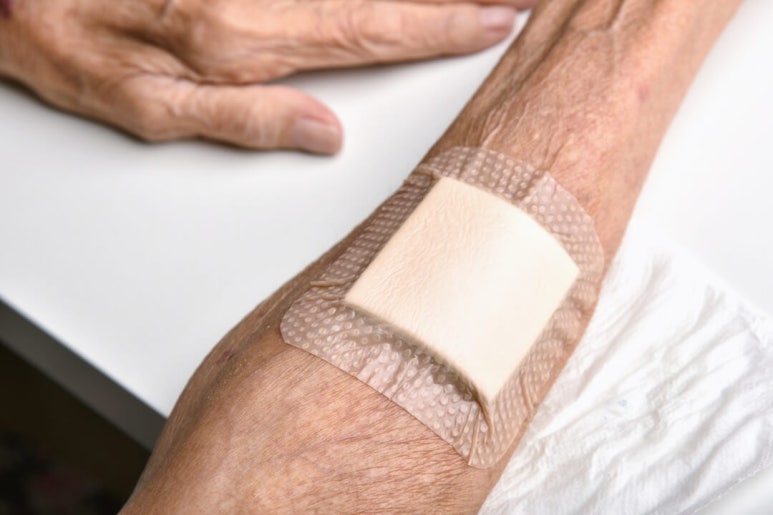
In the case of Mepilex Border, it is integrated, so a secondary dressing is not needed
So there are products on the market in which the securing dressing material and the fixation tape
are combined into one,
making it much easier to use Mepiform for wound care.
But
the shape of a wound’s width, length, and contours
varies from person to person,
and if you try to dress it with a standardized all-in-one product,
it can end up being unnecessarily large or small.
Plastic surgery dressings have to look nice,
like à la carte...
According to one senior resident,
that is why most plastic surgery clinics around Gangnam Station do not actually use integrated dressing materials very often,
and instead often cut Mepiform with scissors to fit the wound size,
then apply a skin-colored adhesive bandage slightly larger than that.
This is absolutely not because they are trying to save money, haha.
Integrated dressings are something you would use when you want to quickly get through dressing changes at a university hospital spending money carelessly....
iii) Hydrocolloid, hydrogel
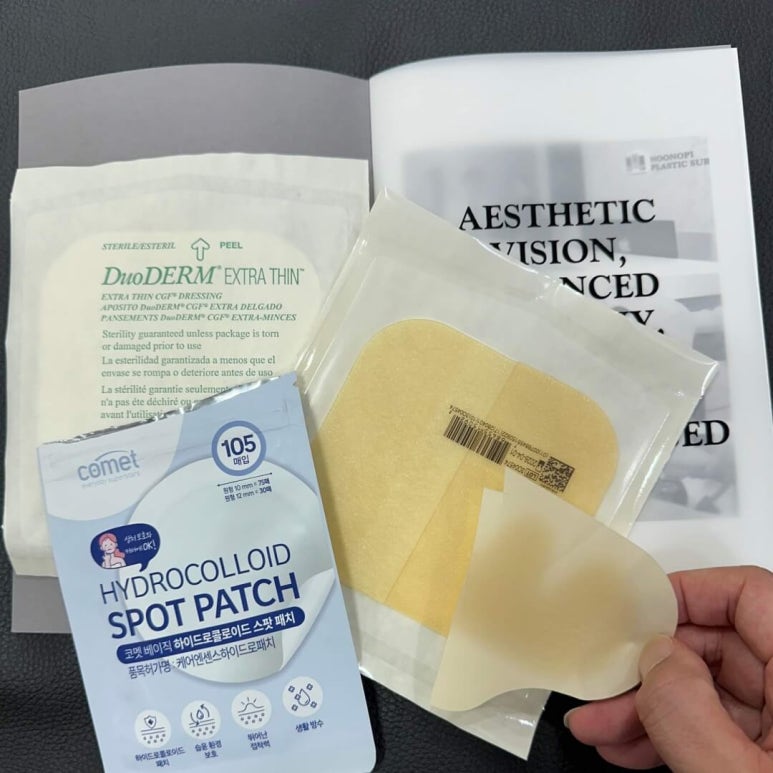
Various hydrocolloid dressings
Duoderm is a representative hydrocolloid dressing material...
Hydrocolloids are sheet products that change into a jelly-like form when they come into contact with exudate.
Unlike Mepiform, they do not have a soft, cushioned feel;
they have a semi-transparent, thick sticker-like texture.
Duoderm is mainly used when
● the amount of exudate is not large
● more skin epithelialization is needed
● skin protection is needed
In other words, to put it simply,
it is used for wounds where the epidermis has peeled away and pink flesh is visible,
and where the amount of exudate is not very large,
while keeping the wound somewhat moist
and using it on wounds where granulation tissue is almost filled in but epithelialization has not yet
sufficiently progressed.
The situation in daily life where you most clearly experience the characteristics of hydrocolloid
is when having moles removed....
After a mole removal procedure, if you put Duoderm on it,
have you ever experienced cloudy exudate collecting the next day?
This Duoderm exudate is
a phenomenon in which the product changes into gel or sol
as it comes into contact with the exudate.
Hydrocolloids do not completely fail to absorb exudate,
but compared with foam dressings,
their exudate absorption ability is lower.
Hydrogel is similar to hydrocolloid, so many people confuse the two,
but the difference is that it is not a sheet material;
it has a jelly-like semi-solid consistency.

Duoderm gel
Although the name is similar,
it should be used in situations that are the opposite of hydrocolloid....
● It is useful for dissolving necrotic tissue (eschar) in dry wounds
Therefore,
it should not be used on wounds with exudate,
and after applying Duoderm gel to the wound like an ointment,
a proper occlusive dressing should be applied.
d) Antimicrobial dressing
An antimicrobial dressing is, simply put,
a dressing material that contains disinfectant.
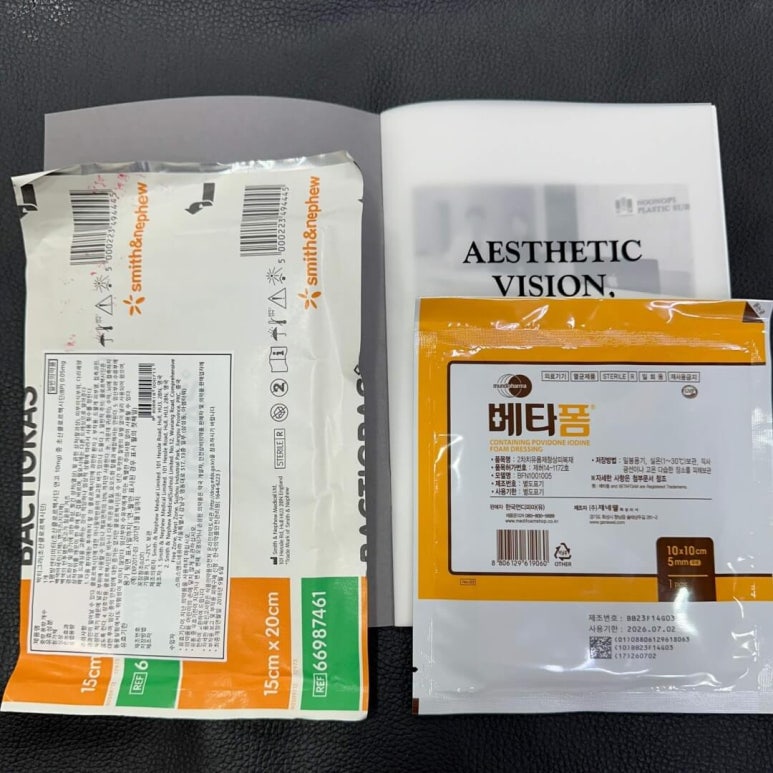
Bactigras, Betafom
Betafom, which contains iodine, is sometimes available at pharmacies,
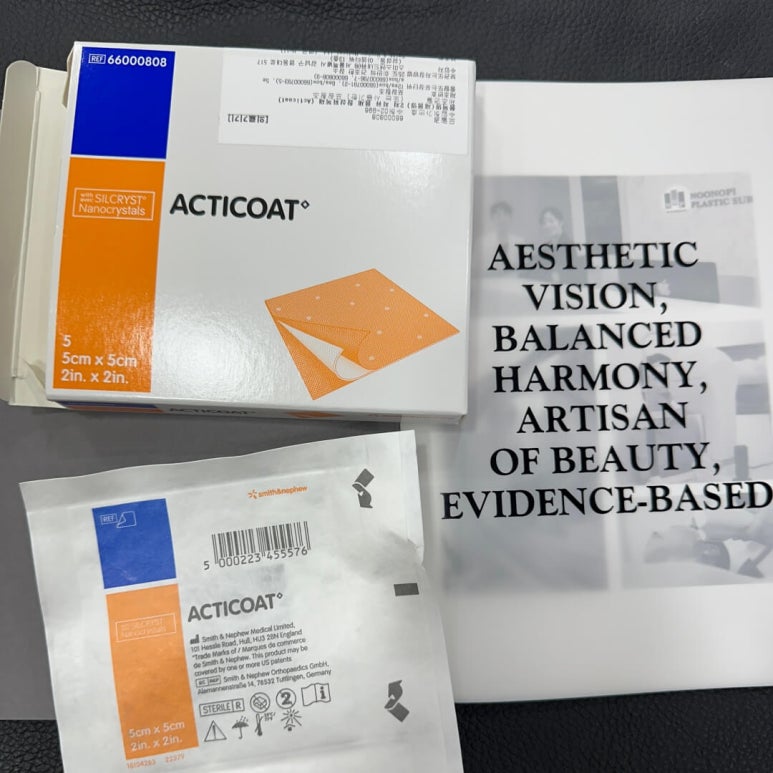
Acticoat
Acticoat, which contains silver, is mainly used in specialized hospitals.
https://youtu.be/ARJhv8tTIpw?si=-CrzlBpoXS4t0yPS
In fact, this material is extremely rarely used in ordinary households....
● pressure sores
● deep burns
● chronic wounds
● situations where infection is a concern
Unless it is one of these cases,
you can assume there is no need to use antimicrobial dressings.
- Conclusion
Wound care in English is called ‘wound dressing’ or simply ‘dressing,’
and when communicating with patients in the clinic,
I think the term dressing has become a fairly general word even for people who do not work in medical institutions.
However, there are many confusing material names,
and maintaining proper wound moisture is important,
but I often see cases where dressings are applied without sufficient understanding of that,
so I have organized the use of dressing supplies here.
For reference,
in cosmetic plastic surgery,
the real reason for applying ointment is not
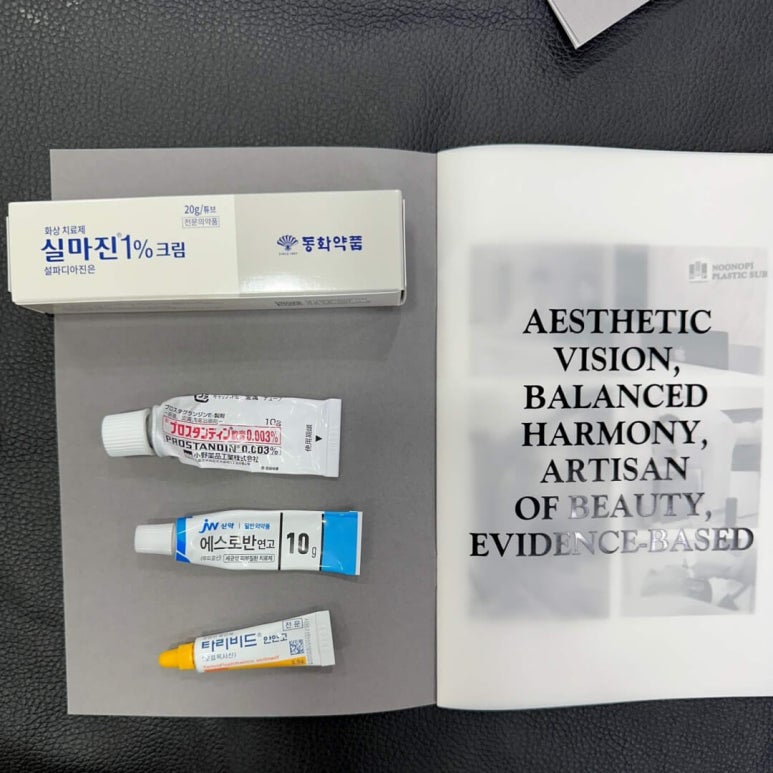
Ointments used for wounds
because the wound will fester if ointment is not applied
(planned cosmetic surgery falls under Class I Clean in the Surgical Wound Classification
— see the exam cheat sheet for Unit 4),
but rather
by applying ointment,
to create an appropriately moist wound environment.
Please keep in mind that moisture control in wounds
plays a very important role in the ideal healing process.
Was this helpful?
At Eye-Level Plastic Surgery, we operate a hyperbaric oxygen therapy unit
to support smooth wound healing.
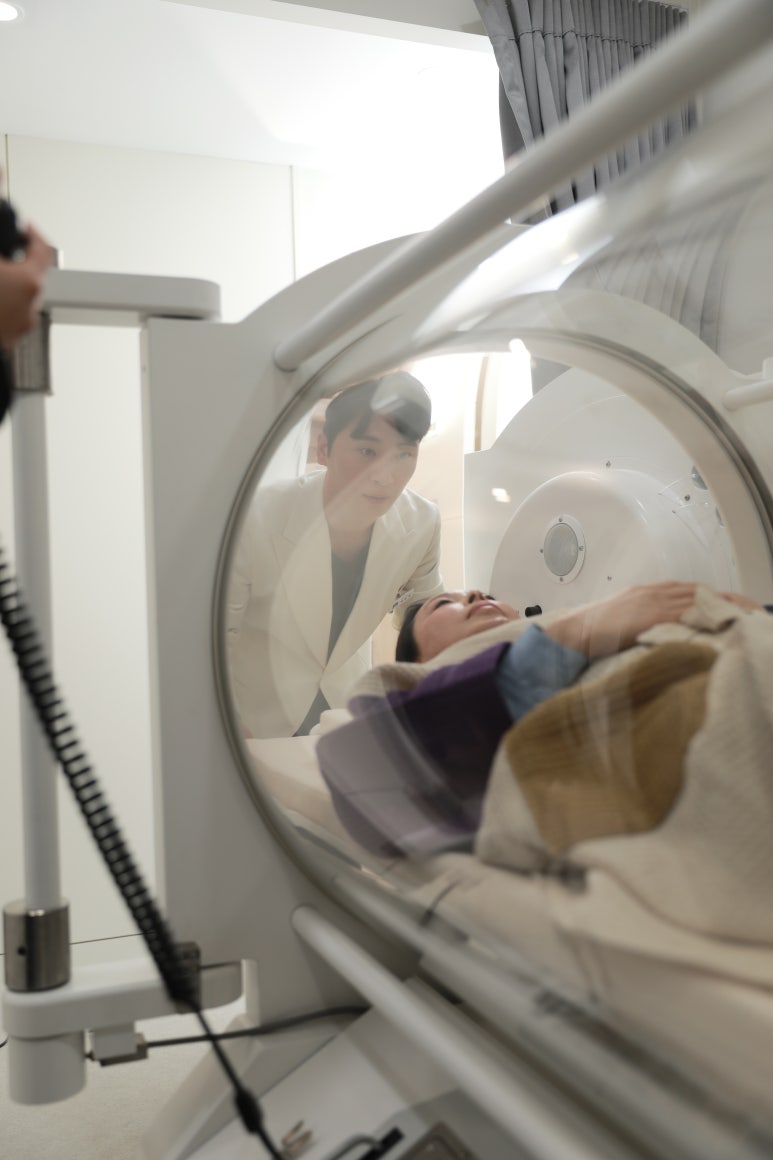
Previous image
Next image
Hyperbaric oxygen therapy
In addition to general cosmetic care,
we also provide reconstructive plastic surgery care such as scar treatment, burns, skin necrosis after fillers,
and inflammation after rhinoplasty, so I hope this was helpful^^

















