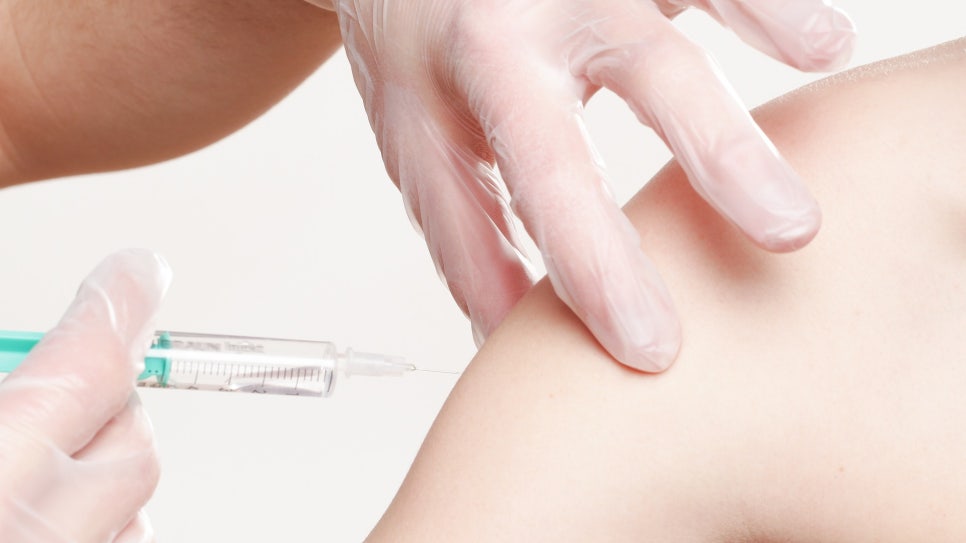
- Need for Treatment
Hyperhidrosis can occur at any age, but because it often develops during adulthood, when people are highly active in their occupations, it also affects job performance. In cases of severe palmar hyperhidrosis, door handles may feel slippery and uncomfortable to hold, and occupations that involve handling electrical equipment, metal, or textiles in particular tend to report greater discomfort. Professions that involve direct physical contact with others, such as doctors or physical therapists, are also affected by hyperhidrosis. In addition, hyperhidrosis can cause complications such as skin conditions like eczema or dermatitis in the areas where sweating is excessive, as well as infections such as athlete’s foot. Because hyperhidrosis can lead not only to psychological, social, and occupational problems but also to complications, it is a condition that requires proper diagnosis and effective treatment.
However, there is no clear clinical standard for how severe hyperhidrosis must be before treatment is needed. That said, if the patient feels that the sweating causes significant discomfort, treatment is considered necessary.
- Treatment
Various surgical and non-surgical methods are currently being used to treat hyperhidrosis. Since surgical methods carry a potential risk of complications, non-surgical treatment should be considered first before proceeding to surgery, and in fact many non-surgical treatments have been developed.
- Non-surgical treatment
(1) Topical agents
Topical agents used to treat hyperhidrosis include aluminum chloride, anticholinergic drugs, anesthetic drugs, and astringents. Because these drugs are safe, effective, and easy to apply, they are used as first-line medications for palmar and plantar hyperhidrosis and axillary hyperhidrosis.
(2) Oral medications
Many oral medications are useful in the treatment of hyperhidrosis, but their use is limited by excessive side effects. The most commonly used oral medications are anticholinergic drugs. Oral medications are used more often for generalized hyperhidrosis than topical agents, and typical examples include glycopyrrolate, oxybutynin, and propantheline. However, these drugs often cause complications such as blurred vision, sedative effects, hyperthermia, orthostatic hypotension, urinary retention, tachycardia, and palpitations, and because of these complications they are rarely used for localized hyperhidrosis. In particular, they must not be used in cases of myasthenia gravis, paralytic ileus, or pyloric stenosis, and should be used with caution in cases of angle-closure glaucoma, symptoms of bladder outlet obstruction, gastroesophageal reflux disease, or heart failure.
(3) Iontophoresis
Iontophoresis is also used for skin conditions such as scleroderma, lichen planus, ischemic ulcers, and wound infections, but it is also effective for hyperhidrosis, and is especially safe and effective for severe palmar and plantar hyperhidrosis. In iontophoresis, a direct electric current is applied while the skin is immersed in water in a basin.
(4) Botox
Botox is widely used for neuromuscular disorders such as strabismus, blepharospasm, and dystonia. Based on its proven safety and effectiveness, it is widely used as an intermediate treatment between non-surgical and surgical treatment for hyperhidrosis, especially axillary hyperhidrosis. Botox comes in types A through G, and the type used for hyperhidrosis is Botox A. Botox works by blocking the release of the neurotransmitter acetylcholine from cells.
- Surgical treatment
The sympathetic nervous system is a part of the autonomic nervous system and is responsible for innervating various secretory glands, including smooth muscle, cardiac muscle, and sweat glands. The sympathetic chain is a nerve structure that descends along both sides of the spine from the neck and thorax to the level of the second lumbar vertebra. Surgical treatment for hyperhidrosis refers to procedures performed on this thoracic sympathetic nerve within the thoracic cavity, and it has been carried out in various forms for about 100 years, from the past to the present.
In the early days, surgery was performed by making a large incision between the ribs to expose the thoracic sympathetic nerve, but with the development of thoracoscopic surgery, it became possible to treat the condition effectively in a minimally invasive way. The surgical method varies somewhat depending on the physician, and various techniques are used, such as cutting or severing the sympathetic nerve, cauterizing it, or clipping it. In addition, there are methods that cut only the branches arising from the sympathetic nerve without damaging the sympathetic trunk itself.
The location of the nerve to be operated on varies somewhat depending on the area of hyperhidrosis, and there are many different opinions regarding its effectiveness and side effects, so it remains controversial. In general, the more extensive the nerve surgery, the higher the risk of complications; however, if surgery is limited to a smaller area, such as resection of the sympathetic branches, the treatment may be ineffective or the chance of recurrence may increase.
Sympathetic nerve surgery rarely causes life-threatening complications. Possible postoperative complications include pneumothorax or pleural effusion due to air or fluid in the chest, bleeding, and nerve injury in the arm. When surgery is performed for facial hyperhidrosis, Horner syndrome, in which the eyelid droops, may rarely occur.
Although sympathetic nerve surgery for hyperhidrosis is permanently effective and safe, it remains controversial because of its side effects. Among these side effects, compensatory hyperhidrosis is the most common after hyperhidrosis surgery and is the main reason patients regret undergoing the procedure.
It is no exaggeration to say that most studies on hyperhidrosis focus on this compensatory hyperhidrosis. After sympathetic nerve surgery, sweating that had occurred in the hands, armpits, or face shifts to the trunk, thighs, or lower body; this is called compensatory hyperhidrosis. Symptoms vary from patient to patient, so the affected areas differ and the degree of discomfort also differs. However, there is no way to predict the extent of compensatory hyperhidrosis before surgery, and it is known that discomfort increases as more areas of the nerve are operated on.
Various methods have been attempted to treat compensatory hyperhidrosis, but no established method exists yet, so even if a patient regrets surgery afterward, there is no way to reverse it. Reported incidence also varies considerably among researchers, with mild compensatory hyperhidrosis reported at about 14–90% and severe cases at about 1–30%. Because compensatory hyperhidrosis can cause extreme distress in some patients, the patient must be fully aware of the possibility of this side effect before deciding to undergo surgery.
So far, I have explained the treatment of hyperhidrosis.
In the next installment, we will learn about acute myocardial infarction.
Source: Korea Disease Control and Prevention Agency National Health Information Portal
