Hello,
I am Director Yeo Sang-ho of Songjeong Station Dental Clinic.
The condition in which the space between teeth widens,
interdental spacing,
is often regarded simply as
a cosmetic issue.
However, when this symptom
appears together with periodontal disease,
it becomes a complex problem that can have
serious effects on overall oral health.
That said, this can occur
for various reasons.
It may happen when there is a congenital imbalance
between the size of the jawbone
and the size of the teeth,
or when teeth are congenitally missing.
What should be examined carefully, however,
is interdental spacing caused by periodontal disease.
As periodontal disease progresses,
inflammation develops in the gums
and alveolar bone surrounding the teeth.
The toxins released from plaque
and calculus formed by bacteria
continuously irritate the gum tissue,
and over time, what begins as simple gum inflammation
can destroy the periodontal ligament
and even the alveolar bone.
At this point, as the alveolar bone is resorbed
and weakened,
the function that firmly supported the teeth
decreases significantly.

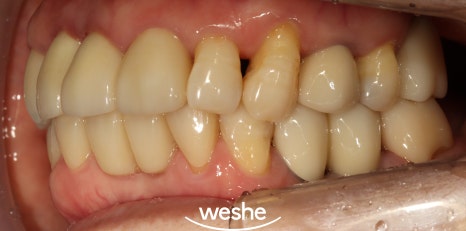
Songjeong Station Dental Clinic treatment period: 2023.05.12~2024.02.14
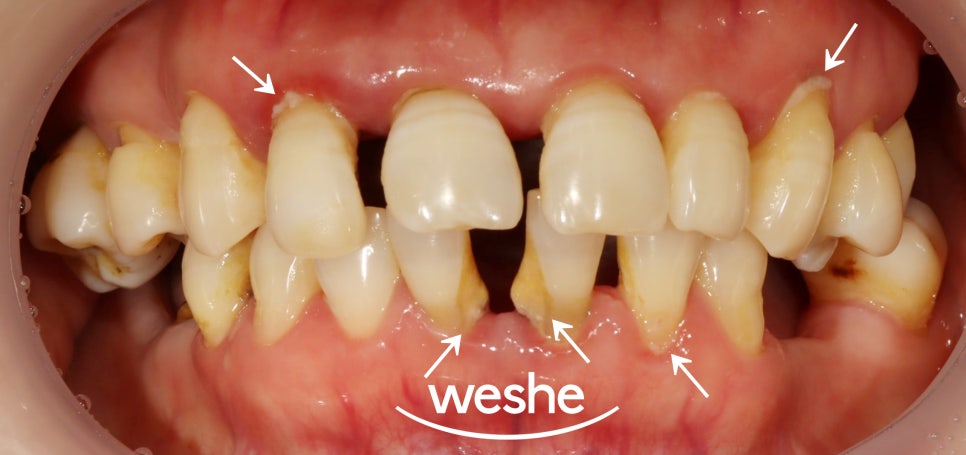
In particular, the front teeth area
shows these changes more prominently
because of the way chewing forces are concentrated there.
Teeth being pushed forward or spreading out in a fan shape
are typical examples,
and in such cases,
simple periodontal treatment alone is often insufficient
to solve the problem fundamentally.
When interdental spacing and periodontal disease
occur at the same time,
systematic examinations are necessary
for an accurate diagnosis.
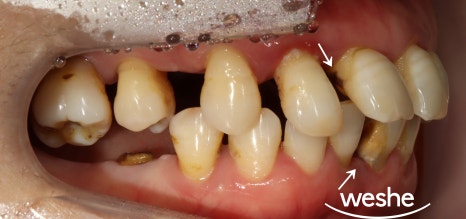
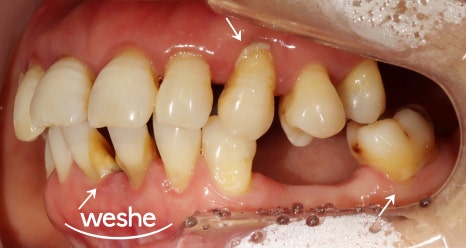
After first evaluating the degree of visible spacing
between the teeth and the condition of gum inflammation,
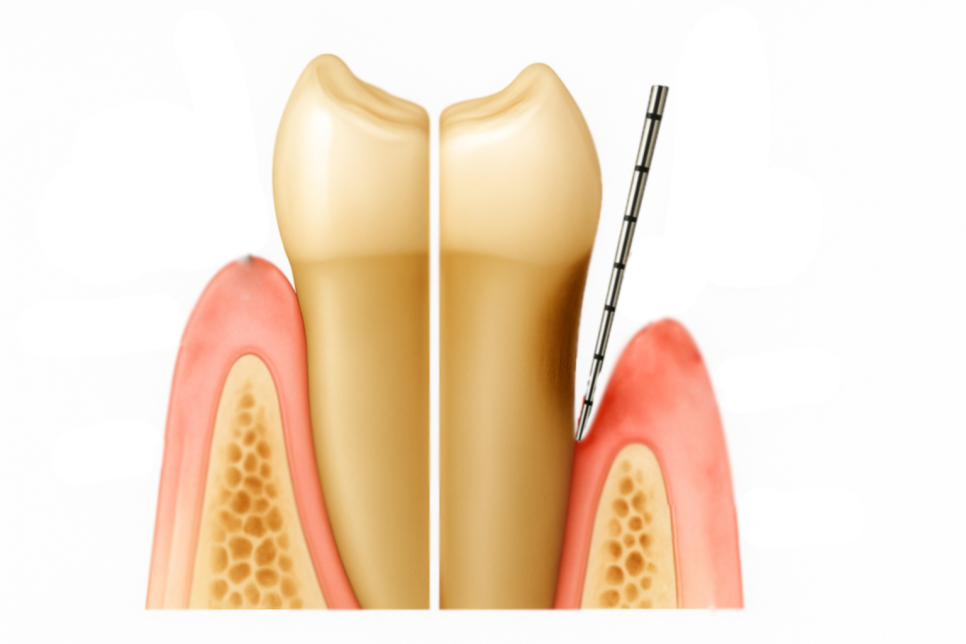
a test is performed to measure the depth of the periodontal pockets.
The normal depth of a periodontal pocket is about 2-3 mm,
but when periodontal disease progresses,
it becomes deeper than 4 mm.
In severe cases, it can deepen to 6-7 mm,
and these figures are important indicators
for objectively assessing the extent of periodontal disease progression.
In addition, tooth mobility is evaluated
through a test to see how much the tooth moves.
It is classified by stage,
and a natural tooth showing severe mobility
is judged to be in a condition that is difficult to preserve.
At this point, changes in the position of the natural tooth
and functional problems must also be considered.
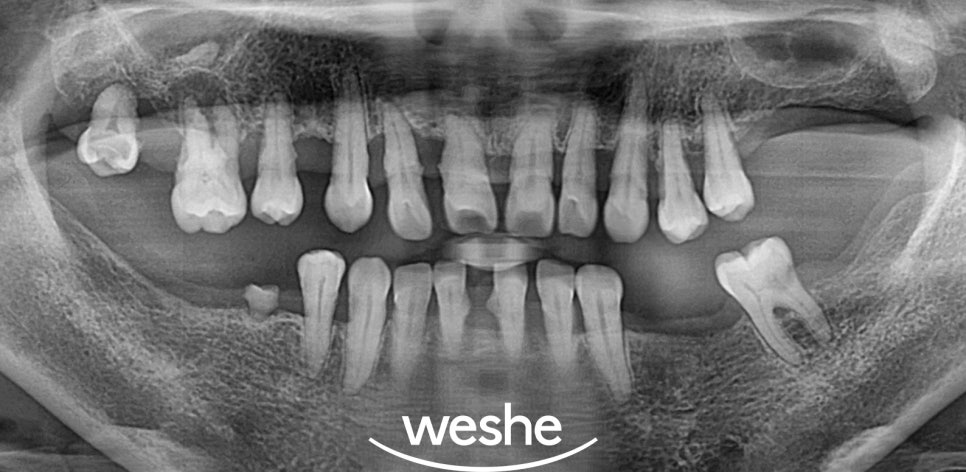
Through radiographic imaging,
the degree of alveolar bone resorption
and the condition around the tooth root
are analyzed in detail.
If alveolar bone resorption has progressed
to more than two-thirds of the root length,
or if the alveolar bone around the tooth
has been extensively destroyed,
the long-term prognosis for that area
is evaluated as poor.
In such a state,
it can become a source of persistent inflammation
and negatively affect adjacent healthy teeth as well.
When interdental spacing and advanced periodontal disease
appear at the same time,
careful treatment planning requires
comprehensive consideration of multiple factors.
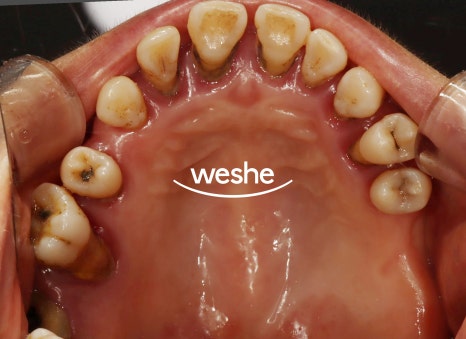
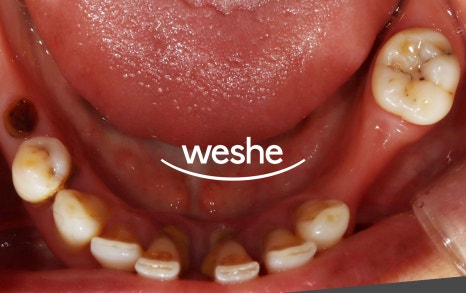
The first thing considered is
the possibility of preserving the affected tooth.
When alveolar bone resorption is severe
and tooth mobility reaches grade 3,
it is difficult to expect long-term success
with conservative treatment.
There are several reasons why implant treatment
is considered in this situation.
First, leaving a tooth in place when it cannot be preserved
can make it a source of ongoing inflammation
and damage the surrounding teeth and jawbone.
Second, after extracting a tooth,
if the space is left as is,
the adjacent teeth may move into the empty space,
worsening the overall dental alignment.
For these reasons, at Songjeong Station Dental Clinic,
we believe it is necessary to quickly resolve the problem
by distinguishing between areas that can be preserved
and those that cannot.
Implant treatment in cases accompanied by
periodontal disease and interdental spacing
is carried out in stages.
First, periodontal treatment is performed
to control acute inflammation.
Calculus is removed through scaling,
and if necessary, root planing is performed
to remove calculus and inflammation from the root surface.
Extraction of teeth that cannot be preserved
must be planned carefully.
During the extraction process,
damage to surrounding tissue is minimized,
and for future implant placement,
in some cases bone grafting is performed at the same time as extraction
to secure sufficient bone volume for implant placement.
Before implant placement,
gum inflammation must be controlled.
If an implant is placed while inflammation is present,
the risk of complications such as failure of osseointegration
or peri-implantitis increases.
Therefore, after allowing sufficient healing time
and once the gum condition has stabilized,
the implant is placed.
The osseointegration process, in which the fixture
firmly bonds with the jawbone,
generally takes 3-6 months.
During this period, regular checkups
are used to monitor the healing process,
and if necessary,
a temporary prosthesis is made
to maintain function and aesthetics.
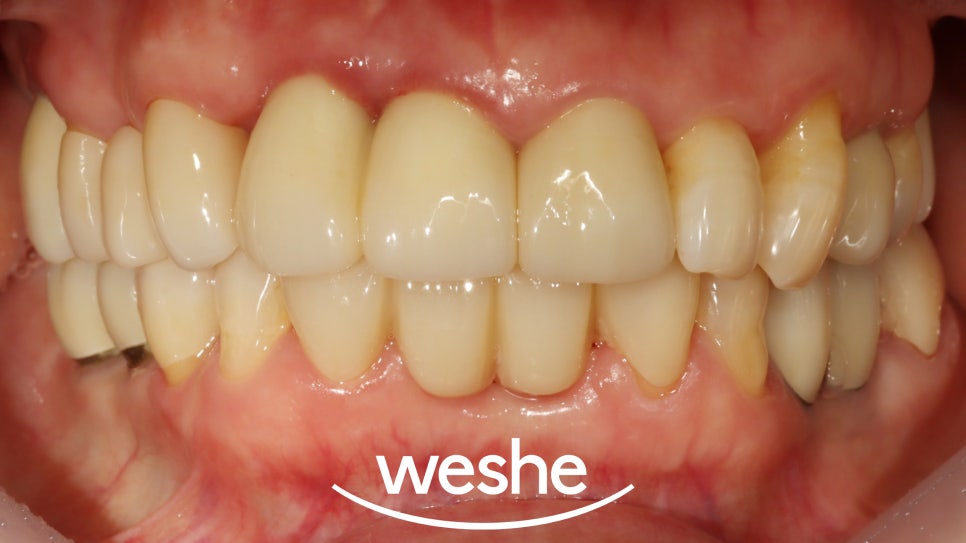
After osseointegration is complete,
a final prosthesis is made
to restore the natural tooth shape
and function.
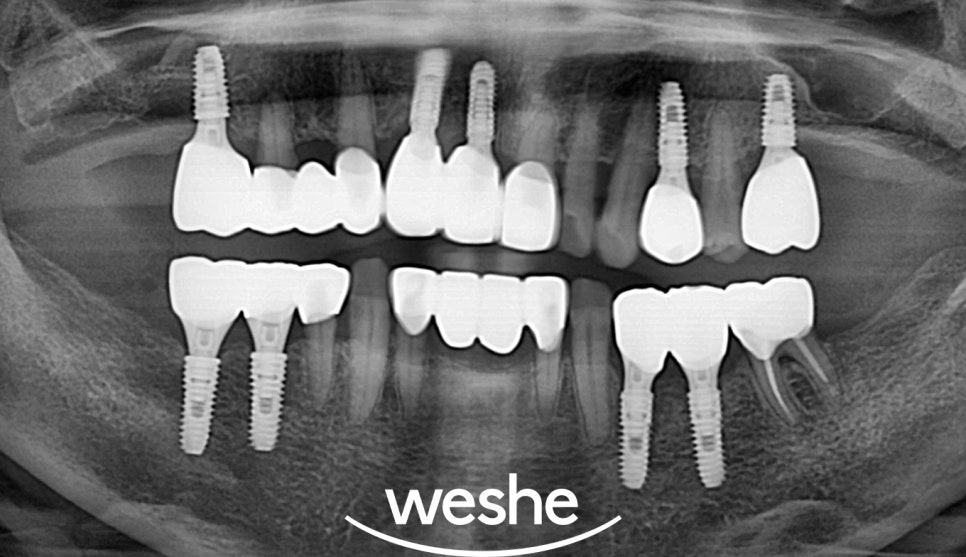
Implants themselves do not develop cavities,
but the surrounding gums and bone
are still vulnerable to bacterial infection.
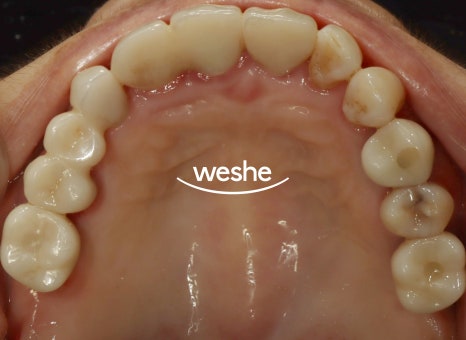
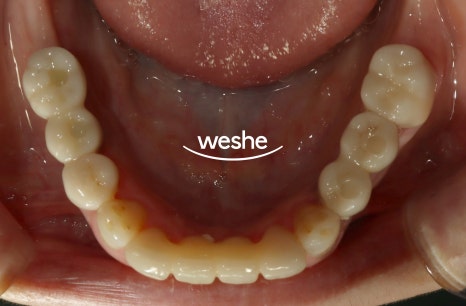
If peri-implantitis develops,
it can progress even faster than periodontal disease in natural teeth,
so special caution is required.
For daily oral care,
it is effective to use auxiliary tools such as
interdental brushes or a water flosser along with a regular toothbrush.
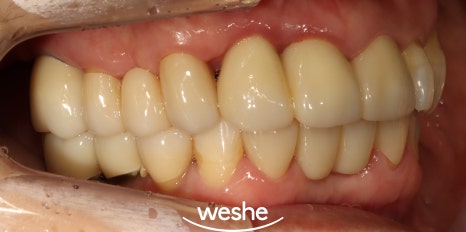
In particular, maintaining cleanliness between implants and natural teeth,
as well as along the gum line,
is important.
You should receive instruction on proper toothbrushing methods
and interdental cleaning techniques,
and continue to practice them consistently.
In conclusion, when interdental spacing
and periodontal disease occur at the same time,
it is important to address the underlying cause
rather than simply relieving the symptoms.
Implant treatment is one way to comprehensively
resolve these complex issues,
but to improve the success rate of treatment,
accurate diagnosis, systematic planning,
and ongoing management must be in place.
This has been Yeo Sang-ho, Director of Songjeong Station Dental Clinic.













