- Why Do Dentists Keep Asking to Take X-rays?
Hello, this is Yeo Sang-ho from Yonsei Wish Dental Clinic.
While treating patients, I often get questions like this.
(This is a panoramic photo of our front desk staff member, haha.)
Do we really need to take pictures if nothing hurts?
"I don’t have any pain or discomfort right now,
so do I really need to get an X-ray?"
The thing is, teeth are not a structure you can fully see inside.
So even when nothing looks wrong to the naked eye,
there are many times when an X-ray reveals something unexpected.
In particular, root infections, cavities that are not visible on the surface,
and changes in the jawbone around the gums
cannot be identified by sight alone.
Of course, if you recently had X-rays taken at another clinic
and received a thorough explanation of your current condition,
there is no need to take them again.
But if that is not the case,
I recommend checking once more.
Even if it feels a little inconvenient, from the patient’s perspective
it can lead to faster and more accurate diagnosis.
Something may look fine for now,
but checking in advance before a bigger problem develops later
may be the better choice.
As I always feel,
when it comes to treatment,
what matters more than starting quickly
is starting after making the right judgment. 😊
Case 1. Came in for scaling, but an unexpected finding…
Not long ago, a patient came in for scaling.
There were no particular symptoms,
but the patient mentioned that it had been a long time since their last checkup and X-ray,
so we decided to take a simple exam along with an X-ray.
(We proceeded after giving a full explanation and obtaining consent!)
Below is the patient’s intraoral photo.
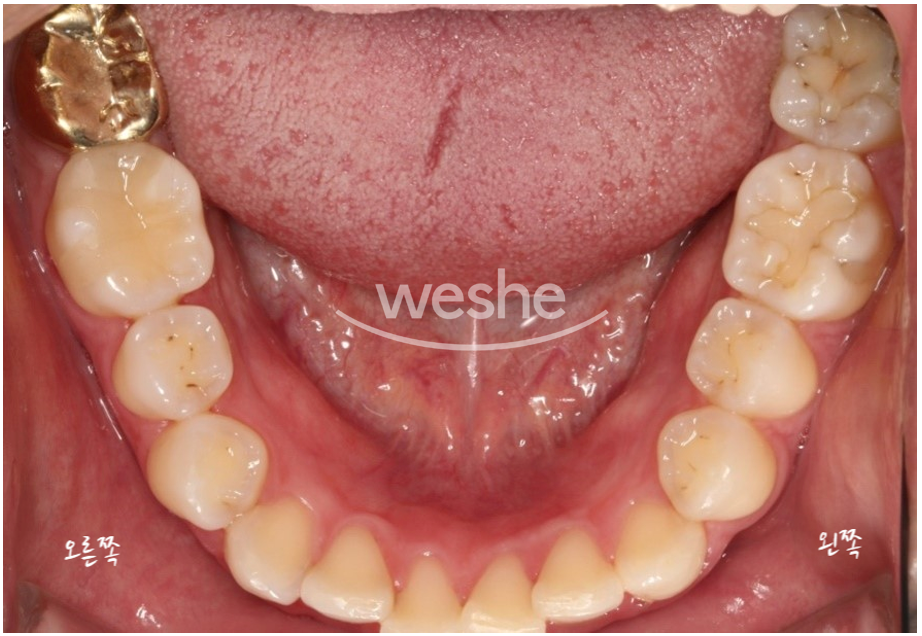
In the right lower molar area (left side in the photo),
there is a restored area treated with a metal crown,
and two lower left molars show sites where cavities were treated in the past.
On the surface, there did not seem to be any major problem,
but the X-ray revealed something unexpected.
Below is the patient’s panoramic X-ray.
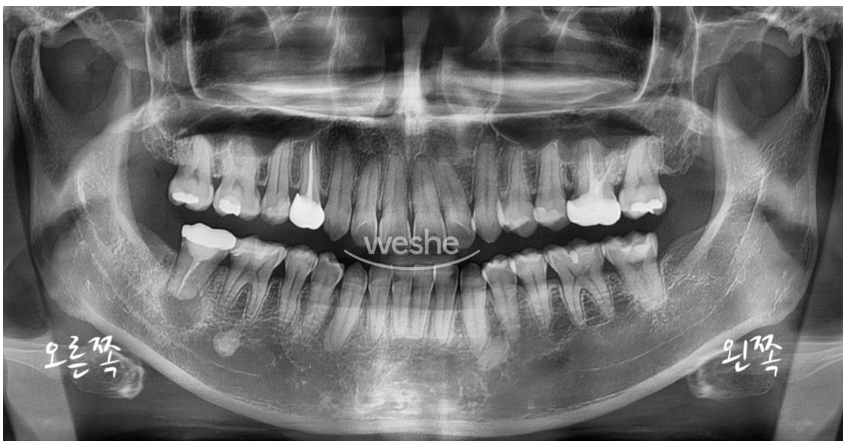
An unexpected problem was found. What could it be?
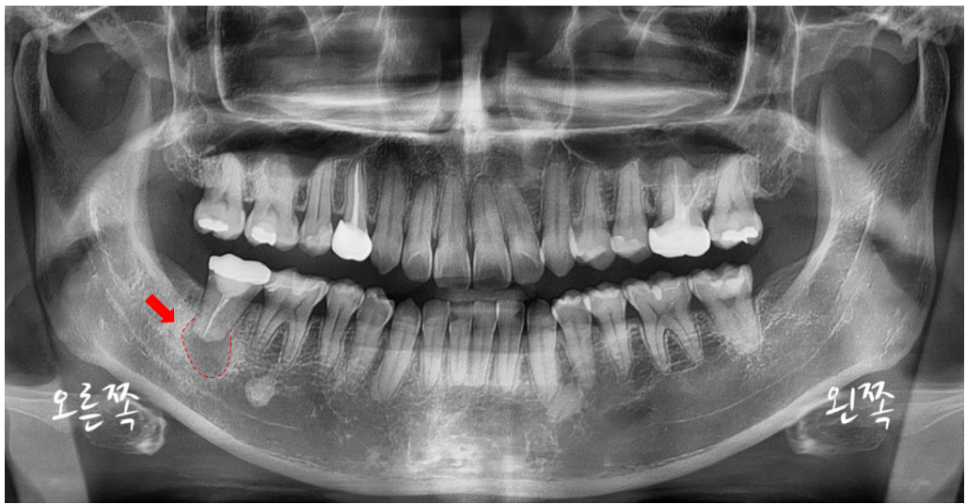
A dark shadow is seen in the marked area.
Normally, healthy alveolar bone (jawbone around the gums) appears as a white or grayish trabecular pattern on X-rays,
but a dark, hollow-looking shadow like this
may indicate that the bone tissue has weakened or been resorbed due to inflammation or other causes.
Because the area was fairly large,
we decided to take a CT scan for a more precise diagnosis.
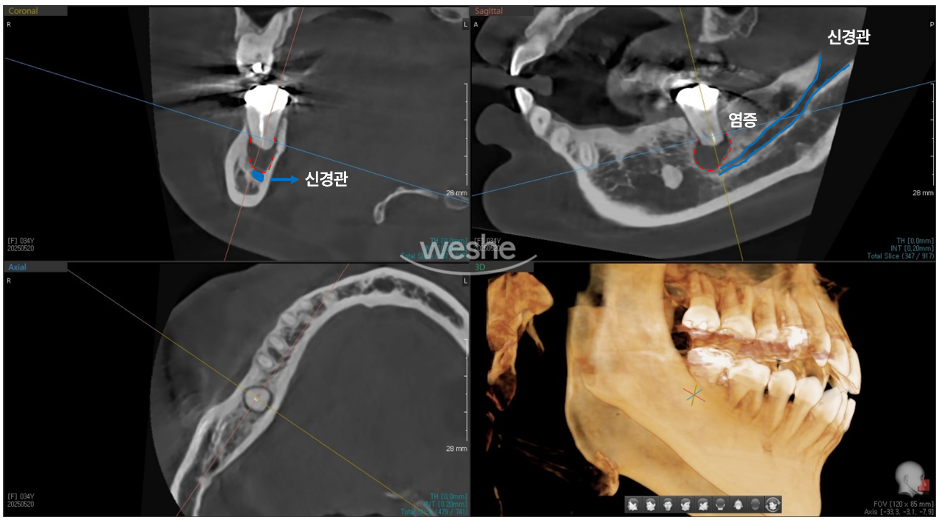
This is the CT image of the same area.
The area marked in red on the X-ray shown below is the dark shadow seen in the panoramic X-ray above.
It is a space created as the alveolar bone was dissolved by inflammation.
The area marked in blue is what we commonly call the inferior alveolar nerve (IAN).
This nerve is an important structure responsible for sensation in the lower jaw,
and it is usually safely protected inside hard bone.
However, when inflammation becomes severe,
it can directly compress the nerve,
or even dissolve the bone surrounding it.
In such cases, numbness that feels as if anesthesia is not wearing off,
or altered sensation, may occur.
For this patient, considering the possibility of saving the tooth,
we decided to proceed with intentional replantation.
(I’ll introduce this treatment in more detail next time if I get the chance!)
Without taking an X-ray, this was a situation where a problem that would have been difficult to identify by sight alone could have been missed.
Even if there is no discomfort,
regular X-ray examinations are very helpful in checking the condition of the teeth and gums
and preventing major treatment later on.
Case 2. A broken tooth from a fall, and another problem confirmed by CT
A male patient came in saying that two weeks earlier,
he had fallen and broken a tooth.
Wanting to save the tooth as much as possible, he looked into several clinics,
and came after being introduced by an acquaintance to a clinic where a specialist in conservative dentistry was practicing.
(The person who referred him—could that have been you? Thank you. T^T)
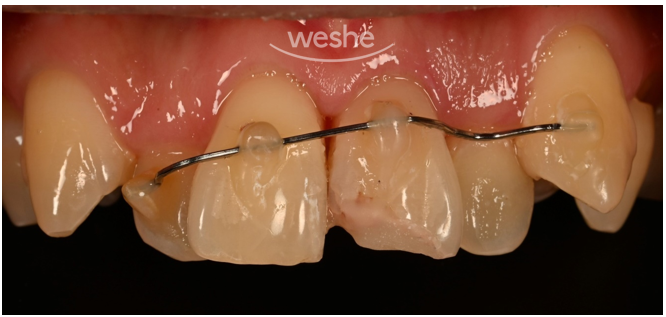
The photo above shows the inside of the patient’s mouth.
The upper left front tooth area (right side in the photo) is visibly broken.
According to the patient,
when he visited a dental clinic right after the injury,
the doctor provided excellent emergency care.
The tooth had been pushed into the gum when it broke,
and the doctor repositioned it correctly,
then also stabilized it with wire because it was loose.
It was a moment when emergency response was absolutely crucial,
and thanks to the quick judgment and treatment by the first doctor,
the prognosis for the tooth may have improved significantly.
However, based on appearance alone or even with a panoramic X-ray,
it can sometimes be difficult to determine whether there is a problem with the root area of the tooth.
For a more accurate assessment,
after explaining the situation to the patient, we decided to take a CT scan.
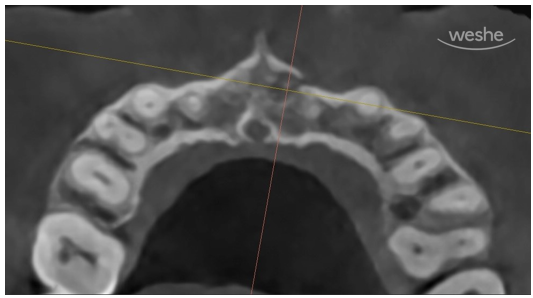
This is the CT image.
The direction is as if we are looking down from above the patient’s head.
What do you see?
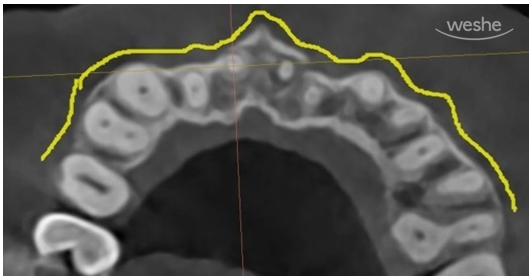
The yellow line was drawn along the outer boundary of our alveolar bone.
On the X-ray, it appears as a dark white line.
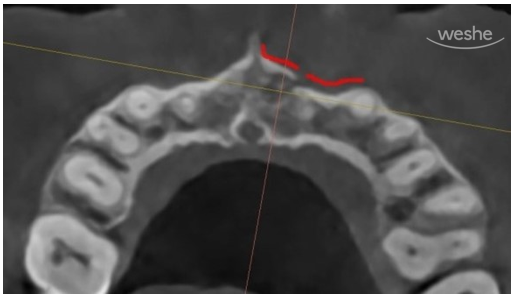
In other areas, the alveolar bone is continuous and well maintained,
but in the red-marked area, the bony outline is clearly interrupted.
This means that it was not simply the tooth that moved;
there was also a fracture in the jawbone itself due to trauma.
According to the guidelines of the American Association of Endodontists (AAE),
if a tooth has been displaced inward into the gum due to trauma,
wiring it in place for about 2 weeks is sufficient.
However, when a fracture of the alveolar bone is also present as in this case,
a fixation period of at least 4 weeks is recommended.
In other words, not all trauma cases are treated the same way.
That is because the treatment plan, fixation period,
and even the order of treatment can all differ depending on the condition.
This case was the same.
If we had not taken the CT scan, we might have checked only the tooth position
and missed the fracture in the alveolar bone.
In that case, the recovery period could have been affected,
and the prognosis might have changed.
Thanks to the patient carefully deciding to undergo the exam and imaging,
we were able to make a more accurate diagnosis
and establish a treatment plan suited to the situation.
Thank you sincerely for your cooperation :)
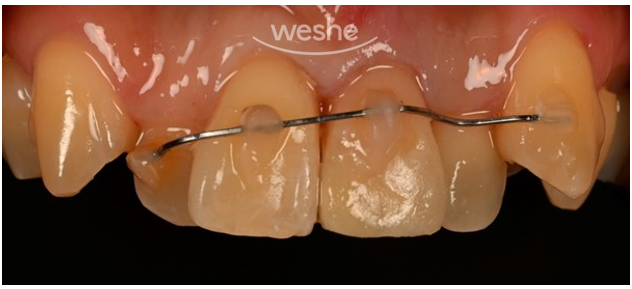
The patient said that in social situations, when speaking or smiling,
he felt uncomfortable worrying that the broken area of the tooth might be visible.
So, to reduce cosmetic discomfort in the pre-treatment stage,
we provided temporary reinforcement treatment.
Case 3. What the thought of “It’ll probably be fine” misses
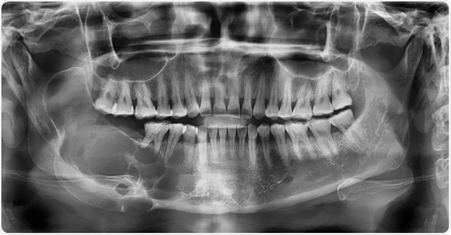
Image Credit: Rames Khusakul/Shutterstock.com - This is a photo of another patient found on Google
The image above is an X-ray of a patient diagnosed with ameloblastoma.
Do you see the dark shadow spreading like soap bubbles in the lower left (lower right from the patient’s perspective)?
Ameloblastoma is a tumor that occurs in the jawbone.
Although it is classified as a benign tumor,
it is characterized by very destructive behavior and tends to dissolve bone.
Benign tumors that develop in other parts of the body
can usually be removed well with surgery without causing major problems.
But ameloblastoma is not simply solved by removal.
It can recur,
and the biggest issue is that because it is a tumor in the jawbone,
part of the jawbone has to be removed,
and then reconstruction is needed so the patient can chew and speak again
without causing aesthetic problems.
It is a very large and difficult surgery.
Even after the surgery was completed safely,
I still remember a young female student quietly crying while looking in the mirror.
Although the tumor had been removed successfully,
accepting the changed appearance after jaw reconstruction
must have been far from easy.
Of course, in the end, the treatment was completed successfully.
But part of me still thought,
“If it had been found a little earlier...
the extent of the surgery might have been smaller.”
A panoramic X-ray taken about once a year
does not cost as much as people might think.
Usually, it is about the price of one chicken order. :)
If this small check can help us protect the health of our face, jaw, and teeth
for a little longer and a little more comfortably,
wouldn’t it be worth taking the time once in a while?
While thinking, “There’s nothing really hurting...”
we may pass over problems that could have been quietly growing.
If it can prevent a bigger problem in advance
for the price of one order of chicken,
wouldn’t that be a more economical choice?










