At Kkachisan Implant Dental Clinic, we will explain the relationship between osteoporosis medication and implant surgery.
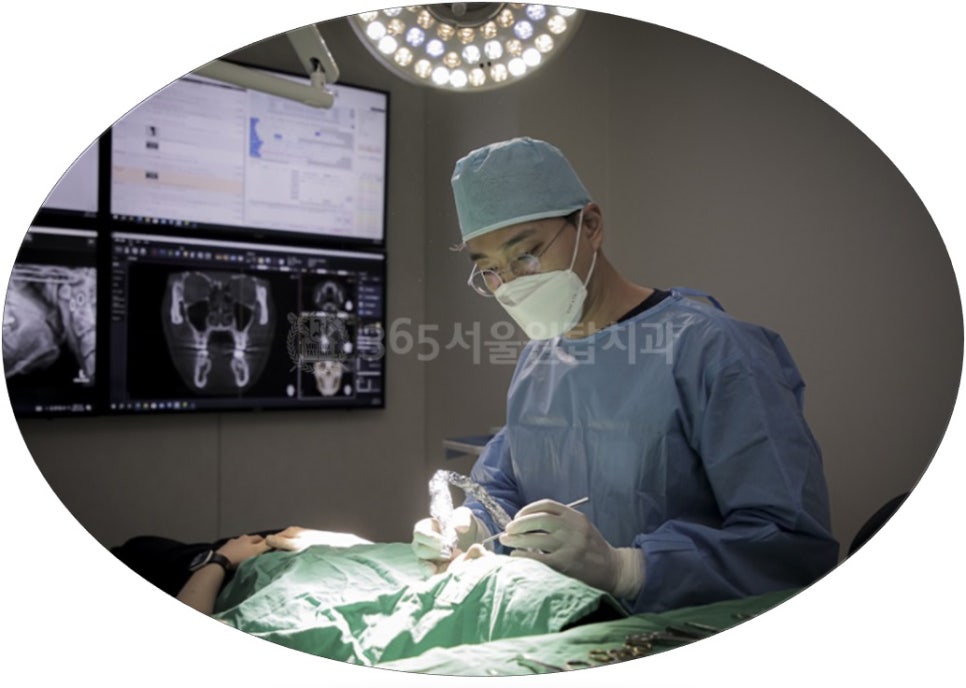
Dr. Kim Geun-il, Director of 365 Seoul One Top Dental Clinic
Hello.
I am dentist Kim Geun-il.
Recently, during an implant consultation with a patient living in Kkachisan,
there was a female patient who said she had been dealing with osteoporosis for a long time and was worried about implant surgery.
Are there any of you who are 고민 중이신 분들이 계신가요? before an implant consultation because you are receiving osteoporosis injections or taking medication?
After the age of 40, bone density
begins to gradually decline,
and especially in women over 50 after menopause,
diagnoses of osteoporosis and medication use
increase sharply.
In fact, in our Gangseo-gu area as well,
people of various ages, from young to old,
are living here,
and especially when consulting with patients over 50 about implants,

I’m taking osteoporosis medication.
Is implant surgery okay?
We hear this question often.
To give the conclusion first,
in most cases treatment is possible,
but an accurate evaluation of the duration of use and overall health condition
is absolutely necessary.
Why is osteoporosis medication a problem?
At Kkachisan Implant Dental Clinic, we will talk in detail about the problems that can occur during treatment surgery when osteoporosis medication is involved.
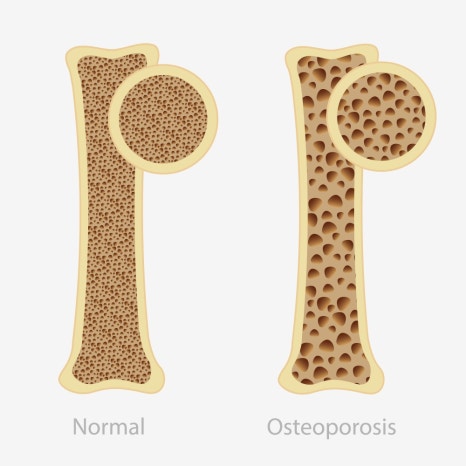
If you have been taking osteoporosis medication for a long time, there is a possibility of jawbone necrosis during tooth extraction or implant surgery, but it does not occur in everyone.
Common osteoporosis treatments
such as bisphosphonates and antiresorptives like denosumab
reduce the activity of osteoclasts that break down bone,
suppress the bone remodeling process,
and help maintain bone density.
The problem is that this effect can also
appear in the jawbone.
After surgical treatment,
the healing process of the bone may be delayed,
and in rare cases, medication-related jawbone necrosis (BRONJ)
may occur.
In dental surgical procedures such as
implants or extractions,
the jawbone (alveolar bone) is often directly exposed,
and normally, through the resorption process by osteoclasts,
osteoblasts are stimulated, new bone is created in that area, and it heals,
while the implant’s artificial root
undergoes a process of fusing with the surrounding bone.
However, if osteoporosis medication has been taken for a long time,
because it reduces osteoclast activity,
new bone formation also slows down,
and symptoms of osteomyelitis may occur, where healing does not proceed and the jawbone remains exposed.
However, not every patient using bisphosphonate preparations
will develop BRONJ (jawbone necrosis).
The likelihood of occurrence varies depending on
the duration and type of the medication,
and whether medications such as steroids
were taken together.
Among patients taking osteoporosis medication,
the rate at which jawbone necrosis occurs
is currently known to be relatively low,
but because it is highly related to osteoporosis medication,
I think it needs to be examined carefully.
What is the 기준 for the duration of osteoporosis medication before implant surgery?
At the time of Kkachisan implant surgery, the duration of osteoporosis medication is usually monitored carefully when it has been taken for about 3 to 5 years.
In clinical practice, there are cases where 3 years or 5 years
is used as the 기준.
This is less a matter of different concepts
and more a difference in the approach to assessing risk.
Currently, many international guidelines
mention a possible increase in risk when oral bisphosphonates have been taken for 4 to 5 years or more.
*If taken for 4 to 5 years or more, or
if risk factors such as diabetes or concurrent steroid use are present
→ a more cautious approach, and if necessary, consideration of consultation with the primary physician
Some medical institutions
apply a 3-year 기준, but
this should be understood as a more conservative safety standard.
What matters most is not a simple number of ‘how many years,’
but a comprehensive judgment based on the duration of use, systemic disease, and type of medication.
 At Kkachisan Implant Dental Clinic, we do not arbitrarily tell patients to stop medication during implant surgery.
At Kkachisan Implant Dental Clinic, we do not arbitrarily tell patients to stop medication during implant surgery.
Should you stop taking osteoporosis medication before implant surgery?
At Kkachisan Implant Dental Clinic, whether to stop medication before implant surgery is determined only through an opinion letter from the primary physician.
If necessary for implant surgery,
the osteoporosis medication being taken may need to be stopped,
but it is not recommended for the patient to stop the medication on their own without an opinion letter from the primary physician.
(※This is a very dangerous act)
In particular, with denosumab,
sudden discontinuation can increase the risk of fractures.
If necessary, after consultation with the prescribing physician,
a drug holiday is carefully decided.
It is not applied uniformly to all patients.
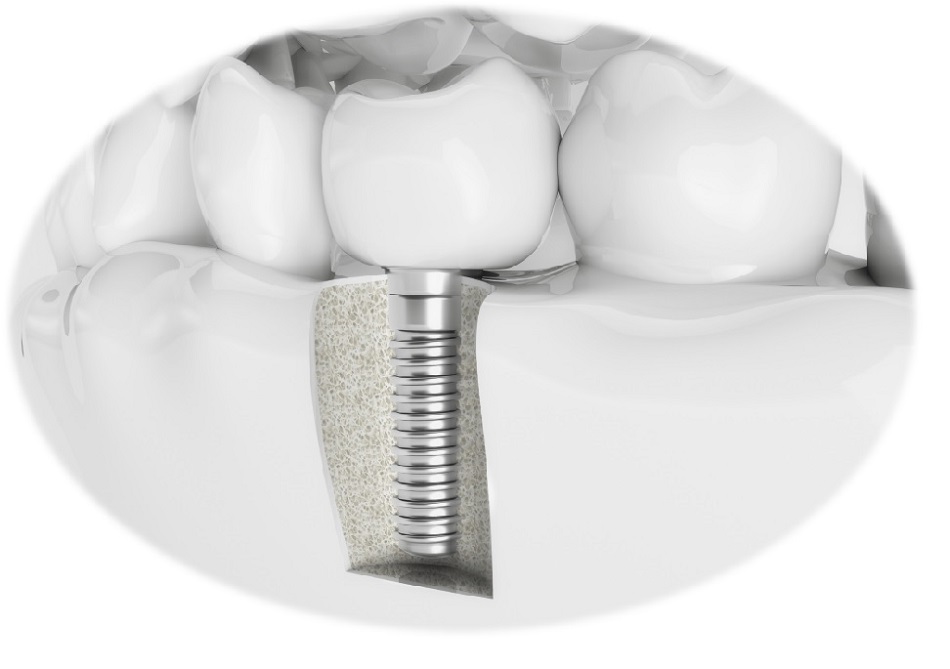 If accurate diagnosis and thorough infection control are carried out, the implant success rate in patients with osteoporosis does not differ greatly from that of general implant patients.
If accurate diagnosis and thorough infection control are carried out, the implant success rate in patients with osteoporosis does not differ greatly from that of general implant patients.
What is the implant success rate in patients with osteoporosis?
At Kkachisan Implant Dental Clinic, with sufficient healing time and proper infection control, patients with osteoporosis can also undergo implant treatment safely and successfully.
According to studies,
the implant success rate in patients taking oral bisphosphonates
often does not differ greatly
from that of general patients.
However,
-
minimally invasive surgery
-
thorough infection control
-
securing sufficient healing time
-
regular follow-up monitoring
are even more important.
 Kkachisan implant treatment: do not give up hastily because of osteoporosis; first visit the dental clinic and accurately check your current condition.
Kkachisan implant treatment: do not give up hastily because of osteoporosis; first visit the dental clinic and accurately check your current condition.
Do not give up on implant surgery hastily
Even patients with osteoporosis can establish a safe treatment plan for implants at Kkachisan Implant Dental Clinic if safety is confirmed through systematic examination.
Just because you are taking osteoporosis medication
does not mean you must
give up on implants.
After carefully reviewing safety through
an accurate medical history check and
bone condition assessment based on 3D CT,
planning treatment is the key.
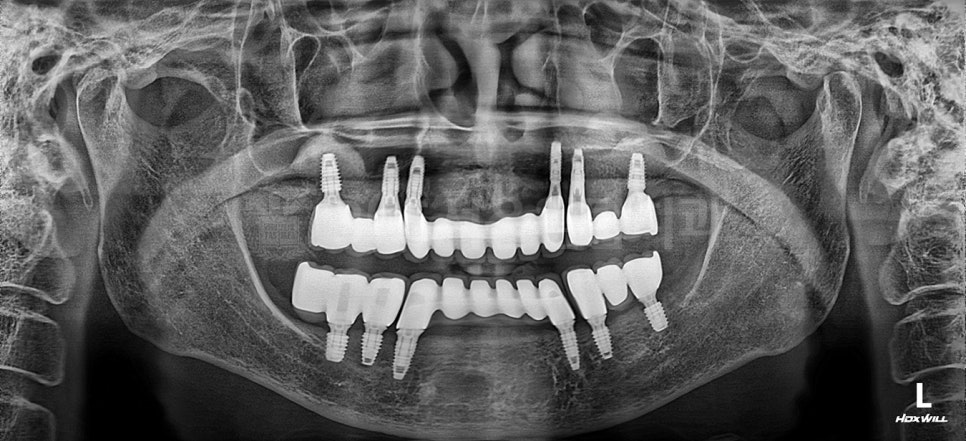
This is sample material for explanation purposes.
In fact, a woman in her mid-70s who recently visited us
had been taking osteoporosis medication for a long time,
but at our hospital
she underwent full-mouth implant treatment
and is currently using them comfortably without any inconvenience
while continuing regular checkups.
Even at an advanced age,
even after taking osteoporosis medication for a long time,
there are cases where implants are possible.
As a dentist,
I understand very well the sadness of patients caused by tooth loss.
Therefore, rather than giving up unconditionally,
after accurately understanding each patient’s systemic diseases,
I provide implant treatment that also considers overall health.
Rather than vague worry,
please confirm the possibility through an accurate diagnosis.
This was dentist Kim Geun-il.
Thank you.

This post was written by the representative director
based on Article 56, Paragraph 1 of the Medical Service Act
for the purpose of providing medical information to patients.
-Notice of side effects: After treatment, side effects such as infection, inflammation, bleeding,
sensory changes, and soft tissue complications may occur.
-Depending on the individual’s health condition, dental treatment may cause different side effects,
so please be sure to consult with medical staff before making a decision.
📍 365 Seoul One Top Dental Clinic
4F, Dongmyeong M Building, 179 Gangseo-ro, Gangseo-gu, Seoul
Implant dental clinic in Hwagok-dong, Gangseo-gu
1 minute on foot from Exit 8 of Hwagok Station





 At Kkachisan Implant Dental Clinic, we do not arbitrarily tell patients to stop medication during implant surgery.
At Kkachisan Implant Dental Clinic, we do not arbitrarily tell patients to stop medication during implant surgery. If accurate diagnosis and thorough infection control are carried out, the implant success rate in patients with osteoporosis does not differ greatly from that of general implant patients.
If accurate diagnosis and thorough infection control are carried out, the implant success rate in patients with osteoporosis does not differ greatly from that of general implant patients. Kkachisan implant treatment: do not give up hastily because of osteoporosis; first visit the dental clinic and accurately check your current condition.
Kkachisan implant treatment: do not give up hastily because of osteoporosis; first visit the dental clinic and accurately check your current condition.

