On June 11, Minish Dental Hospital held a somewhat special seminar along with its regular directors’ meeting. In this seminar, led directly by Director Yoon Pil-sang, the focus was on facial changes caused by severe tooth wear and a case in which ‘Minish Full Mouth’ was applied to restore them.
Director Yoon emphasized that diagnosis should move beyond simply looking at the condition of the teeth and should also analyze the balance of the entire face and the pattern of change. In particular, he explained that vertical dimension (VD), the distance between the upper and lower jaws, is the key standard for treatment planning and must be checked when considering both esthetic and functional recovery, since it affects not only function but also the overall impression.

Director Yoon Pil-sang, Minish Dental Hospital
When teeth are worn down significantly, the problem is not just appearance. As the height between the upper and lower jaws, that is, the vertical dimension, decreases, the entire face can appear to sag, and the ability to chew food properly also gradually declines. This can also reduce the retention of prosthetic restorations. Therefore, when a full prosthetic restoration is needed, deciding whether to maintain the current facial height or restore the reduced vertical dimension becomes the starting point of treatment.
While explaining this treatment design, Director Yoon introduced three representative approaches used in the treatment of patients with tooth wear. This classification is based on a paper by Turner.
First, a method that restores the reduced facial height
Second, a method that creates prosthetic space while maintaining the current height
Third, after comprehensively analyzing the patient’s chewing condition and facial balance
A strategy that sets the treatment scope while making only minimal changes in height. Rather than any one of these being the single “correct” answer, they should be applied flexibly according to the patient’s oral structure and occlusion.
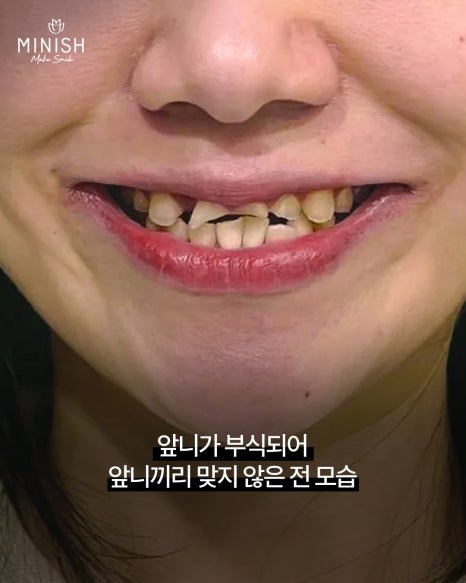
The first patient case shared by Director Yoon that day involved severely worn front teeth, so that even when the mouth was closed, the upper and lower front teeth did not meet.
Director Yoon kept this patient’s vertical dimension unchanged and proceeded with the Minish One-Day method, applying a Minish bridge to the front tooth area.
He also used a Leaf Gauge, which helps find the centric relation position of the temporomandibular joint, for pre- and post-treatment occlusal adjustment to secure an occlusal point that would allow the patient to chew comfortably.

Director Yoon said that he succeeded in restoring comfortable chewing function while preserving the patient’s natural teeth as much as possible. However, he also honestly noted that there was some room for improvement in the morphology of the molar area.
He added, “When the focus is on preserving natural teeth, morphological limitations are inevitable. But continuous efforts to overcome these limitations are absolutely necessary.”
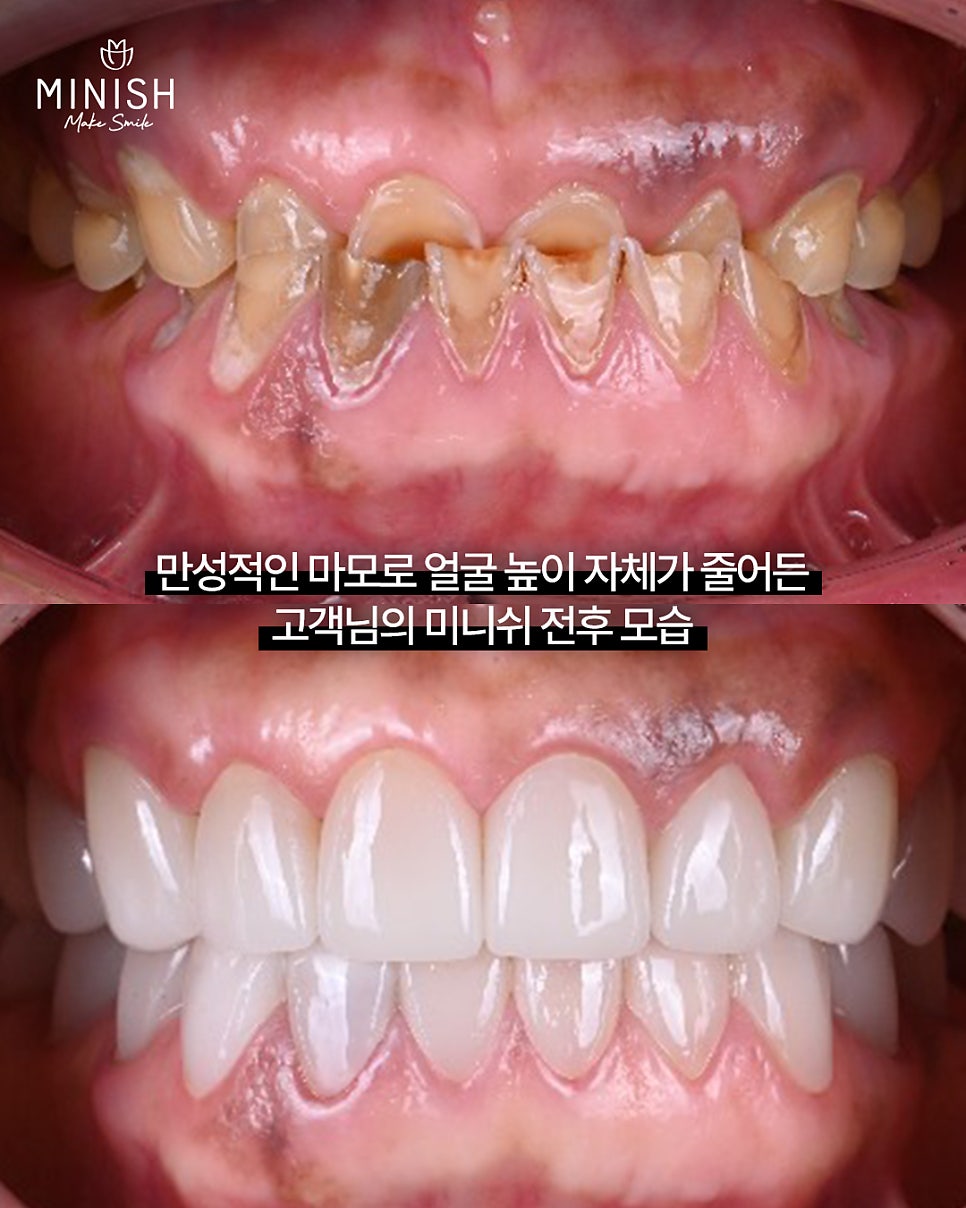
The second patient had severe, long-term tooth wear that had reduced the height of the face itself. In this case, the treatment plan was set in the direction of restoring the vertical dimension. The diagnosis and treatment planning digitally implemented a “two-step approach” devised by Dr. Hobo in Japan. This method is a stepwise treatment approach that considers the patient’s chewing habits and designs the front teeth and molars using different reference points.
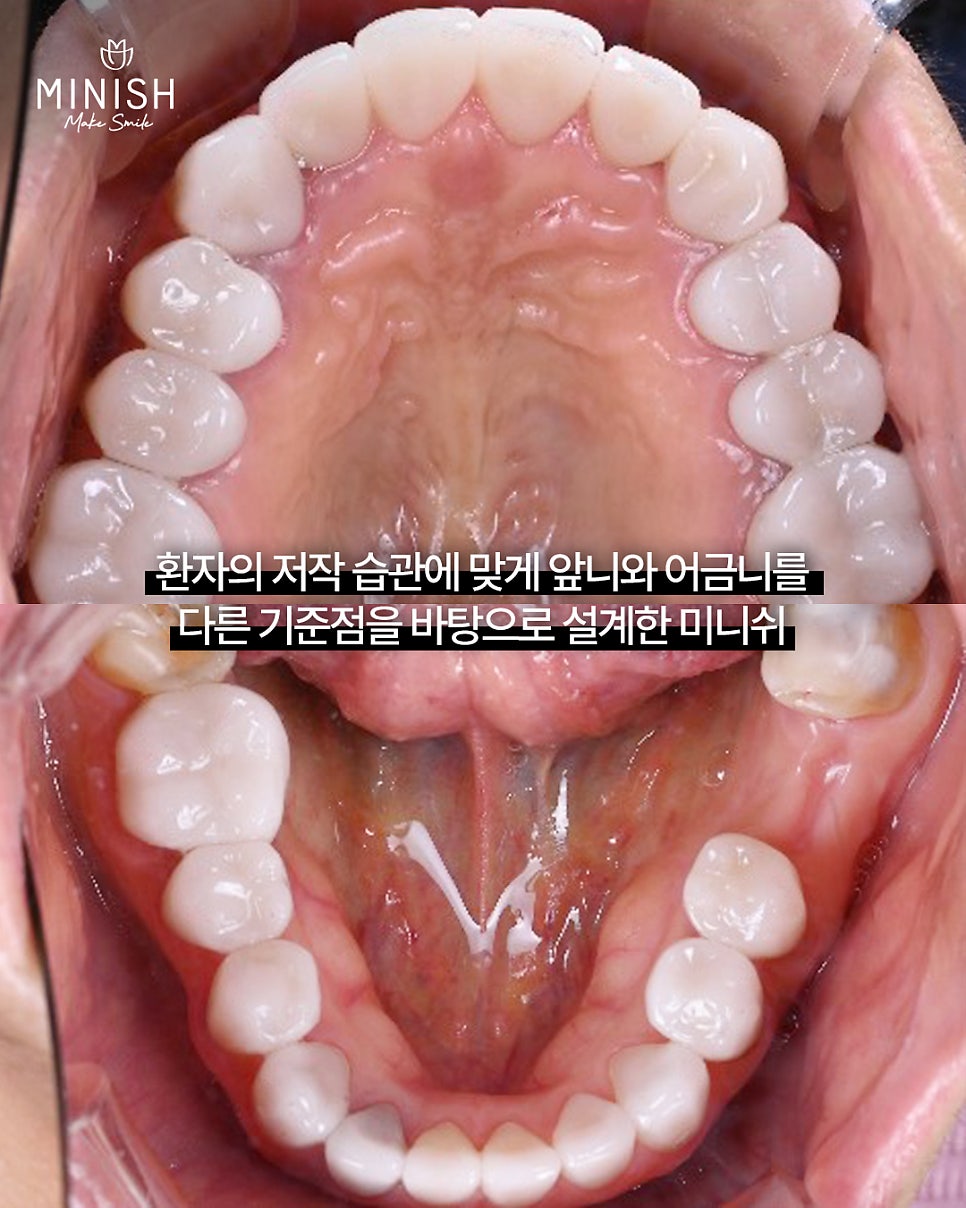
Director Yoon evaluated this treatment case as “a good example in which the anatomical cusps of the teeth were preserved as much as possible while also satisfying chewing function.”
He also added that using a digital articulator in a specialized way greatly improves the precision of restorations and the predictability of treatment. The seminar also shared virtual articulator settings, which provided practical help that can be applied directly in clinical settings.
After the presentation, a discussion session followed. Centering on the first patient case, an in-depth discussion was held on how to strike a balance between “reproducing the occlusal surface” and “preserving existing teeth.” There was also an exchange of views on bonding strength issues that may arise when Minish is bonded to eroded tooth surfaces.
In particular, concern was raised that bonding strength may decrease in eroded dentin areas, and experts agreed that “after preparation (tooth pretreatment), it is essential to remove hardened dentin through long phosphoric acid etching.” The importance of staff training and improving skill level to reduce bonding failures was also emphasized.

Director Yoon emphasized, “The most important thing is to carefully examine each patient with a diagnosis-centered approach,” and added, “We will continue to share diverse clinical experiences and know-how and communicate with our medical staff.”
He also announced plans to hold a small monthly seminar that naturally shares the concerns and insights medical staff encounter in the clinic.










