In the end, I had to have one molar pulled. I thought it could be saved, but its condition was worse than expected, and even root canal treatment had its limits. After the extraction, my body felt the emptiness sooner than my mind did. In my head, it was just the loss of one molar, but every time I ate, the tip of my tongue would unconsciously search for the empty space, and as it became harder to chew naturally like before, meals themselves started to feel stressful. It’s only one missing tooth, but food didn’t taste as good, and without the satisfaction of chewing, I felt less full too. I could feel the strain on the surrounding teeth, and chewing on only one side made my jaw feel stiff. The thought that I shouldn’t leave it like this grew stronger and stronger. Even so, I couldn’t easily decide whether I should start an implant right away. But because it’s not just a matter of enduring discomfort and because the jawbone can also be resorbed, I needed to understand well what problems arise if I don’t get an implant and when and what kind of preparation is needed if I do get treatment.
These days, when a tooth is lost, getting an implant is often accepted as the natural thing to do, but since the implant procedure itself is not an easy decision, there are also people who hesitate or put it off. The problems that arise after a molar extraction if you don’t get an implant are actually complex and can appear in a chain reaction, so it is important to understand the treatment properly and prepare for it.
When a molar is extracted, many people think, “It’s a tooth you can’t see, so maybe I don’t really need an implant,” but molars do more than just chew food. Because they play a major role in stabilizing the overall structure and function of the mouth, leaving the space empty can cause problems in the long term.
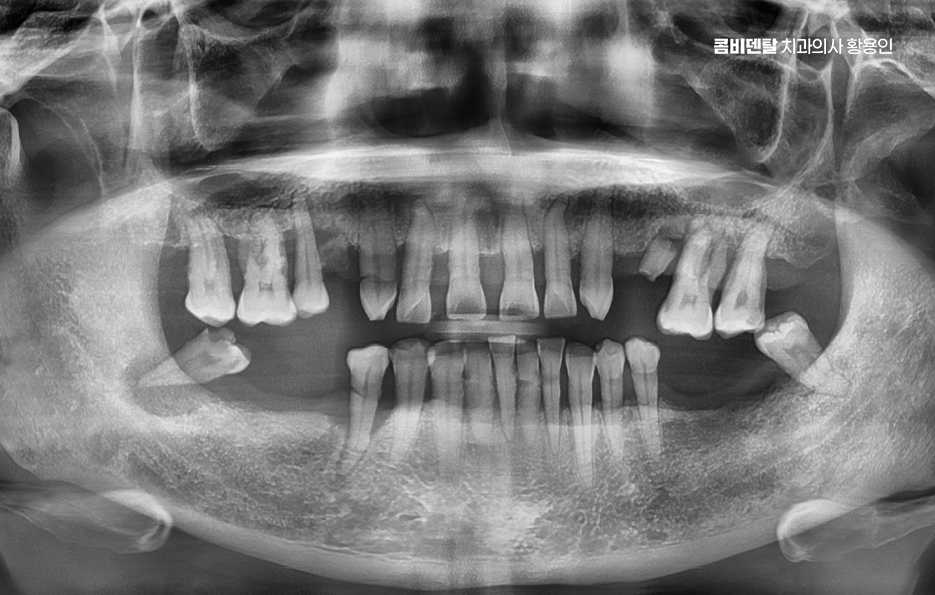
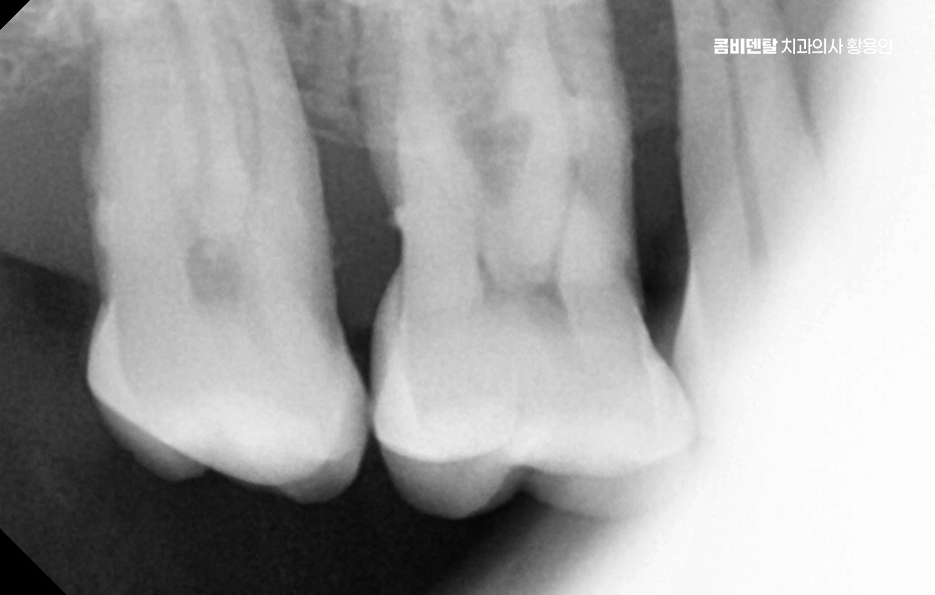

The first problem that appears if you don’t get an implant after a molar extraction is tooth movement. Human teeth rely on one another to maintain balance. When one molar is lost, the adjacent teeth gradually tilt inward as if collapsing to fill the space, and the teeth above and below that were once aligned can shift out of position by drifting downward or upward when their opposing tooth disappears.
In the end, the entire dental arch becomes twisted and the bite is disrupted. This is not just a simple alignment issue; it can lead to changes that also affect the temporomandibular joint.
The second issue if you don’t get an implant after a molar extraction is reduced chewing function. Molars are the main teeth responsible for chewing, so losing even one breaks the balance of chewing force. As a result, the opposite molars may be overburdened, or the front teeth may be used too much, making other teeth more prone to wear or looseness. In particular, if food cannot be broken down well, it can also affect the digestive system.
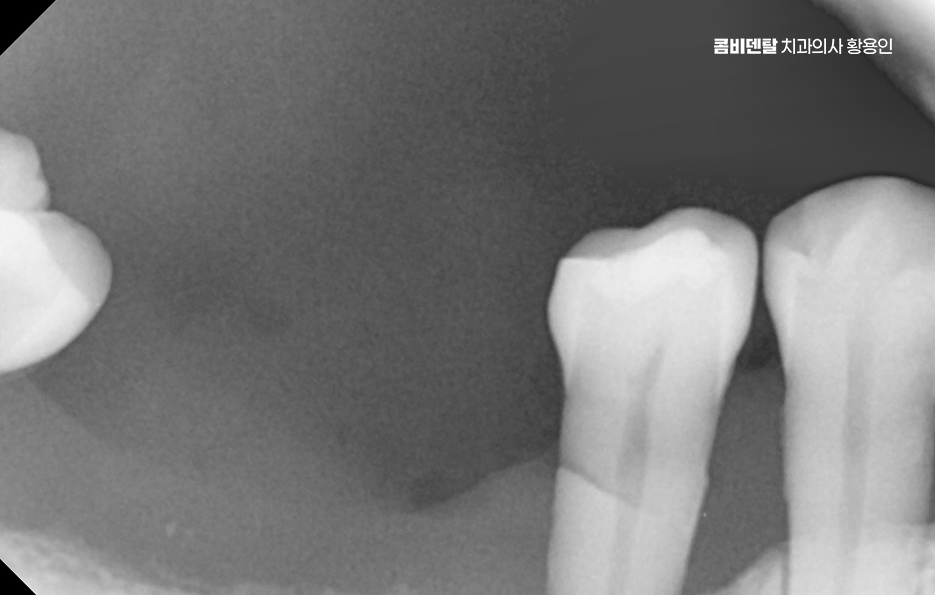
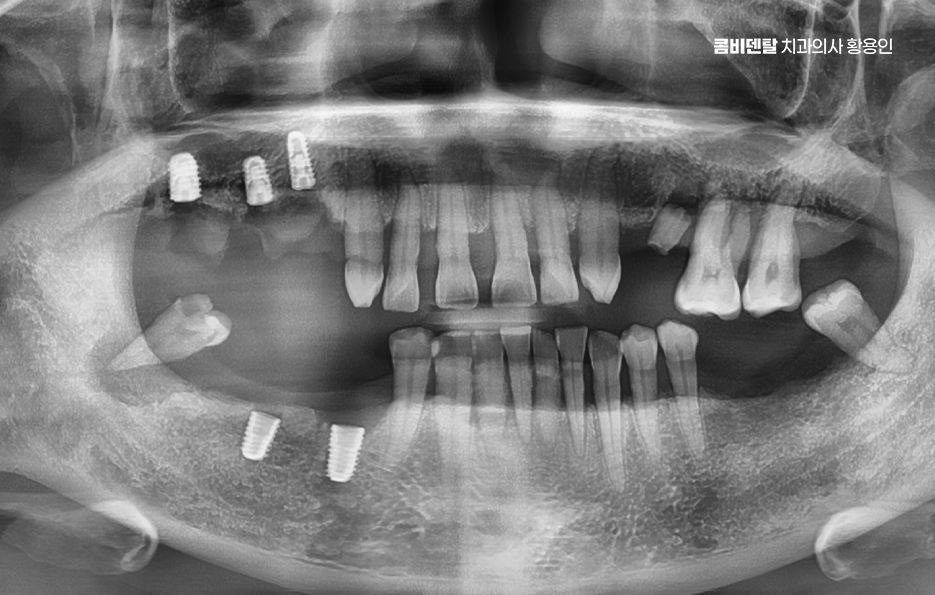
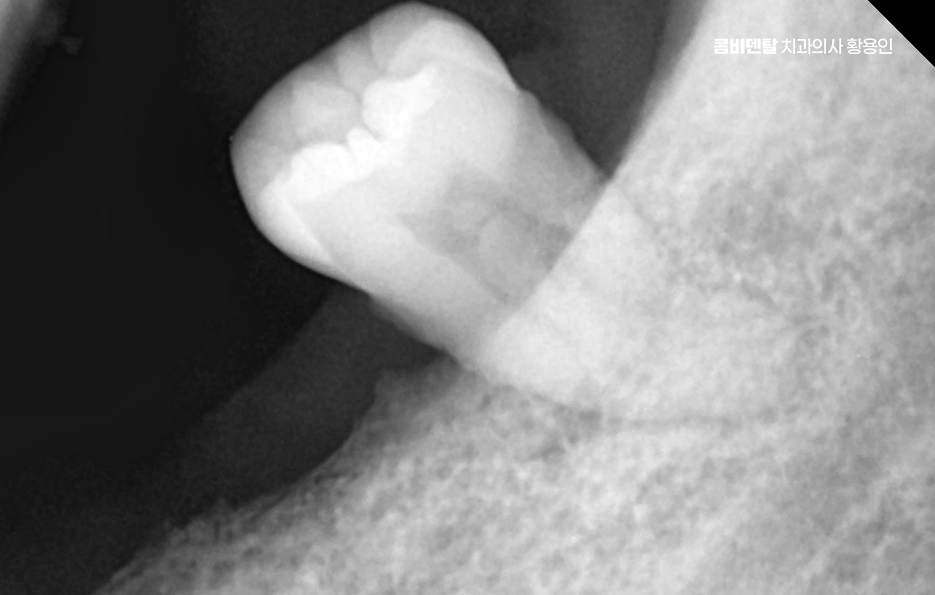
And in fact, the problem of bone resorption is very significant. In other words, it is the gradual loss of the jawbone. The bone is maintained only when the tooth root stimulates the jawbone, but if the tooth is left missing, the bone in that area slowly begins to resorb, as if sinking down.
If this becomes severe, even if you want an implant later, there may not be enough bone, so bone grafting may be needed as well, and the scope of surgery becomes larger. The longer the area is left untreated without an implant, the more difficult the treatment can become, and the higher the cost can be.
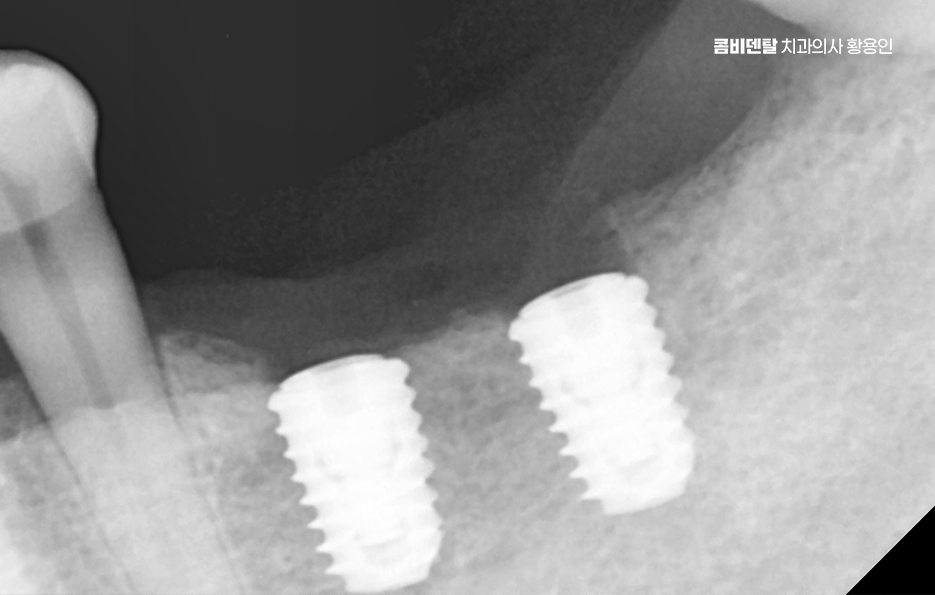
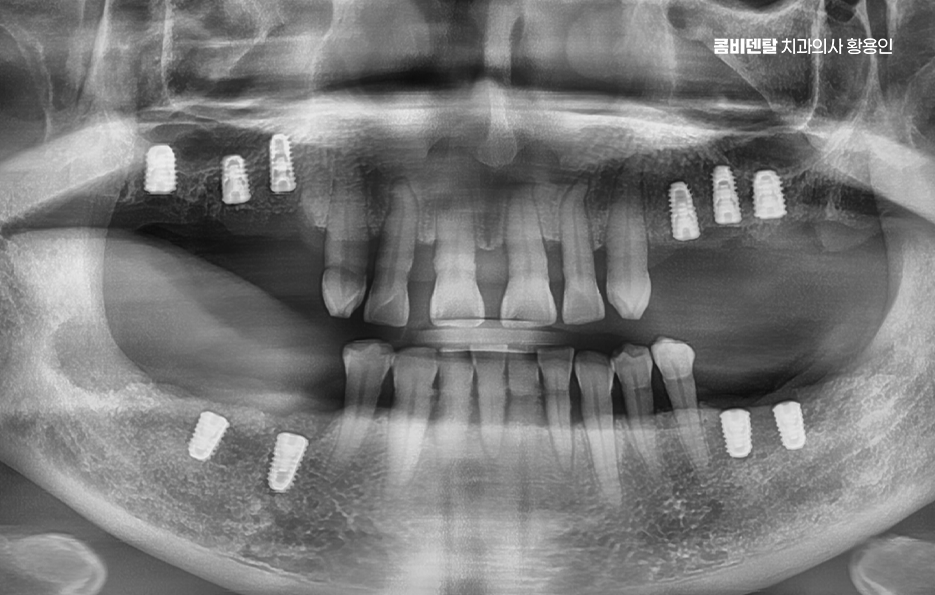

So, after a molar extraction, what is the best way to get an implant? The first is not to miss the timing. Ideally, the implant should be placed within 3 months after extraction. In fact, these days, depending on the case, there are more and more instances of so-called “immediate placement,” where the implant is placed on the same day as the extraction. That is why it is ideal to make an implant treatment plan together with the extraction.
To carry out treatment that suits you, an accurate diagnosis and plan are important. After precisely evaluating the nerve position, bone amount, thickness, and other factors through CT scans, it is important to place the implant in a position that matches the bite and dental arch structure. If it is placed in the wrong position, it can be difficult to use for long, and pain or inflammation may develop later.
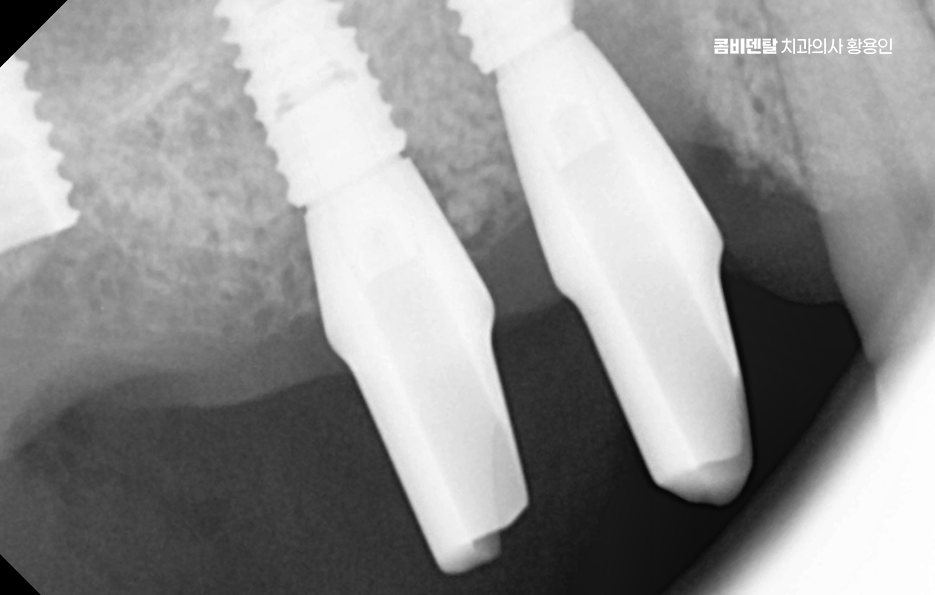

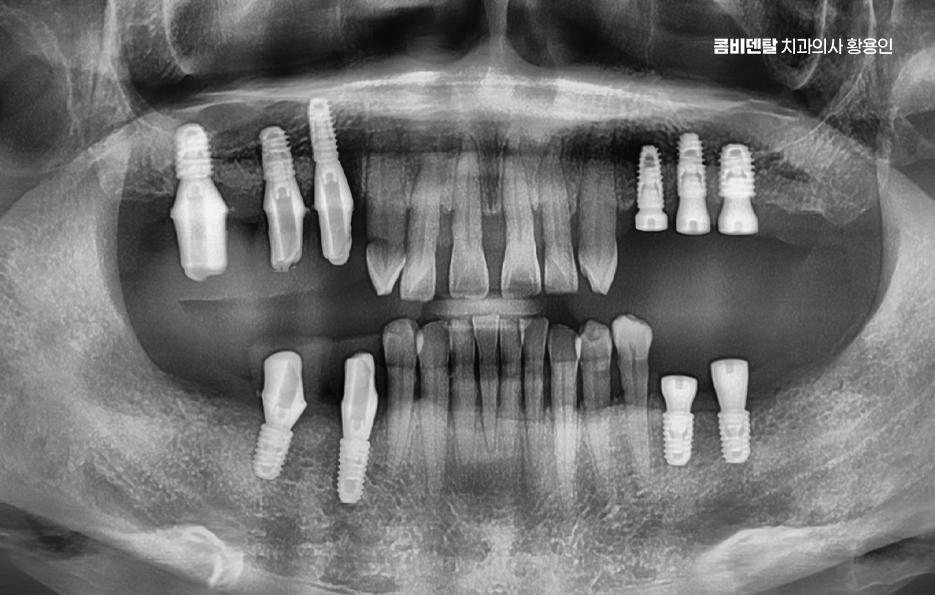
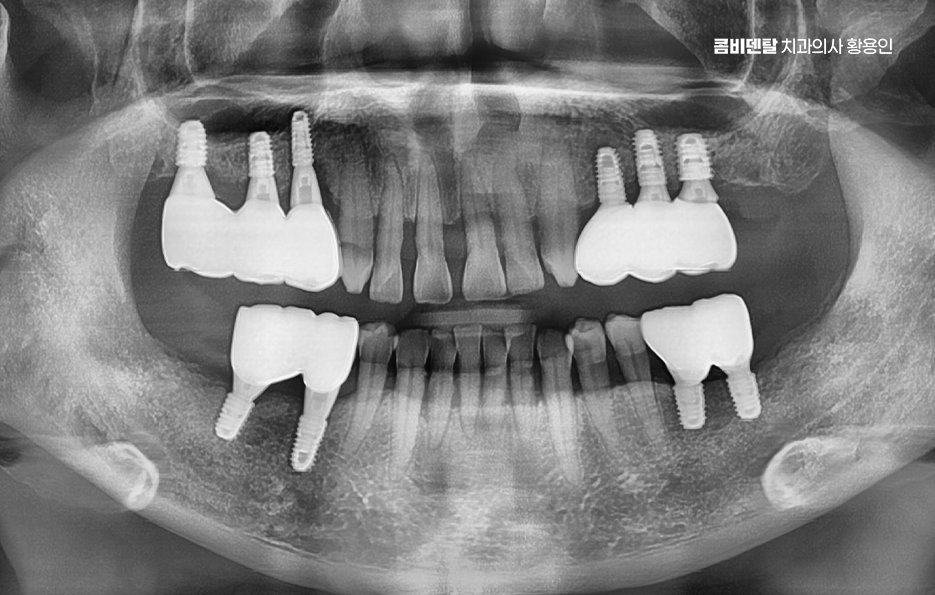
It is said that aftercare is even more important than the initial surgery when it comes to implants, so it is important to have the procedure done under a well-designed treatment plan from the start, and to do a good job with follow-up care afterward. That is what helps maintain the implant’s lifespan.
An implant does not develop cavities like a natural tooth, but it can develop a problem called peri-implantitis. This is inflammation, like periodontitis in natural teeth, in which the bone gradually dissolves and the gums swell. If left untreated, the implant can eventually loosen and fall out. That is why regular scaling and checkups at the dentist at the scheduled times are necessary, and you should also consistently take care of it with tools such as a toothbrush, interdental brush, and water flosser. Because treatment should be viewed from a long-term perspective, from the treatment plan to maintenance, I hope you will also carefully choose a dental clinic that can stay with you for the long run.








Previous image
Next image








Previous image
Next image










Previous image
Next image










Previous image
Next image





















































