Losing just one molar didn’t shake me this much. It was uncomfortable, but I kept telling myself I could chew on the other side and get through it, and I thought I would eventually get used to it over time.
But when I lost not just one, but two, and then quite a few more molars, the situation felt completely different. I could feel in my body that the balance of chewing had collapsed, and it wasn’t just a sensory issue—it was affecting my whole daily life.
Meal times changed first. Foods I had once eaten without thinking became a burden, and I started avoiding chewy or hard foods altogether.
The menus I naturally chose changed too, and I found myself selecting softer foods. On the surface, it may have seemed like a minor change, but underneath it, there was always hesitation: would it be okay to chew this?
Molars were teeth I rarely noticed in everyday life. They weren’t as visible as the front teeth, and if they didn’t hurt, there was hardly any reason to think about them. But once I lost several of them, I realized anew just how important their role had been. It felt like the center of chewing force had collapsed, and because I kept chewing on only one side, there were more days when my jaw felt stiff and sore.
What was hard was the feeling that I was gradually shrinking back into myself. When I had to eat with other people, I started worrying about the menu first and thinking ahead about whether difficult foods might be served. Even meat and nuts, which I used to enjoy, had become things I looked at cautiously. I felt unfamiliar with myself, and a little upset too.
After losing a significant number of molars, implant treatment naturally came to mind. Continuing like this seemed like it would only become more uncomfortable, and after hearing that the remaining teeth could also be put under stress, I felt that postponing it any longer wasn’t the answer. Still, the word implant felt heavy.
The idea of replacing not one but multiple molars with implants was not easy to accept. I kept imagining how long the treatment period would be, how complicated the molar implant process would be, and how much pain there might be.
As such, molars are the teeth that bear the greatest force when we chew food. If the front teeth are for cutting, molars are for crushing and grinding. So even losing just one molar can change eating habits, and chewing only on the opposite side can throw off the overall balance of the bite.
Many people think molars are in a less visible area, so they can just put up with discomfort, but in reality, the longer they are left untreated, the more strain builds up on the surrounding teeth and the temporomandibular joint. That is why the molar implant process after tooth loss can be not just a simple choice, but an important process for restoring function.
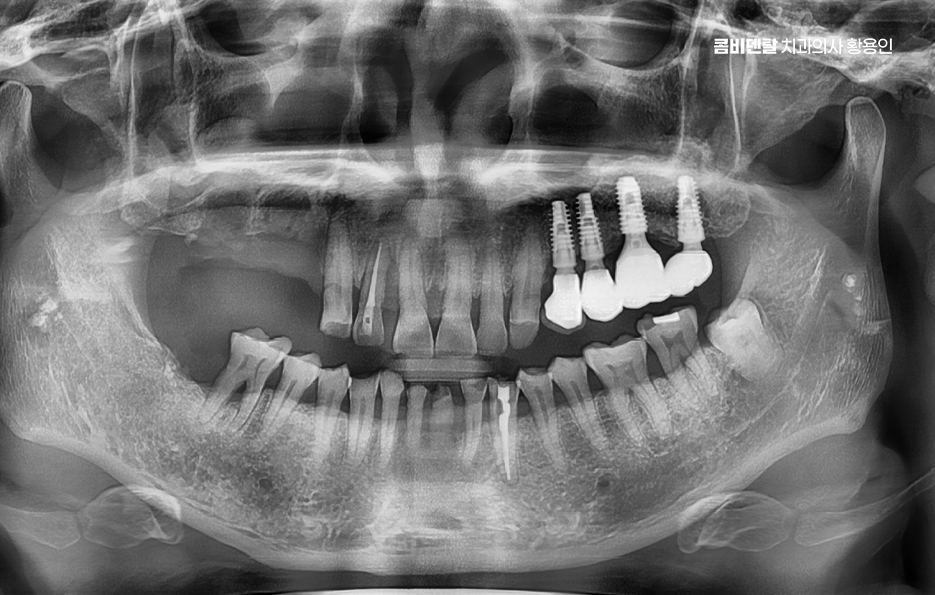
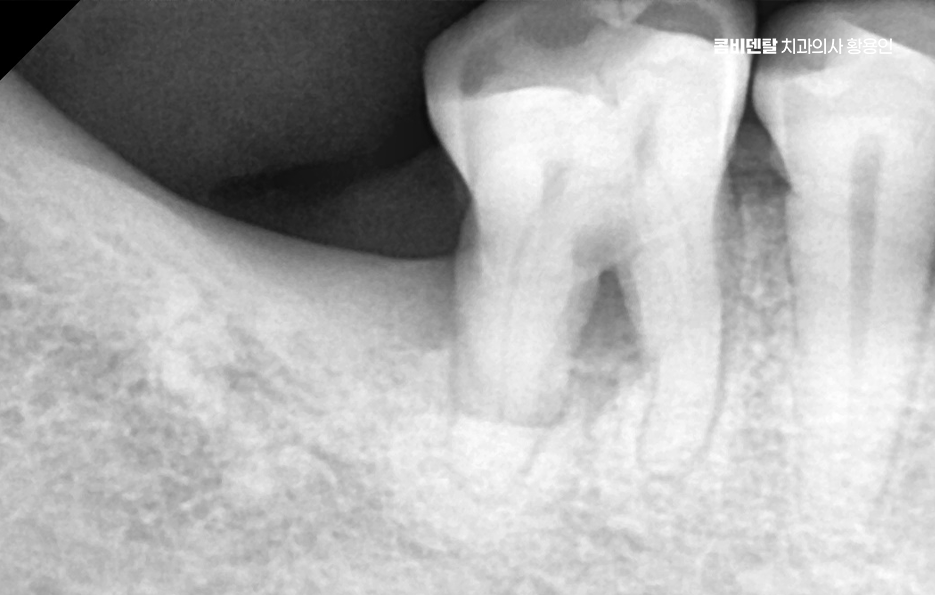
The need for molar implants lies in restoring chewing function. Without molars, people often cannot chew food thoroughly and end up swallowing it too soon, which places a burden on the digestive system and may even lead them to avoid certain foods altogether. Also, if a one-sided chewing habit develops, the teeth and gums on the unused side can gradually weaken.
On the other hand, the side that is used continuously can become overloaded, increasing the risk of wear or cracks. In the long run, the loss of molars can have a chain reaction on overall oral health.
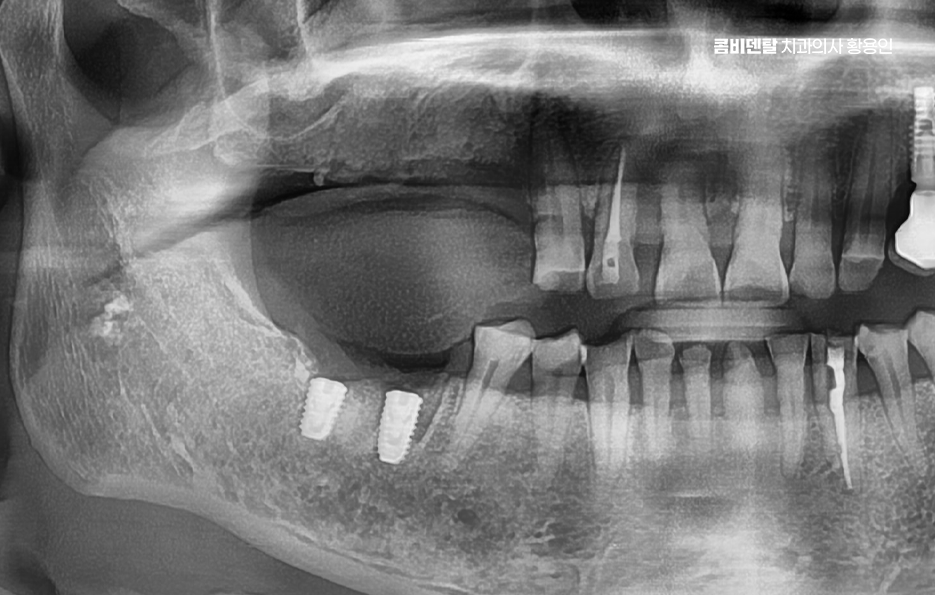
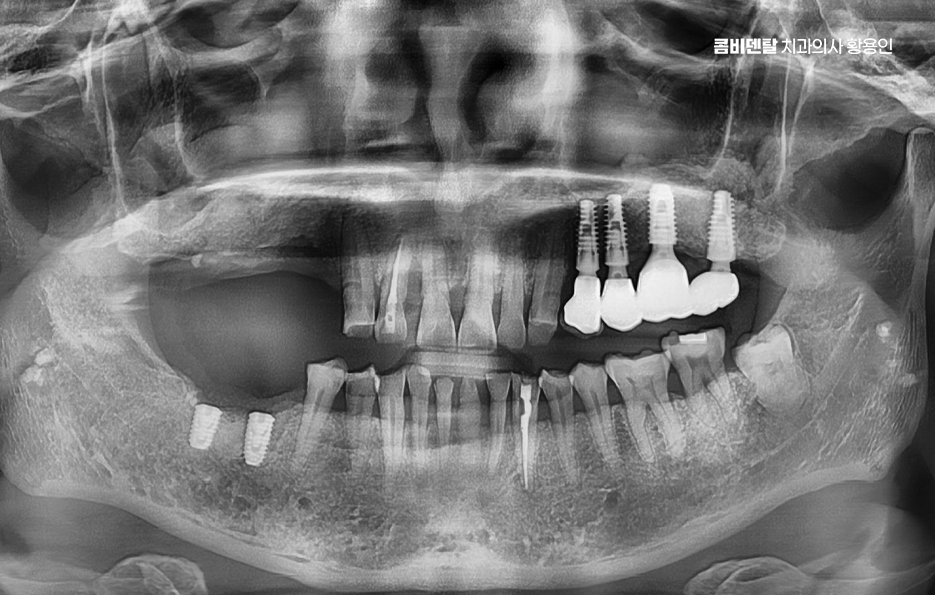
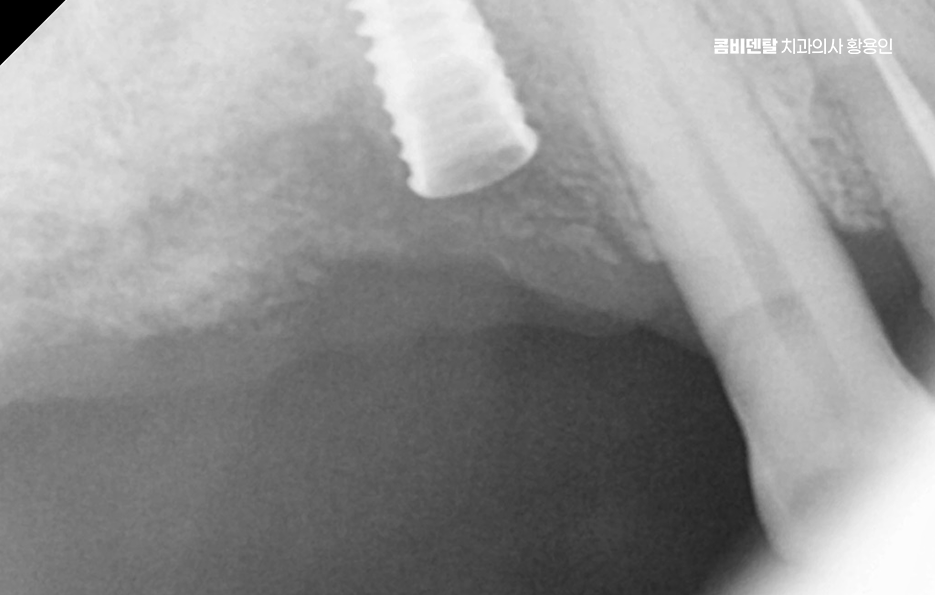
Teeth support one another and maintain balance, but when one is missing, the neighboring teeth can tilt into the empty space. If left untreated, the alignment can become distorted, and if you later try to have prosthetic treatment, the lack of space can make things more complicated. Teeth that bite together with the missing tooth can also gradually drift downward or upward when there is no opposing tooth.
The molar implant process begins with a detailed diagnosis. Because an artificial root is placed into the jawbone, checking the bone condition is essential. Panoramic X-rays or 3D CT scans are used to check bone height and width, as well as the location of nerves. In particular, lower molars are close to the inferior alveolar nerve, so accurate positioning is important, and for upper molars, the distance to the maxillary sinus also needs to be considered.
If there is enough jawbone for the implant, it can be placed right away. But if a tooth has been left out for a long time after extraction, the bone may have resorbed and become insufficient. In such cases, bone grafting may be done first or at the same time. Since molars bear strong chewing force, firm initial stability is necessary, and when considering long-term retention, precise bite alignment is an important factor in this area.
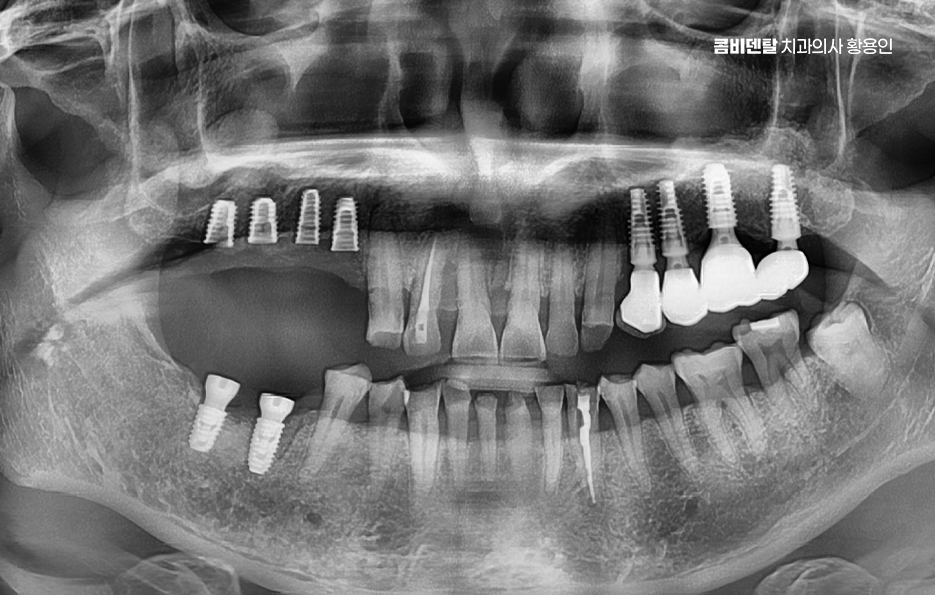
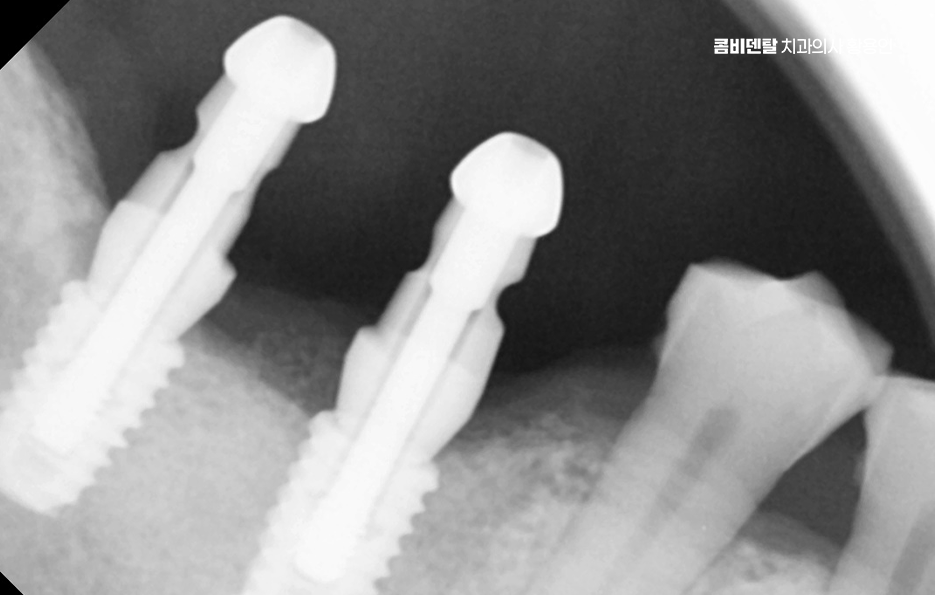
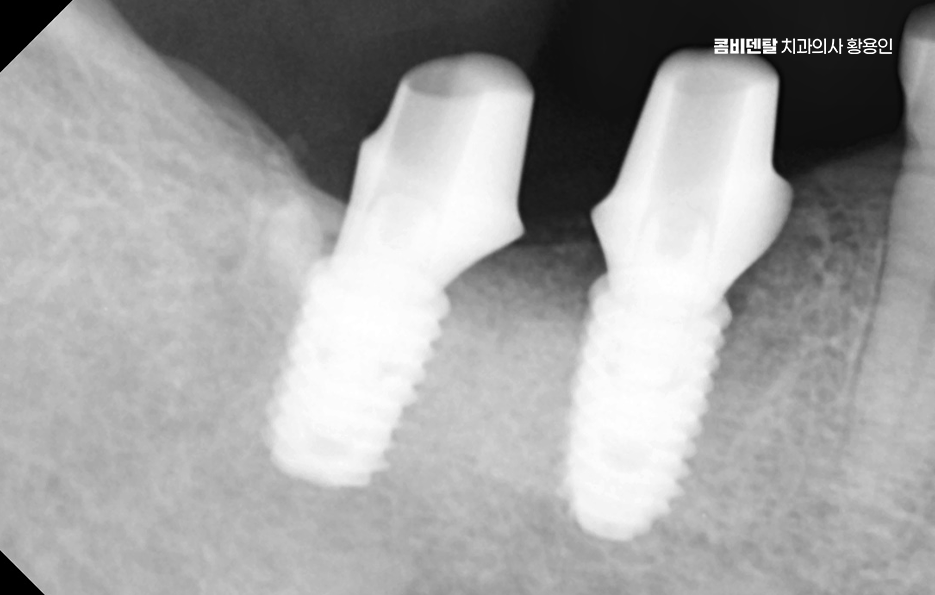
On the day of surgery in the molar implant process, after local anesthesia is given, the gums are incised or accessed with a minimally invasive approach, and the implant is placed into the bone. After surgery, a certain period is needed for osseointegration, which is the process by which the implant and bone firmly bond together.
Once osseointegration is complete, the abutment is connected, impressions are taken, and the final prosthetic tooth is made. Molar crowns are designed to consider both strength and bite harmony. Because this area concentrates chewing force, adjusting the height and contact points is important, and if the bite does not match, screws may loosen or problems may develop in the prosthesis. That is why even after placement, bite checks, regular examinations, and scaling can be important.
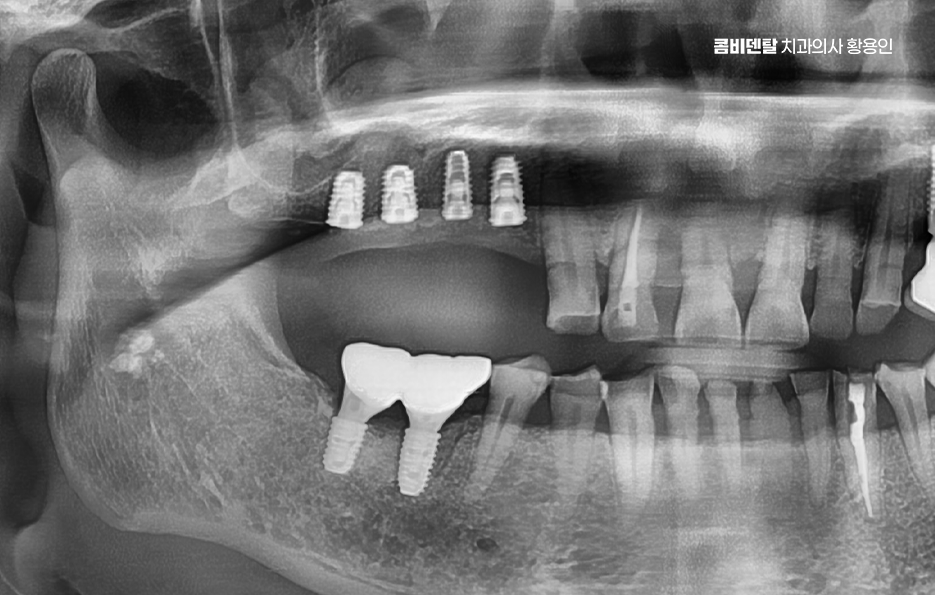
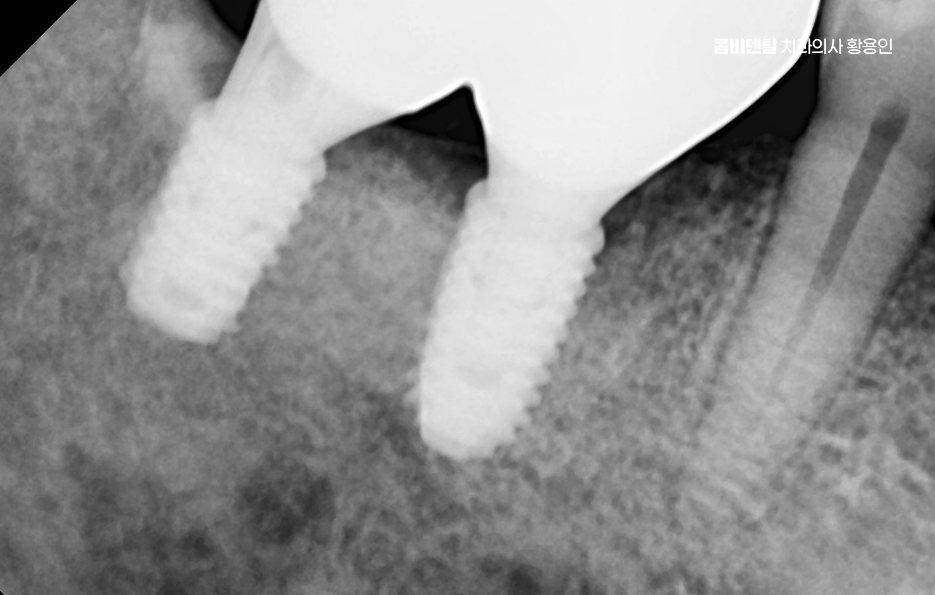
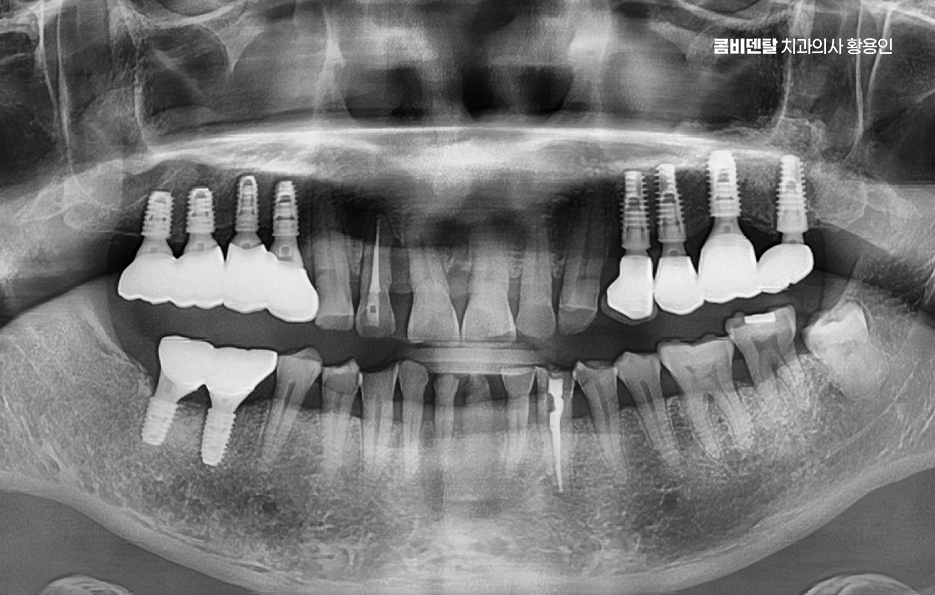
People often think implants cannot get cavities, but gum inflammation can certainly occur. If peri-implantitis develops, the bone can be lost and the implant may fail. So it is important to manage the area carefully with interdental brushes or dental floss and to check bone condition through regular examinations. In particular, molars are a place where food gets stuck easily, so they require extra attention. In that sense, not only the treatment plan but also long-term care, including maintenance, is important.
Molars are not easy to see, but they are at the center of oral function. At first, losing one molar may not seem like a big difference, but over time, that gap can come back as a problem. Since implants are a treatment to restore lost function and protect the remaining teeth, I hope you prepare in advance when tooth loss occurs and approach it with a long-term perspective if you proceed through sufficient diagnosis and planning.





Previous image
Next image




Previous image
Next image




Previous image
Next image




Previous image
Next image