| Ectropion - A condition in which the eyelid margin has turned outward. When this happens, there is a gap between the eyeball and the eyelid margin, causing dryness of the eye. It is more commonly seen in the lower eyelid because of gravity, mechanical forces, the shorter vertical height of the lower tarsal plate compared with the upper tarsal plate, and the laxity of the lower tarsal plate and canthal tissues. [Quoted from Kang Jin-seong, Latest Plastic Surgery, Vol. 1, p. 751. There are three causes of ectropion: 1. senile ectropion 2. cicatricial ectropion 3. iatrogenic ectropion. 1. Senile ectropion occurs when age-related loosening of the eyelid canthal ligaments and related structures weakens the lower eyelid, causing it to turn outward. It is especially common after lower blepharoplasty in older patients. - When the lower eyelid is weak and too much skin is removed - |
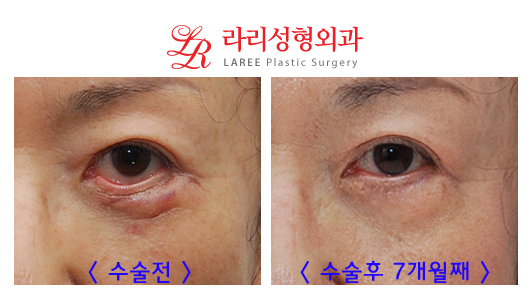
#Complications of lower blepharoplasty
| This is a case of ectropion correction in a patient with a combination of senile and iatrogenic causes. 2. Traumatic ectropion often develops during the healing process after the lower eyelid is torn in a traffic accident or injured by a sharp object. When looking straight ahead, it may not seem severe, but when the head is bent down and the gaze is directed upward, the lower eyelid becomes severely turned outward due to adhesion to the inner muscles and other tissues. |
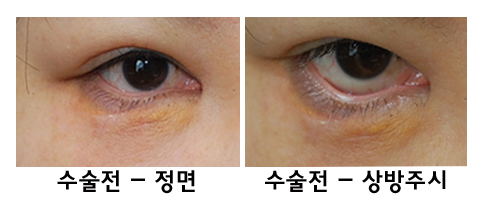
| If you only look at the preoperative frontal photo, the ectropion may not stand out, but it becomes clearly visible in upward gaze before surgery. Compared with the photo after surgery showing good correction of ectropion from the front, you can see that before surgery the lower eyelid was slightly pulled downward by the ectropion. |
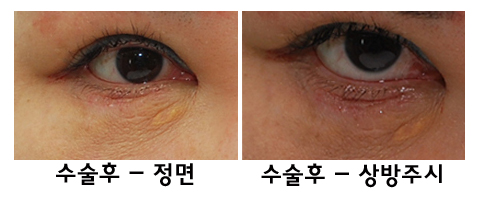
| In particular, if you compare the exposed white part of the eye before surgery, you can more easily notice the difference. |
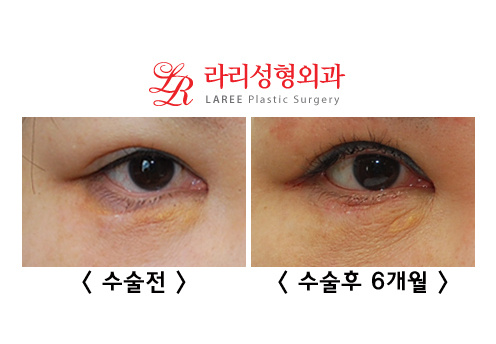
| In fact, the discomfort that patients with lower eyelid ectropion complain about most often is that the eyelid turns outward even more in upward gaze. |
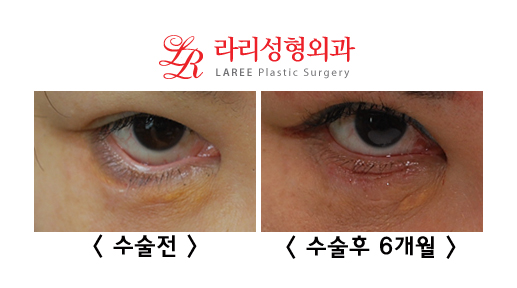
| After surgery, an incision scar on the lower eyelid is somewhat visible, but over time it tends to fade significantly. 3. Iatrogenic ectropion is actually what doctors must be most cautious about. It is a relatively common complication, to the point that surgeons performing lower blepharoplasty may experience it at least once. As mentioned above, extra caution is needed when operating on elderly patients whose lower eyelids lack elasticity. Two tests that should definitely be performed before lower blepharoplasty in elderly patients are the pinch test and the lid distention test. If these two tests indicate significant eyelid laxity, the orbicularis muscle or skin should not be overresected during lower blepharoplasty. |
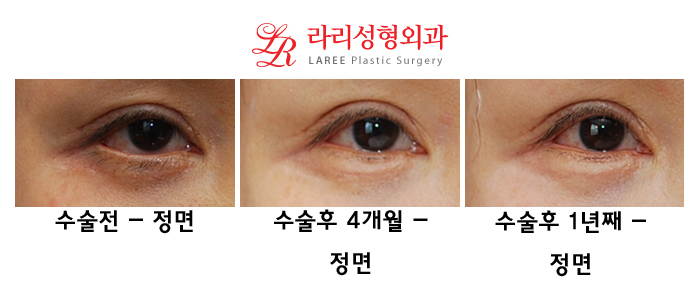
| This patient came to Larri Plastic Surgery with ectropion that developed after lower blepharoplasty performed at another hospital three months before undergoing ectropion correction surgery. As in most cases of ectropion, the degree of outward turning may not be obvious in the frontal photo unless you are a specialist or the patient themself. However, the patient often complains significantly of discomfort caused by corneal dryness or dry eye symptoms. |
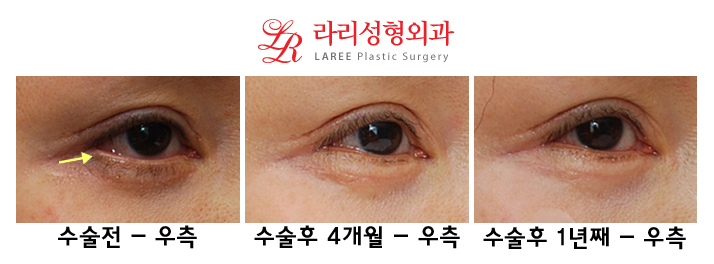
| In the lateral view, conjunctival edema is visible, caused by separation of the eyeball and the tarsal plate, as indicated by the arrow. When the eyelid and eyeball are separated like this, tears do not reach the cornea properly, leading to a strong feeling of dryness. |
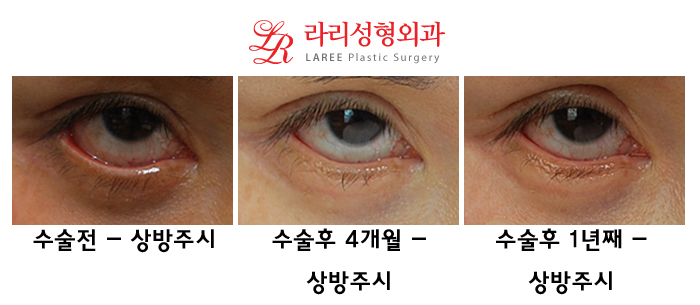
| Again, in upward gaze, the tarsal plate is completely separated from the eyeball and turned outward, exposing the palpebral conjunctiva. After ectropion correction, you can see that the outward turning has improved significantly, and it also shows well that there has been no recurrence even after one year.











