Hello.
I am Heo Jae-won, a board-certified plastic surgeon who studies surgeries that make people look younger.
Today, in a different format, I’d like to select a few good questions from the private comments left on the blog and share them in a Q&A format.
Before looking at the question, I think the post below will help you understand it a little better.
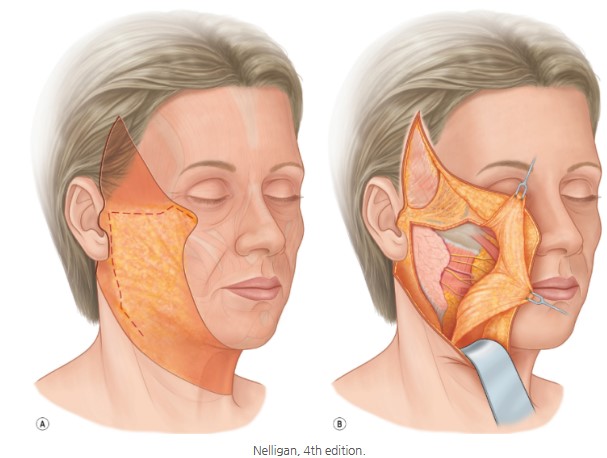
“Hello, doctor. I read your blog post saying that the existence of the SMAS fascia may not be real.
I heard that the SMAS supports the skin. If the existence of the SMAS is uncertain, does that mean its role is uncertain too?”
This was a sharp question that logically asked about the structure and the role of the fascia.
Plastic surgery may look simple on the surface, but in reality, it is carried out through a combination of anatomical calculation and detailed strategy.
So when I receive questions like this, I’m always very glad. I also thought that among those reading this post, many people might have similar questions.
The first question about the SMAS fascia
Q. I heard that the SMAS supports the skin. If the existence of the SMAS is uncertain, does that mean its role is uncertain too?
This was a concern I had kept in my heart for a long time as well.
In the operating room, there were patients in whom the SMAS was clearly visible, but there were also cases where no structurally clear SMAS could be found no matter how hard I looked.
Textbooks in plastic surgery naturally say that it exists, and countless papers say that “pulling the SMAS is the key to a facelift,” but in reality, it is not always visible...
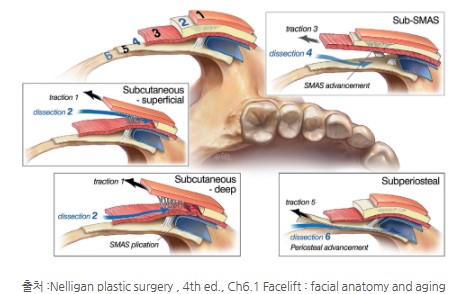
At first, I thought it was because my technique was lacking.
I worried endlessly about whether I should look deeper or change direction.
I found the answer in the wording by Minelli, which I introduced in the link.

"The SMAS fascia can be forced into a layer depending on the thickness chosen by the dissector, but that is an artificially created structure, like thinly slicing cheese."
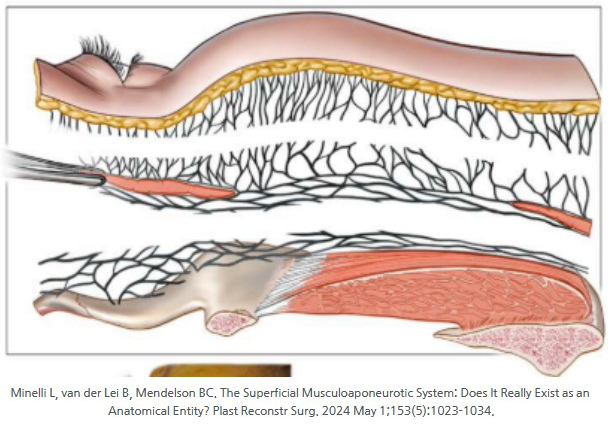
In other words, SMAS does not always exist as one clear anatomical structure; at times, it may be closer to a fantasy created in the hope that surgery will go well, as we expect.
After realizing this, I changed my approach.
I came to recognize that the purpose and the action are different.
First, I set the soft contour I want (the purpose), and then I perform the action of lifting (dissecting) the SMAS to refine that contour (the action).
On the other hand, if you indiscriminately lift and pull the SMAS without a purpose, I do not think that sagging or contours can all be solved that way.
It is subtle, but it makes a big difference. That is why these days I explain it like this.
Whether or not to dissect the SMAS is now a thing of the past, and what is actually more important is not forcing yourself to find a layer that does not exist, but focusing more on how to reposition the structures that have actually sagged (the nasolabial fat pad).
In that process, of course, the act of so-called “dissecting the SMAS” is still always done, but I no longer obsess over it.
So this has become an era that requires more precise surgical planning and individual anatomical judgment.
In the next post, along with the second question, I will look in more detail at the effects of liposuction and AccuSculpt on the SMAS.
Thank you.



