Hello.
I am Dr. Huh Jae-won, a board-certified plastic surgeon at Ipjeok Plastic Surgery, where I perform facial rejuvenation surgery.
Today, I’d like to talk about skin necrosis, one of the complications that always puts pressure on surgeons every time we perform facelift surgery.
Skin necrosis is not something that can simply be dismissed as a problem caused by a poorly performed operation.
It is also deeply related to the anatomical limitations of the facial vascular structure.
To understand this issue accurately, it is helpful to look in chronological order at several anatomical studies published over the past 20-plus years.
Today, I will focus on studies published in the 1990s and 2000s.
How common is skin necrosis?
In fact, skin necrosis after a facelift is a very rare complication.
However, once it occurs, it places a major psychological burden not only on the patient but also on the surgeon.
According to the literature, the incidence is reported to be about 1.1% to 3%.
This comes from the research of Dr. Baker, a leading figure in the field of facelifts.
(Baker DC. Complications of cervicofacial rhytidectomy. Clin Plast Surg. 1983;10(3):543–62.)
That means it is a “rare but not negligible complication” that can occur in one or two out of 100 patients.
“I don’t have that problem because I’m good at surgery.”
That may sound reassuring to patients, but it is not a realistic way to think about it.
Rather, acknowledging the risks that can occur probabilistically, preparing preventive measures to reduce those risks, and knowing how to respond if they do occur is what I believe reflects a truly safe surgical approach. I, too, continue to study and make improvements to reduce this 1% chance even further.
What causes skin necrosis?
The causes of skin necrosis can be broadly divided into two categories.
-
Preventable causes – cases that can be reduced through the surgeon’s technique or attention
-
Hard-to-prevent causes – cases that are difficult to avoid because of anatomical structure or blood flow issues
First, let’s look at the parts surgeons need to be careful about.
-
When trying to leave the SMAS thick, the skin layer is dissected too thinly
-
When the skin is pulled too tightly
-
When there is mechanical injury during the operation
These situations can be sufficiently prevented with refined technique and careful adjustments.
Maintaining an appropriate skin thickness, distributing tension, and minimizing injury are the keys.
The unavoidable cause - blood flow problems
But the most fundamental cause is insufficient blood flow to the skin.
If the skin does not receive enough blood supply, the tissue cannot withstand the stress no matter how precise the surgery is.
So why does this blood flow problem occur in facelifts? The answer lies in anatomical research.
In 2004, Dr. Wolff’s team in Germany dissected donated cadavers to study which blood vessels supply the blood flow to facelift flaps.
The results were as follows.
-
Facial artery: supplies blood to the central face through small perforators near the side of the nose, the corners of the mouth, and under the jaw
-
Transverse facial artery (TFA): supplies blood to the lateral face through small perforators below the cheekbone
-
Superficial temporal artery (STA): contributes in part, but its role is limited
In other words, it became clear that the main blood supply to the lateral face comes from the TFA.
The problem begins here.
During facelift surgery, the perforators of the TFA must inevitably be cut while dissecting the flap.
In the end, blood supply to the lateral area is blocked.
So why doesn’t skin necrosis occur in most patients?
That is because the perforators of the facial artery remain and provide substitute blood flow to the area that the TFA had been supplying.
In other words, it is a structure that survives through bypass blood flow.
To use a water tank analogy, even if one of three faucets is turned off, the tank can still remain full if the other two provide enough water.
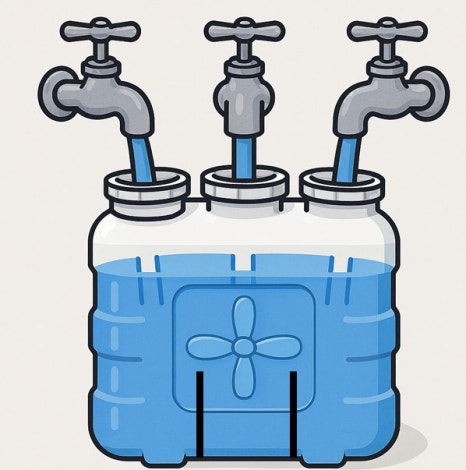
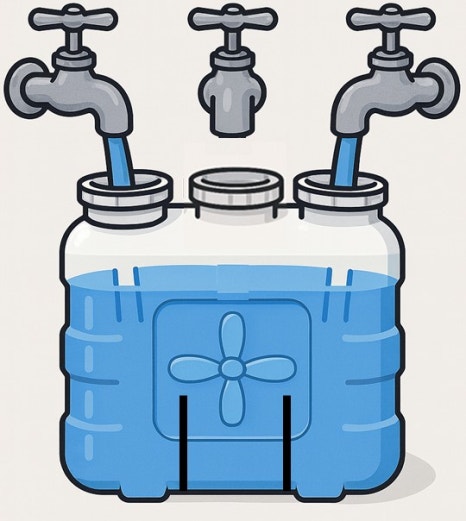
However, in smokers, patients with diabetes, or cases where the dissection range is taken too broadly, this bypass pathway can be compromised and blood flow may not hold up.
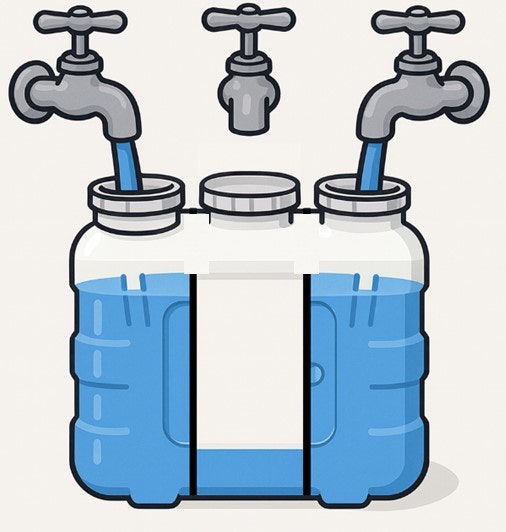
The result is skin necrosis.
That is why, for patients who smoke and come in for facelift consultation, we advise them to quit smoking for a certain period before surgery.
Dr. Wolff’s team concluded the following.
“It is important not to extend skin dissection near the nasolabial fold.”
The reason is that if the dissection passes beyond that boundary, the facial artery can also be damaged, and the flap loses blood flow completely.
2009 Rohrich study: anatomical confirmation
Later, in 2009, Professor Rohrich’s team in the United States (the Dallas group) reanalyzed this issue using advanced technology.
Their results clearly showed that the key blood supply to the lateral face flap comes from the transverse facial artery (TFA).
Both deep plane facelifts and dual plane facelifts involve some degree of cutting of this vessel, and when that happens, a relative ischemic area forms in the lateral face. In most cases, however, surrounding vessels compensate for it. Rohrich’s team presented the following conclusions.
-
The lateral facelift flap depends on TFA perforators.
-
When these are cut, blood flow decreases.
-
However, necrosis does not occur in most cases because surrounding blood flow, including that from the facial artery, compensates.
-
That said, if the patient smokes, has diabetes, or has congenital abnormalities in vascular patterns, the bypass pathways may be insufficient and the risk of necrosis may increase.
When surgical design, dissection range, and the patient’s vascular condition overlap, this complication can appear.
In other words, “it is rare, but it can happen.” That is the most realistic way to view skin necrosis.
Therefore, it is important for the physician to be aware of this before surgery and to properly assess the patient’s condition when deciding whether to proceed.
Today, I have summarized one of the important complications in facelift surgery, focusing on the 2004 Wolff study and the 2009 Rohrich study.
If there is an opportunity, I would like to take time to talk about the preventive measures I use to minimize this possibility.
Thank you.


