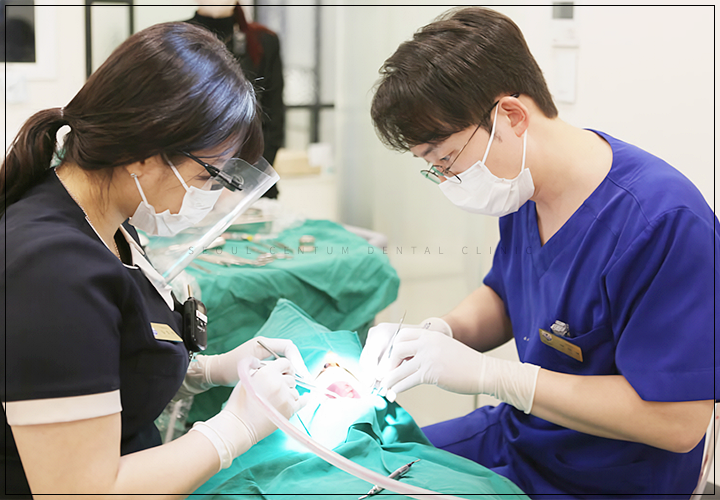
When implant bone grafting is needed
If you want to check in detail

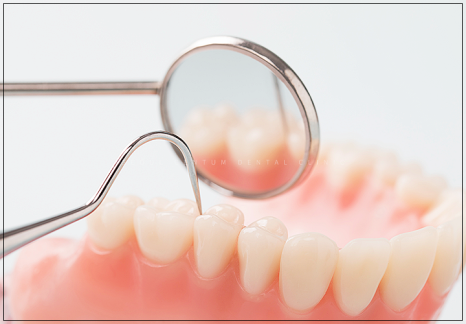
Looking at people who want to have implants placed,
they often look into it as a way to fill the empty space after extraction,
following fractures caused by unavoidable accidents or chronic oral habits such as
teeth grinding and clenching,
or after chronic pulpitis or periodontitis leads to tooth extraction.

At an initial consultation,
a diagnosis that bone grafting implants are needed
is often given,
and there is a clear reason why
you may hear this kind of diagnosis.
If there is not enough jawbone,
the fixture cannot be placed properly,
and to ensure a good prognosis,
enough alveolar bone (bone) is needed.
Of course, with the endless advancement and development of dentistry,
artificial roots with shorter lengths and greater thickness have been introduced,
but in the case of molars with strong biting force,
a certain level of bone width is still required.
So these are the cases that can be seen as when implant bone grafting is needed.
More specifically, let’s go over when implant bone grafting is needed,
one by one.
I’ll explain using situations that anyone can experience,
so please read comfortably.
When bone loss occurs due to chronic periodontitis
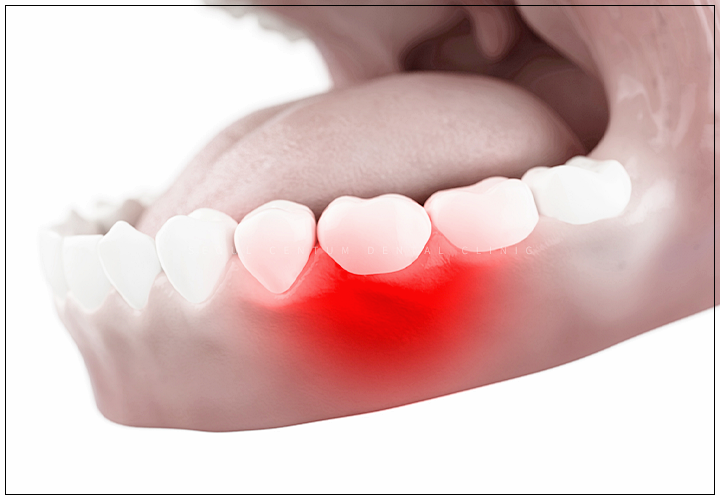
This is one of the cases in which implant bone grafting is needed. Periodontitis is a condition that requires caution because it can become a chronic disease if not handled properly,
and because the pain increases gradually, you may not feel significant discomfort.
If it is not addressed in the early stages, the periodontal pocket deepens, causing the periodontal ligament to swell and become damaged, and the surrounding alveolar bone gradually gets resorbed. If it deepens to 6–7 mm or more, even the jawbone surrounding the tooth can melt away, eventually leading to a decision to extract the tooth.
Even if alveolar bone has been lost extensively, some people try to endure it, but in cases of severe loss, the bone width is not suitable for fixture placement, so bone reconstruction is necessary. (*For bone reconstruction, an appropriate option can be selected from synthetic bone, autogenous bone, xenograft, or allograft.)
If alveolar bone augmentation of 4 mm or less is needed, bone should be filled using a lateral approach; if it is 4 mm or more, bone density can be adjusted using a crestal approach.
When the apical abscess is extensive due to pulpitis
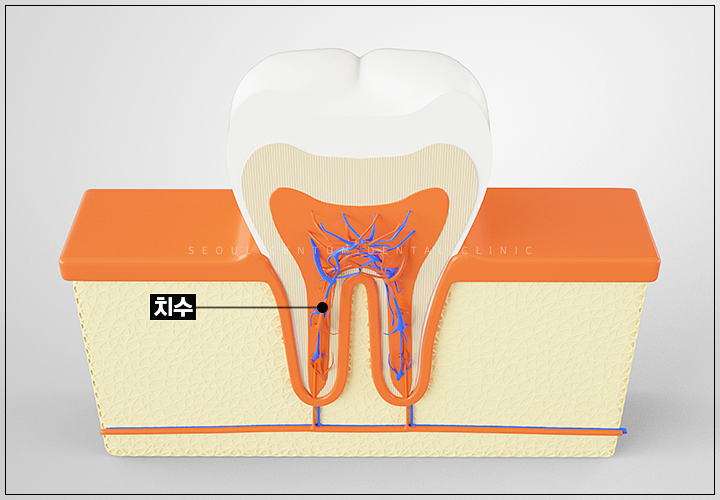
Cavities are a dental lesion that anyone, from children to adults, can experience. When cavities become deep, they cause necrosis in the order of enamel, dentin, and pulp, leading to the formation of a periapical abscess.
A periapical abscess refers to inflammation at the tip of the tooth root, and if the inflammation is extensive, symptoms such as tooth mobility, gum abscess, bleeding, and pressure pain may appear. Depending on the oral environment, the tooth may be saved through root canal treatment, retreatment, or apicoectomy, but if pus has spread to adjacent teeth, extraction followed by implants may ultimately be the best option.
If the contaminated alveolar bone around the root is widespread, it must all be curetted and bone grafting must be performed again.
Since fixtures are usually 8–10 mm products, it is good to prepare a depth of 10 mm and a horizontal bone width of about 10 mm. This is an academically necessary alveolar bone condition, so if the area deviates too much from this range, reconstructing the jawbone through bone grafting is necessary.
When the gums have been resorbed due to long-term denture use
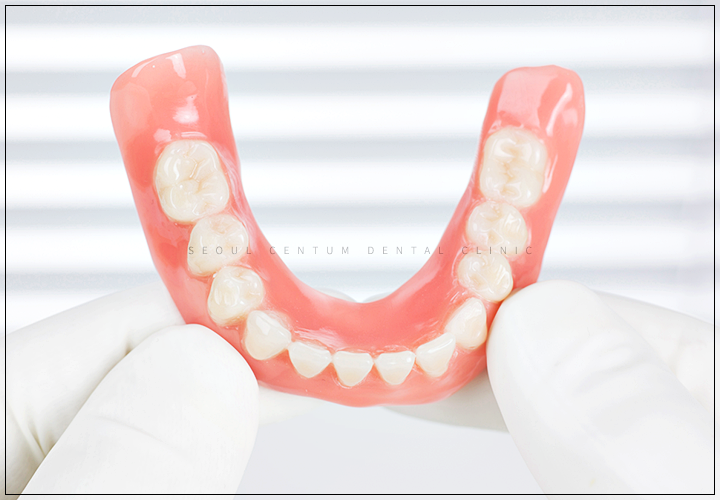
People with edentulism or partial edentulism can restore some of their original tooth function and live using dentures as an alternative.
However, since dentures are devices worn on the gums, it should be kept in mind that the gums gradually diminish.
When the gums lose their function, they eventually shift toward being resorbed. So if denture use continues for a long time, the gums sink down, and when you later want to place implants, you may not meet the alveolar bone 기준, leading to bone grafting.
Because each person’s oral environment is different, you cannot estimate alveolar bone loss purely in proportion to denture-wearing duration, but if, after an accurate examination, there is not enough space to place a fixture, grafting the alveolar bone is the right choice.
When the maxillary sinus membrane has descended
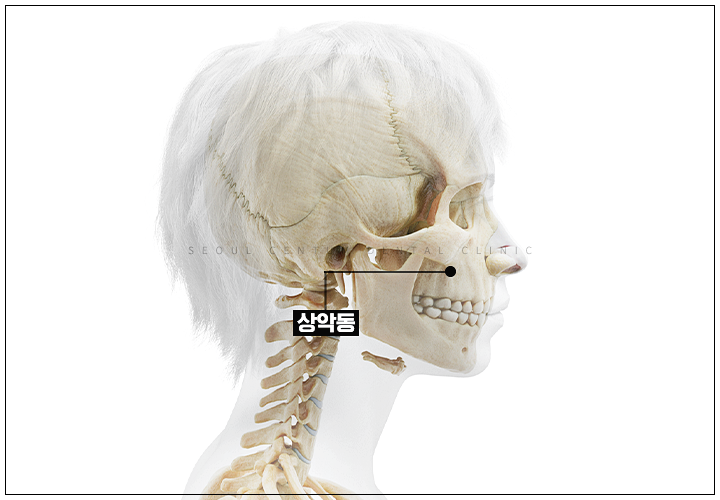
There is a space above the upper teeth called the maxillary sinus. Literally, it means a sinus (cavity) that exists in the maxilla (upper jaw).
If a maxillary molar is extracted and a long period of time passes, the maxillary sinus membrane gradually descends. Then there is not enough space to place an implant.
If a fixture is placed while bone loss has occurred and the maxillary sinus membrane has descended, the maxillary sinus may be perforated, causing secondary side effects such as inflammation, pain, and fever. Therefore, if the loss of an upper molar has been longstanding, the maxillary sinus membrane has descended, and the bone width is insufficient, reconstruction through sinus lift surgery and bone grafting is necessary.
When tooth loss occurs due to aging

As people reach middle age, aging sets in, and not only does the surface of the teeth gradually wear down, but the gums can also naturally weaken and recede. As a result, teeth may become loose, and in severe cases, tooth loss may occur. For this reason, implants are also needed in this case, and if the bone width is insufficient, a bone graft implant may be performed accordingly.
The cases in which implant bone grafting is needed are as described above, so please keep them in mind. Since implants can be used semi-permanently once they are properly placed, I recommend receiving them using the appropriate method. If you have any questions related to the main text, please feel free to leave an inquiry anytime.^^