Hello, I’m Kim Min-young, a restorative dentistry specialist at a dental clinic near Sunyudo Station.
A horizontally impacted wisdom tooth erupts abnormally and often becomes a major cause of threatening the health of the adjacent second molar.
Most patients visit only after symptoms appear,
but by the time pain develops,
it is often already the case that caries in the crown area of the adjacent tooth or distal alveolar bone resorption has progressed.
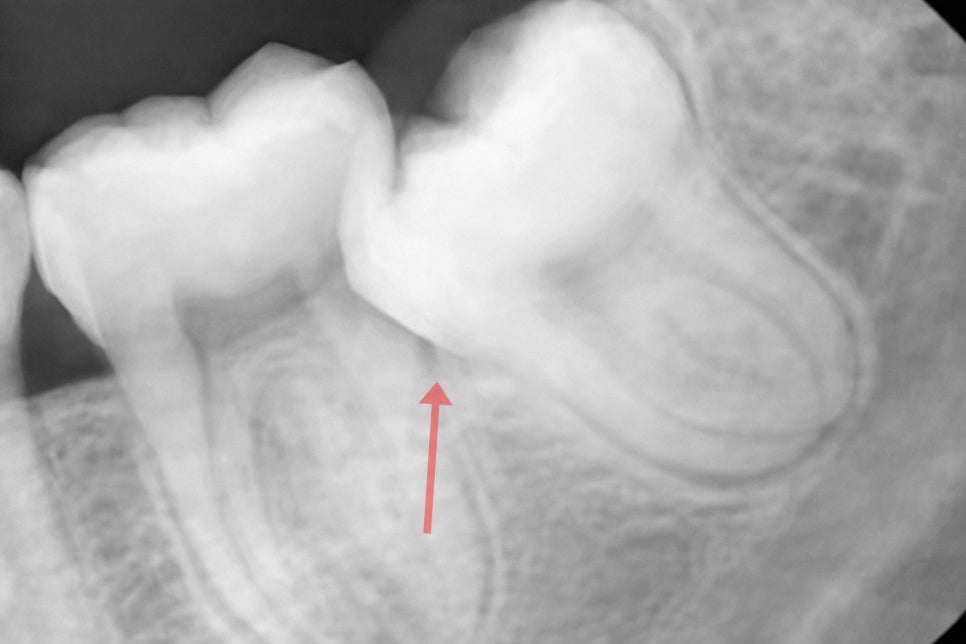
This creates a gap between it and the front molar
that makes it impossible to keep clean,
leading to chronic periodontitis and pericoronitis.
In particular, root resorption and irreversible bone loss
shorten the lifespan of the adjacent tooth itself.
Therefore, from the standpoint of oral health management,
preventive extraction may be necessary.
In this article, we will look at the problems that occur if this is left untreated.
Sunyudo Station Dental Clinic Restorative Dentistry Specialist Kim Min-young
- Anatomical Structure of a Horizontally Impacted Wisdom Tooth
From the stage of dental germ formation, it develops at an abnormal angle,
cannot erupt vertically into the oral cavity,
and lies horizontally toward
the distal surface of the second molar.
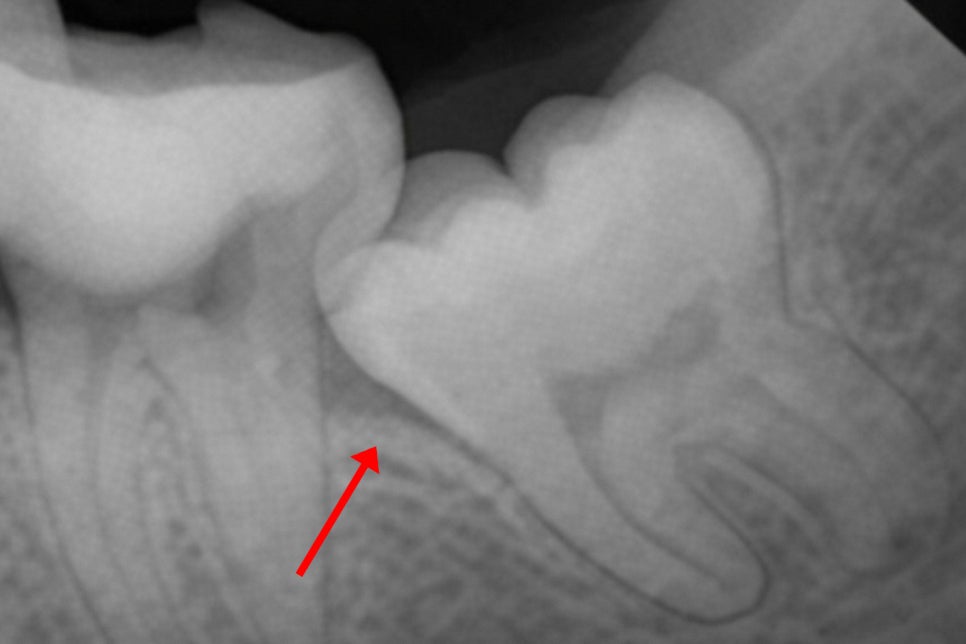
This forms a narrow, deep V-shaped gap
between it and the distal surface of the second molar,
and because this area is difficult to maintain
with brushing or flossing alone,
food debris and bacteria become trapped,
making it a perfect breeding ground for Mutans streptococci
and forming biofilm and hard tartar.
In addition, pericoronitis can occur around the wisdom tooth,
causing chronic inflammation that may lead to pain and bleeding,
and it continuously presses on the root or crown of the second molar,
changing the density of the surrounding bone
and becoming a direct cause of bone loss.
Sunyudo Station Dental Clinic Restorative Dentistry Specialist Kim Min-young
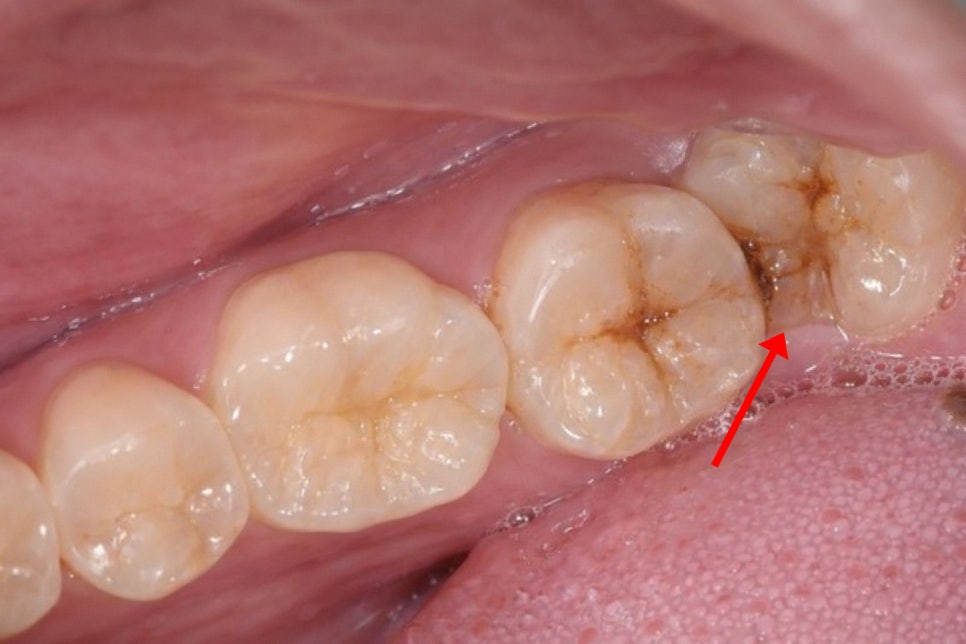
- Distal Caries of the Adjacent Tooth
The most common complication is caries in the adjacent tooth,
which starts on the interproximal surface hidden by the gums.
This area not only lacks self-cleansing by saliva,
but it is also difficult for the patient to see with the naked eye,
and in many cases there is no pain until the caries has deepened close to the root canal.
Therefore, by the time a patient visits because they feel sensitivity or pain,
in most cases infection of the pulp has already progressed.
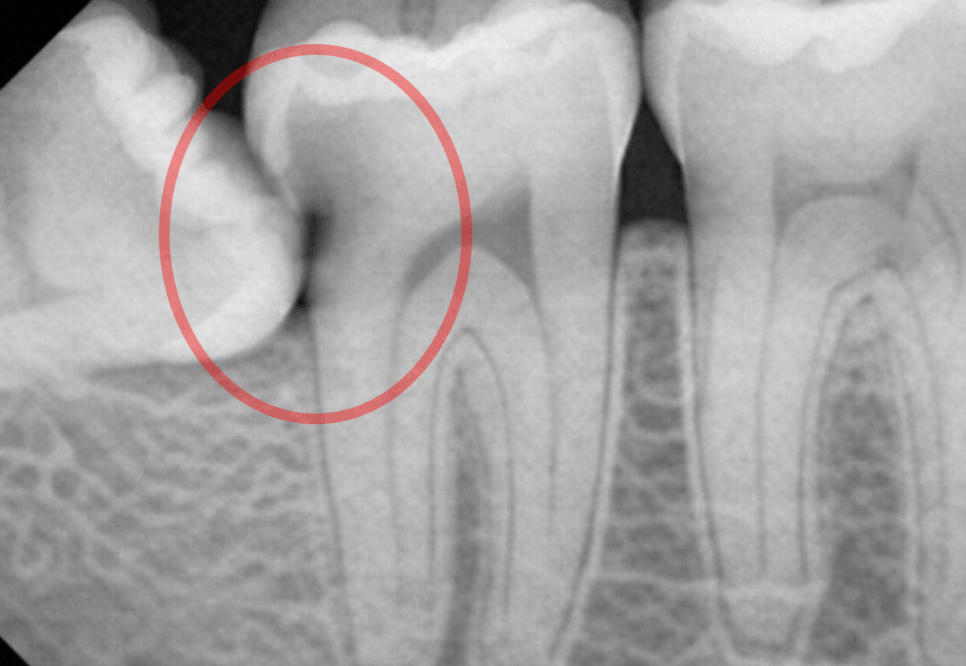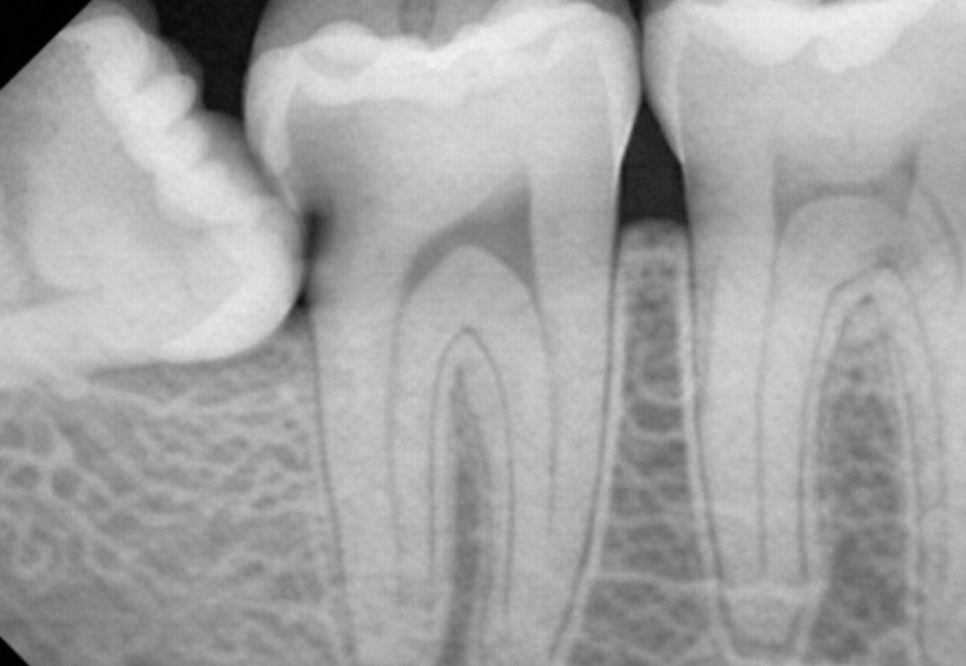
When it is in contact with the root,
it begins near the cementoenamel junction (CEJ)
or on the root surface below it,
where the tissue is softer and thinner than enamel,
making it vulnerable to acid erosion,
and it quickly reaches the pulp along the dentin.
In severe cases, it can ultimately lead to the worst-case scenario
in which even the second molar must be extracted.
Sunyudo Station Dental Clinic Restorative Dentistry Specialist Kim Min-young
- Alveolar Bone Loss and Periodontal Pocket Formation
Along with the pressure caused by continuously compressing the alveolar bone or the root of the front molar,
the osteoclasts activated by pericoronitis dissolve the alveolar bone,
and on X-rays,
a pattern of bone loss appears in which the bone looks dark and radiolucent.
This means that the height of the bone supporting the tooth has decreased.
Pathological periodontal pocket formation
Between a healthy tooth and the gums, there is a shallow groove of about 1–3 mm,
but as inflammation progresses, a deep pathological periodontal pocket of 5–6 mm or more forms.
This provides an anaerobic environment that is ideal for bacterial growth
and can lead to bigger problems.
For these reasons, I recommend preventive extraction in the early 20s,
when the periodontal tissues are healthy
and their regenerative capacity is good.
Sunyudo Station Dental Clinic Restorative Dentistry Specialist Kim Min-young
- External Root Resorption
The root tissue of the front molar
is subjected to physical pressure or a physiological inflammatory response,
and the periodontal ligament is compressed.
During this process, local blood flow is impaired,
and the body’s immune system recognizes this and activates osteoclasts.
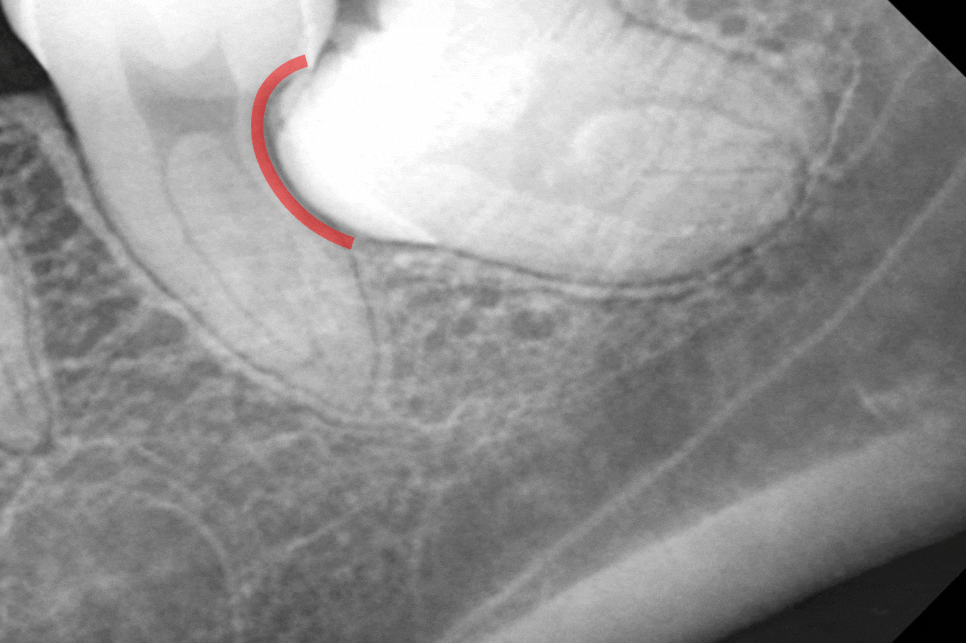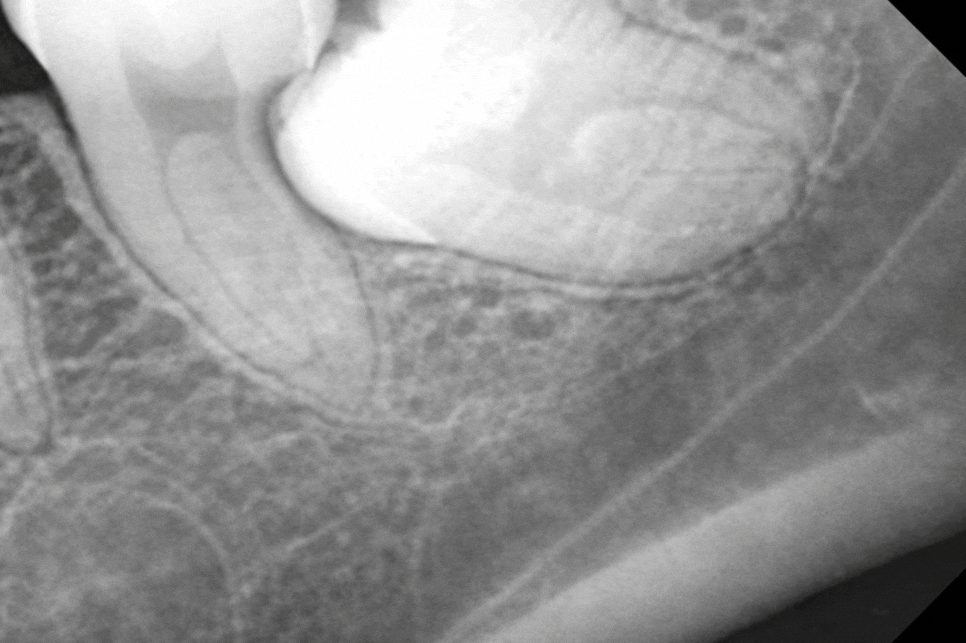
The activated osteoclasts begin to erode the root of the adjacent tooth,
and this gradual dissolution of the root from the outside
is called external resorption.
This shortens the lifespan of the natural tooth
and leads to devastating consequences.
If such signs are detected through a detailed examination,
preventive extraction is recommended
to prevent greater loss.
As we looked at today, a horizontally impacted wisdom tooth is far too costly to leave untreated
simply because it does not hurt right away.
Caries, alveolar bone loss, and root resorption
all leave irreversible damage that is difficult to reverse once they occur.
Therefore, even if you do not have pain right now,
please get a regular checkup.
This has been Kim Min-young,
a restorative dentistry specialist at a dental clinic near Sunyudo Station.




